## Clinical Diagnosis: Septic Shock ### Key Clinical Features Present **Key Point:** This patient exhibits the classic triad of septic shock: hypotension (BP 88/54), evidence of infection (fever, elevated WBC, positive blood cultures pending), and evidence of tissue hypoperfusion (elevated lactate 4.2 mmol/L). ### Pathophysiologic Mechanism **High-Yield:** Septic shock is characterized by: 1. **Distributive shock** — peripheral vasodilation due to inflammatory mediators (TNF-α, IL-1, IL-6, nitric oxide) 2. **Warm shock** — warm, flushed skin with bounding pulses (early phase) due to peripheral vasodilation 3. **Maldistribution of blood flow** — shunting away from vital organs despite normal or increased cardiac output 4. **Microvascular dysfunction** — impaired oxygen extraction at tissue level ### Diagnostic Criteria (qSOFA/SIRS) This patient meets sepsis criteria: - Fever (≥38°C or ≤36°C) - Tachycardia (implied by shock state) - Elevated WBC (18,500/μL) - Suspected source: perforated viscus with peritonitis - Hypotension requiring vasopressor support (implied) - Lactate elevation (4.2 mmol/L) — marker of tissue hypoperfusion ### Shock Types Comparison | Feature | Septic | Cardiogenic | Hypovolemic | Anaphylactic | |---------|--------|-------------|-------------|---------------| | **Skin** | Warm, flushed | Cold, clammy | Cold, clammy | Warm, flushed | | **SVR** | Low | High | High | Low | | **CO** | Normal/High initially | Low | Low | Normal/High | | **Lactate** | Elevated | Elevated | Elevated | Normal/Mildly elevated | | **Cause** | Infection | Pump failure | Blood loss/fluid loss | Allergen exposure | | **WBC** | Elevated | Normal | Normal | Normal | **Clinical Pearl:** The combination of **warm skin + hypotension + fever + elevated lactate + infection source** is pathognomonic for septic shock. The patient's warm, flushed appearance despite shock distinguishes this from cardiogenic and hypovolemic shock, where skin is typically cold and clammy. ### Mnemonic: SEPSIS **S**uspected infection **E**levated lactate or hypotension **P**erfusion abnormality (altered mental status, mottled skin, oliguria) **S**ystemic inflammation (fever, tachycardia, tachypnea) **I**ncreased vasodilation (warm shock) **S**hock state (hypotension unresponsive to fluids) ### Management Implications 1. **Immediate:** Fluid resuscitation (30 mL/kg crystalloid in first 3 hours) 2. **Antibiotics:** Broad-spectrum within 1 hour 3. **Source control:** Surgical intervention for perforation 4. **Vasopressors:** Norepinephrine if hypotension persists after fluids 5. **Lactate clearance:** Monitor as marker of tissue perfusion response [cite:Robbins 10e Ch 4] 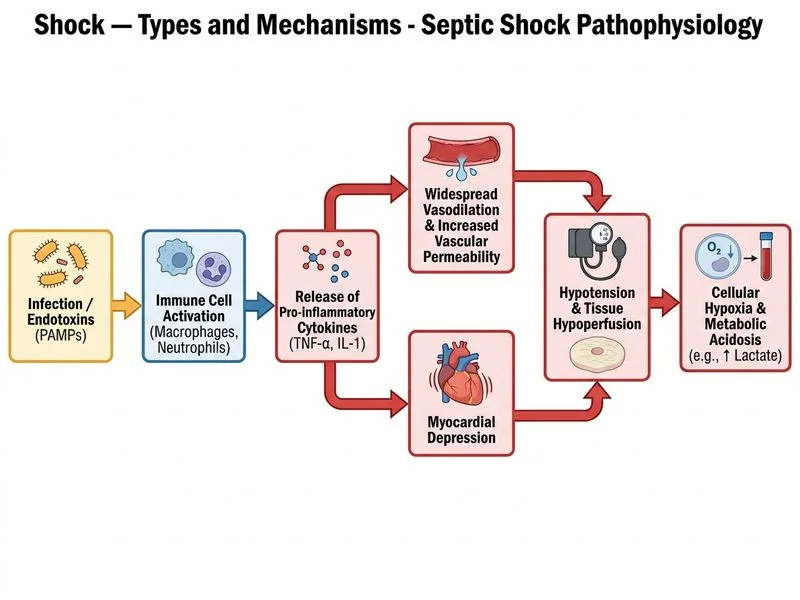
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.