## Clinical Diagnosis: Cardiogenic Shock ### Hemodynamic Profile Analysis **Key Point:** This patient presents with the classic hemodynamic triad of cardiogenic shock: - **Reduced cardiac output:** CO 3.2 L/min (normal 4–8 L/min) - **Elevated pulmonary capillary wedge pressure:** PCWP 28 mmHg (normal 6–12 mmHg) - **Elevated systemic vascular resistance:** SVR 1200 dyne·s·cm⁻⁵ (at upper limit of normal, compensatory) ### Pathophysiologic Mechanism **High-Yield:** Cardiogenic shock results from **pump failure** — the heart cannot generate sufficient cardiac output to meet tissue metabolic demands. #### Sequence of Events in Acute MI 1. **Myocardial infarction** → loss of contractile function 2. **Reduced ejection fraction** → decreased stroke volume 3. **Compensatory mechanisms activate:** - Sympathetic nervous system → increased heart rate, contractility, vasoconstriction - Frank-Starling mechanism → increased preload to optimize contraction 4. **Consequence:** Elevated filling pressures → pulmonary edema (crackles, orthopnea) 5. **Tissue hypoperfusion** → anaerobic metabolism, lactate accumulation, organ dysfunction ### Hemodynamic Classification of Shock ```mermaid flowchart TD A[Shock State]:::outcome --> B{Cardiac Output?}:::decision B -->|Low| C{SVR?}:::decision B -->|High| D[Distributive Shock]:::outcome C -->|High| E[Cardiogenic Shock]:::outcome C -->|Low| F[Septic/Anaphylactic]:::outcome E --> G[MI, HF, Arrhythmia]:::action F --> H[Infection, Allergen]:::action D --> I[Sepsis, Anaphylaxis]:::action ``` ### Shock Types: Hemodynamic Differentiation | Parameter | Cardiogenic | Septic | Hypovolemic | Anaphylactic | |-----------|------------|--------|-------------|---------------| | **CO** | ↓ | ↑ (early) | ↓ | ↑ | | **SVR** | ↑ | ↓↓ | ↑ | ↓↓ | | **PCWP** | ↑↑ | Normal/↓ | ↓ | Normal/↓ | | **Skin** | Cold, clammy | Warm, flushed | Cold, clammy | Warm, flushed | | **Mechanism** | Pump failure | Vasodilation | Volume loss | Vasodilation | | **Lactate** | ↑ | ↑ | ↑ | Normal/↑ | **Clinical Pearl:** The **elevated PCWP (pulmonary edema) + low CO (hypotension) + high SVR (compensatory vasoconstriction)** triad is pathognomonic for cardiogenic shock. The cold, clammy skin reflects sympathetic activation and peripheral vasoconstriction — a key distinguishing feature from distributive shock (warm, flushed). ### Clinical Clues in This Case 1. **Recent anterior MI** — left ventricle damage → reduced contractility 2. **Holosystolic murmur at apex** — suggests acute mitral regurgitation (papillary muscle rupture or ischemia), further reducing effective forward flow 3. **Orthopnea + bilateral crackles** — pulmonary edema from elevated filling pressures 4. **Elevated JVP** — right ventricular involvement or RV afterload from pulmonary edema 5. **Hypotension + reduced CO** — tissue hypoperfusion ### Mnemonic: PUMP FAILURE **P**ressure elevated (PCWP ↑) **U**nderperfusion (low CO, high lactate) **M**yocardial dysfunction (MI, HF, arrhythmia) **P**ulmonary edema (crackles, orthopnea) **F**illing pressures high (elevated JVP, PCWP) **A**ctivated sympathetic system (cold, clammy, tachycardia) **I**ncreased SVR (compensatory) **L**ow cardiac output **U**rgent revascularization or mechanical support needed **R**educed ejection fraction **E**levated lactate (tissue hypoperfusion) ### Management Approach 1. **Inotropes:** Dobutamine or milrinone to improve contractility 2. **Vasopressors:** Norepinephrine if hypotension persists (avoid pure vasodilation) 3. **Diuretics:** Cautiously, to reduce pulmonary edema without worsening renal perfusion 4. **Revascularization:** PCI or CABG for acute MI 5. **Mechanical support:** IABP, ECMO if refractory [cite:Robbins 10e Ch 4; Harrison 21e Ch 330] 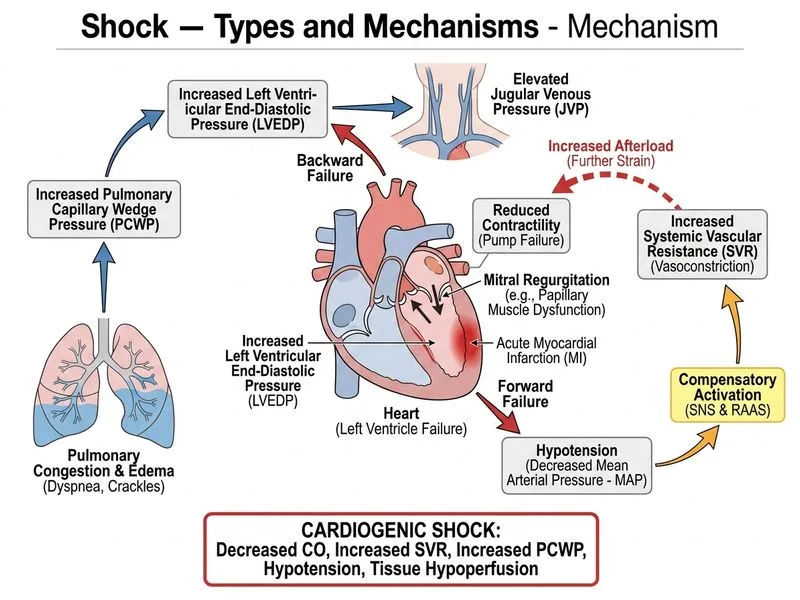
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.