## Diagnosis: Acute Chest Syndrome **Key Point:** Acute chest syndrome (ACS) is a life-threatening pulmonary complication of sickle cell disease characterized by fever, chest pain, dyspnea, and a new infiltrate on chest imaging. ### Clinical Features of ACS - Fever and respiratory symptoms (dyspnea, cough, chest pain) - New pulmonary infiltrate on chest X-ray (not present on prior imaging) - Hypoxemia (SpO₂ < 90% on room air is typical) - Elevated reticulocyte count (reflects ongoing hemolysis) - Occurs in 10–15% of sickle cell patients annually ### Pathophysiology ACS results from: 1. Vaso-occlusion in pulmonary vasculature 2. Fat embolism from bone marrow infarction 3. Infection (bacterial or viral pneumonia) 4. In-situ thrombosis **Clinical Pearl:** ACS can rapidly progress to respiratory failure and is a leading cause of death in sickle cell disease. Immediate management includes oxygen therapy, broad-spectrum antibiotics, and consideration of exchange transfusion if severe. ### Distinguishing Features from Other Crises | Complication | Presentation | Key Finding | | --- | --- | --- | | **Acute Chest Syndrome** | Fever + dyspnea + chest pain | **New pulmonary infiltrate** on imaging | | Splenic Sequestration | Acute abdominal pain, splenomegaly | Massive splenomegaly, rapid Hb drop | | Aplastic Crisis | Pallor, fatigue, dyspnea | **Reticulocytopenia** (low reticulocyte count) | | Acute Stroke | Focal neurologic deficit | Sudden onset hemiparesis/aphasia | **High-Yield:** The combination of **new infiltrate + fever + hypoxemia** in a sickle cell patient is ACS until proven otherwise. Reticulocytosis (not reticulocytopenia) is present because bone marrow is still producing RBCs despite the acute lung pathology. **Mnemonic for ACS triggers:** **FIST** - **F**at embolism (from bone infarction) - **I**nfection (pneumonia) - **S**ickle vaso-occlusion - **T**hrombosis (in-situ) [cite:Robbins 10e Ch 14] 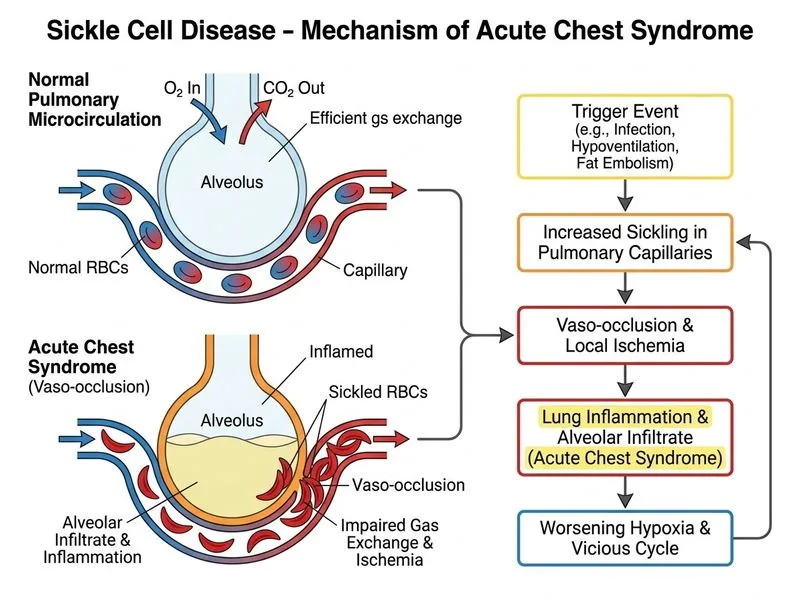
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.