## Clinical Presentation Analysis This patient presents with loss of **fine touch, vibration sense, and proprioception (joint position sense)** while **pain and temperature sensation are preserved**. This is the inverse of dissociated sensory loss and is pathognomonic for **dorsal column (posterior column) involvement**. ### Dorsal Column Anatomy and Function **Key Point:** The dorsal columns consist of two fasciculi: - **Fasciculus gracilis** — carries sensation from lower limbs and lower trunk (medial, enters below T6) - **Fasciculus cuneatus** — carries sensation from upper limbs and upper trunk (lateral, enters above T6) Both carry **fine touch, vibration, and proprioception** via **uncrossed, ipsilateral fibers** that ascend to the medulla. ### Spinal Cord Tract Sensory Modalities | Tract | Modality | Crossing | Spinal Location | Clinical Deficit | |-------|----------|----------|-----------------|------------------| | **Dorsal Columns** | Fine touch, vibration, proprioception | Uncrossed (ipsilateral) | Posterior cord | Loss of fine touch, vibration, proprioception | | **Spinothalamic** | Pain, temperature | Crossed (contralateral) | Anterolateral cord | Loss of pain and temperature | | **Spinocerebellar** | Unconscious proprioception | Mostly uncrossed | Lateral cord | Ataxia, not conscious sensory loss | | **Dorsal Root Entry Zone** | Mixed (all modalities) | Variable | Dorsolateral cord | Segmental sensory loss at entry level | ### Why Dorsal Columns Are Involved 1. **Bilateral, progressive lower limb sensory loss** → suggests a midline or central cord lesion affecting both fasciculi 2. **Selective loss of fine touch, vibration, and proprioception** → these modalities are exclusively carried by dorsal columns 3. **Preserved pain and temperature** → spinothalamic tract is spared (located anterolaterally) 4. **Cervical and upper thoracic lesion on MRI** → can affect fasciculus cuneatus (upper limbs) and fasciculus gracilis (lower limbs) simultaneously 5. **No clear sensory level** → dorsal column lesions often do not produce a sharp sensory level because the tracts ascend over multiple segments **High-Yield:** **Dorsal column disease = loss of fine touch, vibration, proprioception. Spinothalamic disease = loss of pain and temperature.** This is the single most important distinction in spinal cord sensory pathology. ### Clinical Correlation: Likely Diagnosis The progressive bilateral lower limb weakness with dorsal column sensory loss and upper motor neuron signs (hyperreflexia, Babinski) in a 38-year-old woman suggests: - **Multiple sclerosis** (demyelinating disease) - **Subacute combined degeneration** (B12 deficiency) - **Cervical myelopathy** (structural compression) - **Syringomyelia** The T2-hyperintense lesion on MRI is consistent with demyelination (MS) or edema from compression. **Clinical Pearl:** Patients with dorsal column disease often report difficulty walking in the dark or with eyes closed (positive Romberg sign) because they lose proprioceptive feedback and must rely on vision. This is NOT seen in spinothalamic disease. [cite:Standring Anatomy 41e Ch 4; Robbins Pathology 10e Ch 28] 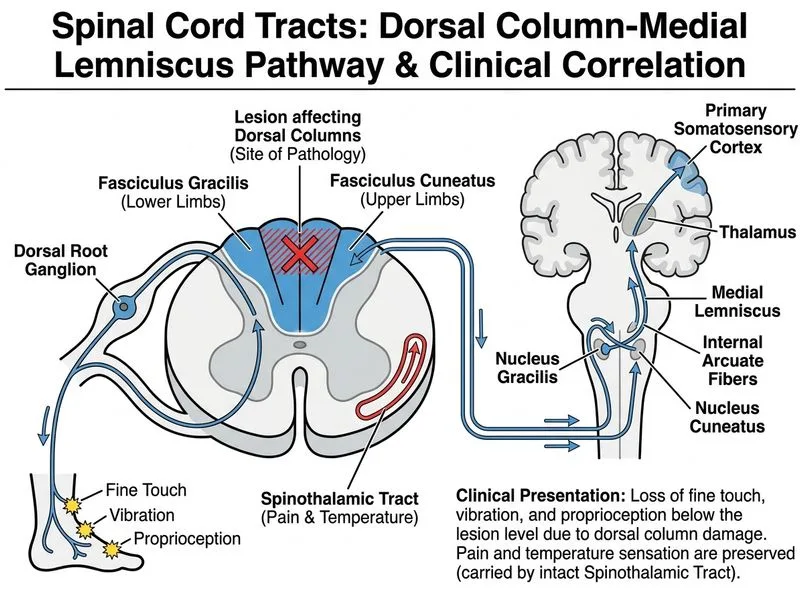
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.