## Clinical Diagnosis: Cauda Equina Syndrome with Cord Involvement The patient presents with **conus medullaris/cauda equina compression**: - **Bilateral leg weakness** → bilateral corticospinal tract involvement - **Bladder dysfunction + decreased anal tone** → sacral parasympathetic and somatic motor involvement (S2–S4 segments) - **Sensory level at T10** → thoracolumbar lesion - **Hyperreflexia** → upper motor neuron signs (cord involvement, not pure cauda equina) ### Anatomical Correlation **Key Point:** The **conus medullaris** (spinal cord termination at L1–L2) and **cauda equina** (nerve roots below) can be compressed by the same lesion. The presence of hyperreflexia (upper motor neuron signs) indicates cord involvement, not pure cauda equina syndrome. **High-Yield:** Cauda equina syndrome is a **neurosurgical emergency** requiring imaging within hours to guide urgent decompression. Delay beyond 48 hours significantly reduces recovery of bowel/bladder function. ## Management Decision Tree ```mermaid flowchart TD A[Cauda equina/conus syndrome suspected]:::outcome --> B{Imaging modality?}:::decision B -->|MRI available| C[Urgent MRI spine with contrast]:::action B -->|MRI unavailable| D[Stat CT spine + myelography]:::action C --> E{Compressive lesion found?}:::decision E -->|Yes: tumor, disc, abscess, hematoma| F[Neurosurgery consultation for decompression]:::action E -->|No: demyelinating/inflammatory| G[High-dose IV methylprednisolone]:::action F --> H[Decompression within 48 hours]:::urgent ``` ### Why MRI Is the Correct First Step 1. **Superior soft-tissue contrast** — identifies cord edema, intramedullary lesions, and compression 2. **Identifies etiology** — disc herniation, tumor, abscess, hematoma, demyelination 3. **Guides urgent intervention** — decompression vs. medical therapy 4. **Non-invasive** — safe in acute settings 5. **Contrast enhancement** — helps identify infection, inflammation, and vascular lesions **Clinical Pearl:** Cauda equina syndrome is one of the few true neurosurgical emergencies. MRI must be obtained **stat** (within 1–2 hours) to determine if urgent decompression is needed. ## Why Other Options Are Incorrect ### Antibiotics Without Imaging - Empirical antibiotics delay diagnosis of non-infectious causes (disc herniation, tumor) - If the lesion is compressive, antibiotics alone will not relieve compression - Imaging must be obtained first to guide treatment ### Corticosteroids Without Imaging - Steroids are contraindicated in spinal epidural abscess (delays drainage) - Steroids do not decompress mechanical lesions - Imaging must identify the etiology before starting steroids ### Plain Radiographs - Plain films have poor sensitivity for soft-tissue pathology (disc, abscess, tumor) - Do not visualize the spinal cord or nerve roots - Delay diagnosis and treatment in a time-sensitive condition - MRI is far superior for evaluating cord and cauda equina compression 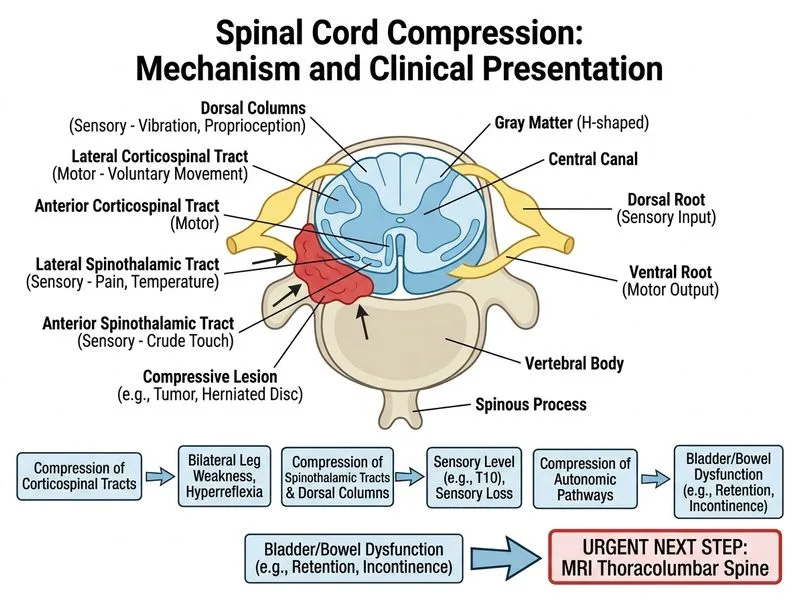
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.