## Clinical Scenario Analysis This patient presents with **acute anterior STEMI** with the following key constraint: - Symptom onset <12 hours ✓ - ST elevation in V1–V4 (anterior wall, LAD territory) - Elevated troponin ✓ - **PCI NOT available within 120 minutes** (3.5-hour transport time) ## Reperfusion Strategy: Fibrinolysis vs. Primary PCI **High-Yield:** When door-to-balloon time exceeds 120 minutes, fibrinolysis is preferred over delayed PCI [cite:Harrison 21e Ch 297]. ```mermaid flowchart TD A[STEMI Diagnosis]:::outcome --> B{Time from symptom onset<br/>< 12 hours?}:::decision B -->|No| C[Medical management]:::action B -->|Yes| D{PCI-capable hospital<br/>available?}:::decision D -->|Yes| E{Door-to-balloon<br/>≤ 120 min?}:::decision D -->|No| F[Fibrinolysis]:::action E -->|Yes| G[Primary PCI]:::action E -->|No| H[Fibrinolysis +<br/>planned rescue PCI]:::action G --> I[Optimal outcome]:::outcome H --> J[Reperfusion achieved<br/>or rescue PCI if failed]:::outcome F --> K[Reperfusion strategy]:::outcome ``` ## Fibrinolytic Agent Selection | Agent | Fibrin-Specificity | Dosing | Advantage | Disadvantage | |-------|-------------------|--------|-----------|---------------| | **Alteplase (tPA)** | High | 15 mg IV bolus, then 0.75 mg/kg over 30 min, then 0.5 mg/kg over 60 min | Lower re-infarction rate | Higher intracranial hemorrhage risk (0.7–1%) | | Streptokinase | Low | 1.5 million units IV over 60 min | Cheaper, lower ICH risk | Higher re-infarction, antigenic | | Reteplase | High | 10 units IV bolus × 2 (30 min apart) | Convenient dosing | Similar to alteplase | **Key Point:** Alteplase is preferred in anterior STEMI due to superior patency rates and lower re-infarction, despite slightly higher ICH risk [cite:Harrison 21e Ch 297]. ## Contraindication Check: Peptic Ulcer Disease **Clinical Pearl:** A history of peptic ulcer disease is **NOT an absolute contraindication** to fibrinolysis, especially if the ulcer is healed and the patient is on PPI therapy (as in this case). The risk of re-bleeding is low and is outweighed by the benefit of myocardial salvage in acute STEMI. **Warning:** Do NOT withhold fibrinolysis in STEMI solely due to remote PUD history. Active bleeding or recent GI bleed would be a contraindication. ## Rescue PCI Strategy **High-Yield:** Rescue PCI is indicated if fibrinolysis fails (defined as <50% ST-segment resolution or ongoing ischemic symptoms at 60–90 minutes post-thrombolysis). The patient should be transferred to a PCI-capable center with this plan in place [cite:ESC STEMI Guidelines 2017]. ## Immediate Management Protocol 1. **Dual antiplatelet therapy:** Aspirin 325 mg + clopidogrel 600 mg (or prasugrel 60 mg) 2. **Fibrinolysis:** Alteplase IV as above 3. **Anticoagulation:** Unfractionated heparin 60–70 units/kg IV bolus, then infusion 4. **Arrange transfer:** To PCI-capable center for rescue PCI if needed 5. **Monitoring:** Serial ECGs, troponin, clinical assessment for reperfusion success 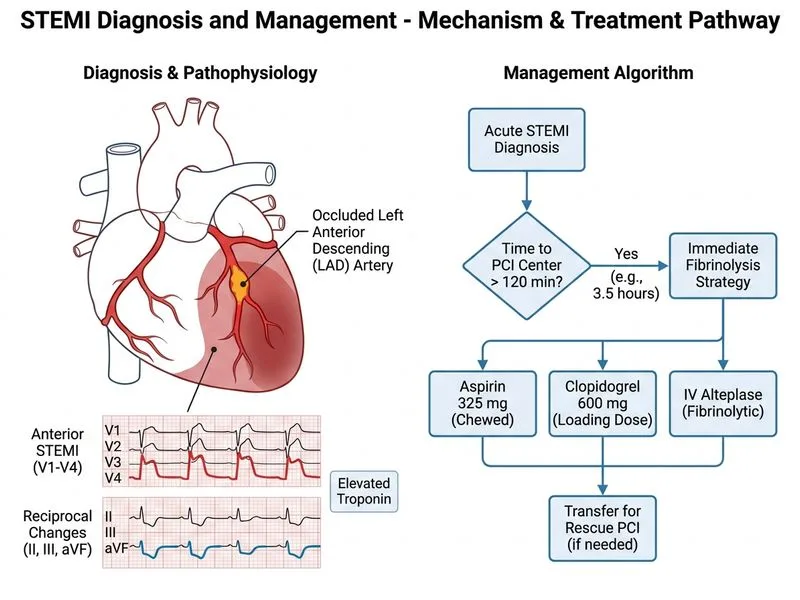
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.