## Clinical Scenario Analysis This is an **inferior wall STEMI** (ST elevation in II, III, aVF with reciprocal changes) presenting within the **fibrinolytic window (< 12 hours)** at a **non-PCI-capable facility**. ## Key Decision Points **Key Point:** When PCI-capable centre is >120 km away with transfer time >2 hours, **fibrinolytic therapy is the guideline-recommended reperfusion strategy** in the absence of contraindications [cite:Harrison 21e Ch 297]. **High-Yield:** The "door-to-balloon" time for primary PCI should be ≤90 minutes. If this cannot be achieved, fibrinolysis within 30 minutes of symptom onset is preferred over delayed PCI. ## Rationale for Correct Answer 1. **Inferior STEMI confirmed** — ST elevation in inferior leads + reciprocal changes + elevated troponin 2. **Fibrinolytic window open** — 2 hours from symptom onset (window extends to 12 hours) 3. **No contraindications evident** — no mention of bleeding history, recent surgery, or stroke 4. **Transfer delay unacceptable** — 2.5-hour transfer would exceed 90-minute PCI door-to-balloon target 5. **Streptokinase is DOC in India** — cost-effective, available at primary centres, Class I recommendation for STEMI ## Dual Antiplatelet Therapy (DAPT) | Agent | Dose | Timing | |-------|------|--------| | Aspirin | 300–325 mg (chewed) | Immediately | | Clopidogrel | 600 mg loading dose | Immediately (before or with fibrinolytic) | | Streptokinase | 1.5 MU IV over 60 min | Within 30 min of first medical contact | **Clinical Pearl:** Combination of aspirin + clopidogrel + fibrinolytic reduces mortality and reinfarction compared to fibrinolytic monotherapy [cite:Harrison 21e Ch 297]. ## Post-Fibrinolysis Management **Key Point:** After fibrinolytic therapy: - Arrange **early transfer** (6–24 hours) for coronary angiography and rescue PCI if fibrinolysis fails - Monitor for reperfusion signs: pain relief, ST resolution, arrhythmias - Continue DAPT, beta-blocker, ACE inhibitor, statin **Mnemonic: FIBRINOLYTIC TIMING — "GOLDEN HOUR" (actually first 3 hours)** - **F**irst medical contact to fibrinolytic: <30 min - **I**nferior/anterior/lateral wall: all eligible - **B**lood pressure stable: can give fibrinolytic - **R**eperfusion assessment: ST resolution, pain relief - **I**nfarction size: smaller with early therapy - **N**o PCI available: fibrinolysis is DOC - **O**ther antiplatelet agents: aspirin + clopidogrel mandatory - **L**ate presentation (>12 hrs): consider conservative management - **Y**ield: 30% mortality reduction vs. no reperfusion - **T**ransfer: arrange early angiography post-fibrinolysis - **I**nhibitors: ACE inhibitor, beta-blocker post-MI - **C**omplex cases: rescue PCI if fibrinolysis fails **Warning:** Do NOT delay fibrinolysis while arranging transfer — "time is myocardium." 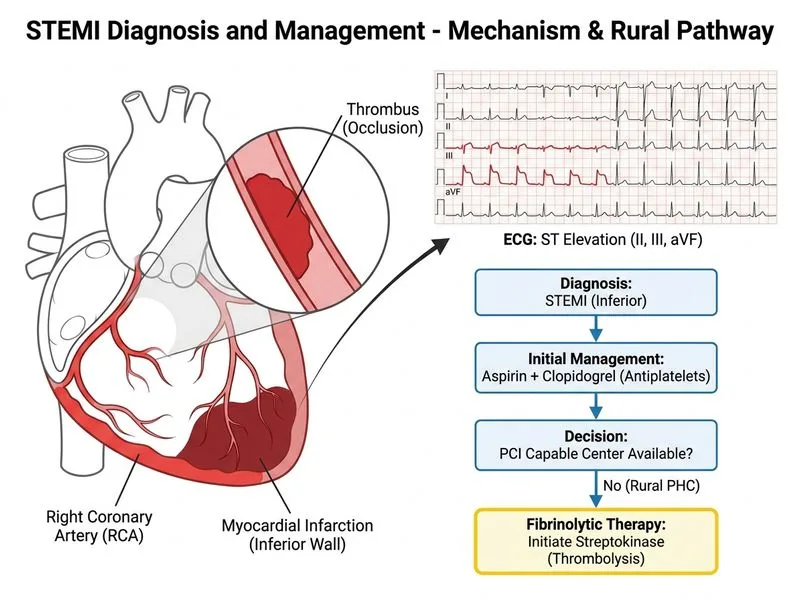
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.