## Nerve Injuries in Supracondylar Fracture: Diagnosis and Management ### Clinical Presentation Analysis **Key Point:** Weakness of **wrist and finger extension** with **intact sensation in the first web space** localizes the injury to the **posterior interosseous nerve (PIN)**, not the anterior interosseous nerve (AIN) or median nerve. ### Anatomical Correlation | Nerve | Motor Function | Sensory | Clinical Test | |-------|---|---|---| | **Posterior Interosseous Nerve (PIN)** | Wrist extension, finger extension (EDC, EIP) | None (purely motor) | Loss of wrist/finger extension | | **Anterior Interosseous Nerve (AIN)** | Thumb IP flexion, index DIP flexion | None (purely motor) | Loss of thumb IP and index DIP flexion | | **Radial Nerve (proximal)** | Wrist extension, finger extension, thumb abduction | Dorsal first web space | Loss of wrist/finger extension + sensory loss | | **Median Nerve** | Wrist/finger flexion, thumb opposition | Lateral palm, thumb, index | Loss of grip, opposition | **High-Yield:** The **first web space sensation is NORMAL** — this rules out radial nerve injury (which causes sensory loss in the dorsal first web space). ### Why PIN and Not AIN? - **PIN injury** → loss of **wrist and finger extension** (EDC, EIP muscles). - **AIN injury** → loss of **thumb IP flexion** and **index DIP flexion** (FPL, FDP-II muscles) — no wrist or finger extension loss. This patient has wrist/finger extension weakness, so **PIN is the diagnosis**. ### Management of Nerve Injuries in Supracondylar Fracture ```mermaid flowchart TD A[Supracondylar fracture + nerve injury]:::outcome --> B{Timing of injury recognition?}:::decision B -->|Immediate post-reduction| C{Nerve type?}:::decision B -->|Delayed discovery| D[Observe 8-12 weeks]:::action C -->|PIN/AIN/Radial| E[Observe 8-12 weeks]:::action C -->|Median/Ulnar| F[Observe 8-12 weeks]:::action E --> G{Recovery at 12 weeks?}:::decision G -->|Yes| H[Full recovery expected]:::outcome G -->|No| I[EMG/NCS + consider exploration]:::action ``` **Clinical Pearl:** Nerve injuries in supracondylar fractures are usually **neurapraxias** (stretch injuries) and recover spontaneously in 80–90% of cases. **Observation for 8–12 weeks is the standard of care** for all nerve injuries in this setting, unless there is: - Nerve transection (rare in closed fractures). - Vascular injury requiring exploration (which may incidentally identify nerve injury). - Failure to recover by 12 weeks (then EMG/NCS and possible exploration). ### Why Observation? 1. Most injuries are stretch-related (neurapraxia), not transection. 2. Spontaneous recovery occurs in >80% by 8–12 weeks. 3. Immediate exploration risks further soft tissue trauma. 4. EMG/NCS at 3 weeks can help prognosticate, but does not change acute management. [cite:Rockwood & Green's Fractures in Adults 9e Ch 11] 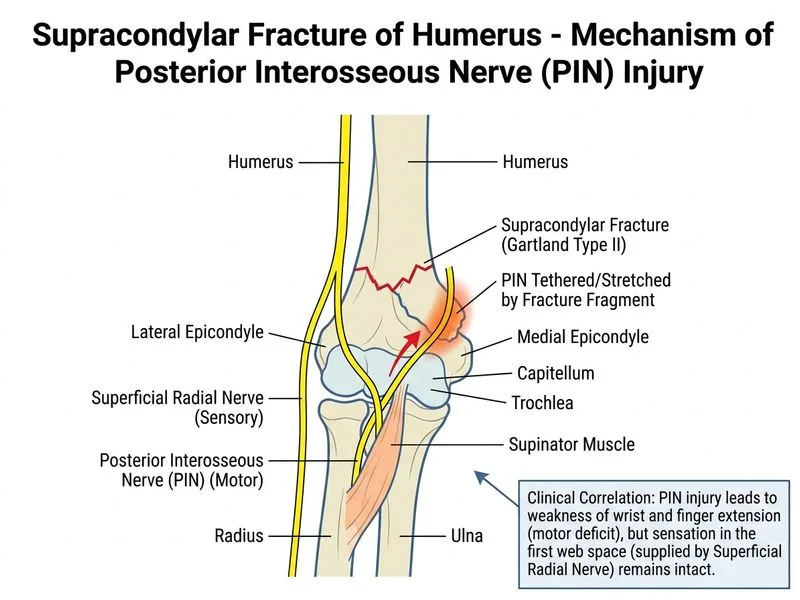
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.