## Pathophysiology of Thrombosis in Diabetes and Hypertension ### Virchow's Triad and Endothelial Dysfunction **Key Point:** Thrombosis results from the interaction of three factors: blood flow abnormality, vessel wall injury, and blood composition changes (Virchow's triad). In this case, endothelial injury is the primary driver. ### Mechanism of Endothelial Damage in Diabetes and Hypertension Chronic hyperglycemia and hypertension cause: 1. **Endothelial dysfunction** — reduced nitric oxide production, increased oxidative stress 2. **Exposure of procoagulant surfaces** — tissue factor (TF) and von Willebrand factor (vWF) are released from damaged endothelium 3. **Atherosclerotic plaque rupture** — chronic hyperglycemia accelerates atherosclerosis; plaque rupture exposes the lipid core (rich in TF) to circulating blood 4. **Platelet activation and aggregation** — vWF binds to exposed collagen and von Willebrand factor receptors on platelets, initiating the coagulation cascade ### Why This Patient Thrombosed The patient's diabetes and hypertension have caused: - Coronary atherosclerosis with lipid-rich plaque - Plaque rupture → exposure of tissue factor - Tissue factor activates the extrinsic coagulation pathway (Factor VII → X → II → fibrin) - Platelet adhesion via vWF-collagen-platelet interactions - Rapid thrombus formation occluding the artery **High-Yield:** The **extrinsic pathway** (tissue factor-dependent) is the primary initiator of thrombosis in atherosclerotic plaque rupture. Tissue factor is the most potent trigger for coagulation in vivo. ### Coagulation Cascade Overview ```mermaid flowchart TD A[Plaque Rupture]:::outcome --> B[Tissue Factor Exposure]:::outcome B --> C[Factor VII Activation]:::action C --> D[Factor X Activation]:::action D --> E[Factor II Activation]:::action E --> F[Thrombin Generation]:::action F --> G[Fibrin Polymerization]:::action G --> H[Thrombus Formation]:::urgent B --> I[Platelet Adhesion via vWF]:::action I --> J[Platelet Aggregation]:::action J --> H ``` **Clinical Pearl:** Acute coronary thrombosis is almost always preceded by atherosclerotic plaque rupture with exposure of the lipid core (tissue factor-rich) to blood. This is why antiplatelet agents (aspirin, P2Y12 inhibitors) and anticoagulants (heparin, warfarin) are both used in acute MI management — they target different pathways of thrombus formation. [cite:Robbins 10e Ch 4] 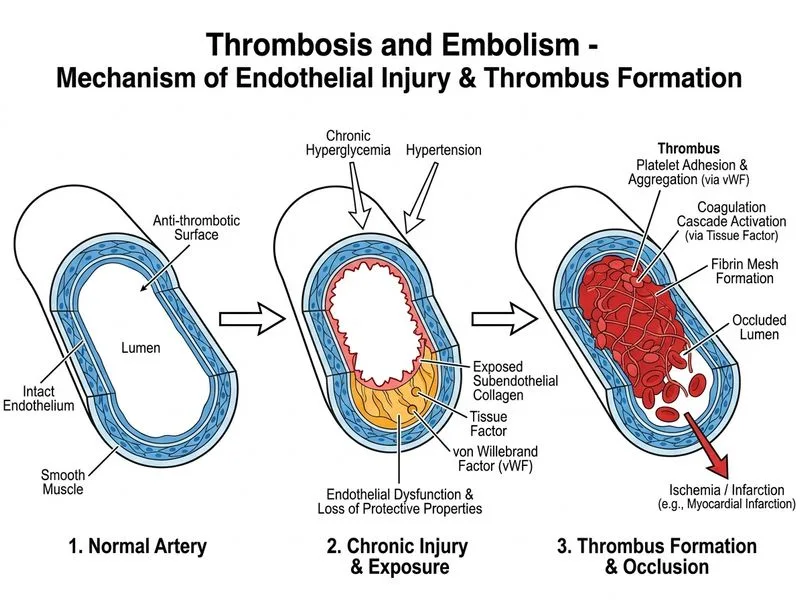
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.