## Cardioembolic Thrombosis in Atrial Fibrillation ### Pathophysiology of AF-Related Thromboembolism **Key Point:** Atrial fibrillation causes blood stasis in the left atrium (especially the left atrial appendage, LAA), which promotes thrombus formation via Virchow's triad: **blood stasis** (abnormal flow), **endothelial injury** (from atrial wall remodeling), and **hypercoagulability** (inflammatory state in AF). ### Why the Left Atrium Thromboses in AF 1. **Loss of atrial contraction** — AF eliminates organized atrial systole, causing blood to pool in the LA and LAA 2. **Reduced flow velocity** — stagnant blood in the LAA has flow velocities <0.4 m/s, promoting thrombus formation 3. **Endothelial remodeling** — chronic AF causes atrial wall inflammation, fibrosis, and endothelial dysfunction 4. **Hypercoagulability** — AF is associated with elevated D-dimer, fibrinogen, and markers of inflammation 5. **Thrombus formation** — typically in the LAA (90% of cases), but can occur throughout the LA ### Acute Arterial Occlusion Presentation The classic **6 Ps of acute limb ischemia**: - **Pain** — sudden onset left leg pain - **Pallor** — pale, white leg - **Pulselessness** — absent femoral pulse - **Paralysis** — left leg paralyzed (motor deficit from ischemia) - **Paresthesia** — sensory changes (not explicitly mentioned but implied) - **Perishing cold** — coldness of the limb **High-Yield:** **Cardioembolic sources account for ~80% of acute arterial occlusions in the lower extremity.** The most common cardiac source is atrial fibrillation, followed by acute MI with mural thrombus, dilated cardiomyopathy, and prosthetic valves. ### Differential Diagnosis of Acute Arterial Occlusion | Feature | Cardioembolic (AF) | Atherosclerotic Thrombosis | Paradoxical Embolism | |---------|-------------------|---------------------------|----------------------| | **Onset** | Sudden | Gradual (claudication) then acute | Sudden | | **Source** | LA thrombus from AF | Plaque rupture in situ | Venous thrombus through PFO | | **Presentation** | No prior claudication | Often prior claudication | Associated with DVT/PE history | | **Prevalence** | Most common | Second most common | Rare in lower extremity | | **Clinical clue** | Known AF, no anticoagulation | Atherosclerotic risk factors | Recent immobility, DVT signs | ### Why This Patient Has Cardioemboli This 72-year-old woman has: - **Chronic AF** (high-risk arrhythmia for thromboembolism) - **No anticoagulation** (no warfarin or DOAC) — major risk factor - **Sudden onset** of limb ischemia (classic for embolism, not in-situ thrombosis) - **No prior claudication** (rules out chronic atherosclerotic disease) **Clinical Pearl:** Patients with AF have a 4–5-fold increased stroke risk and similar risk for peripheral arterial embolism. The CHA₂DS₂-VASc score is used to stratify stroke risk and guide anticoagulation decisions. A score ≥1 in men and ≥2 in women warrants anticoagulation. ### Acute Limb Ischemia Management Algorithm ```mermaid flowchart TD A[Acute Limb Ischemia]:::outcome --> B{Viable or Viable-Threatened?}:::decision B -->|Immediately threatened| C[Emergent Revascularization]:::urgent C --> D{Embolus or Thrombosis?}:::decision D -->|Embolus| E[Embolectomy]:::action D -->|Thrombosis| F[Thrombolysis or Bypass]:::action B -->|Irreversible| G[Amputation]:::urgent E --> H[Anticoagulation + Treat Source]:::action F --> H ``` **Mnemonic:** **ABCD of acute limb ischemia** — **A**cute onset, **B**lue/pale limb, **C**old limb, **D**iagnose with Doppler/angiography. [cite:Robbins 10e Ch 4; Harrison 21e Ch 243] 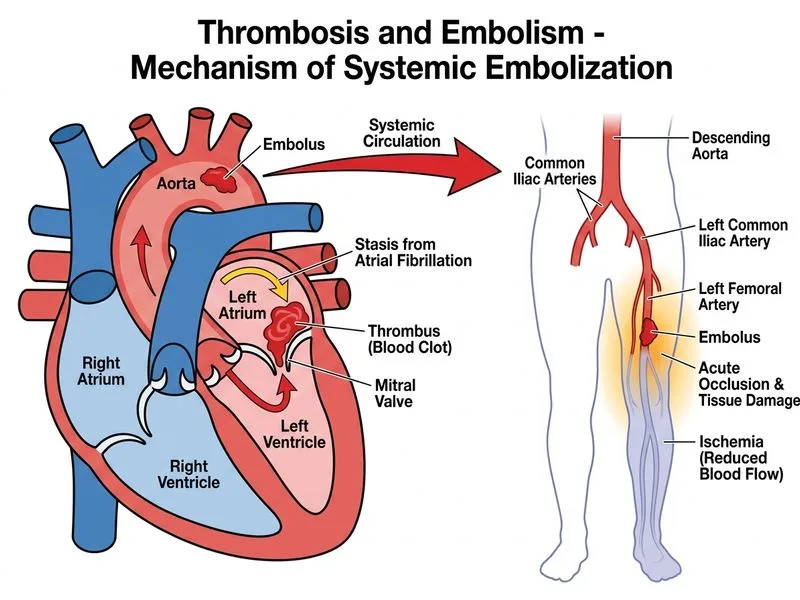
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.