## Investigation of Choice for Metastasis Detection in Thyroid Cancer **Key Point:** Whole body radioactive iodine scan (I-131 scan) after TSH stimulation is the gold standard for detecting radioactive iodine-avid metastases in differentiated thyroid cancer (DTC) before radioactive iodine therapy. ### Clinical Context: Follicular Thyroid Cancer with Capsular Invasion The histology describes **follicular thyroid carcinoma (FTC)** with capsular invasion but no vascular invasion. This represents **minimally invasive FTC**, which has intermediate malignant potential and risk of distant metastases (especially bone and lung). ### Why I-131 Scan is the Investigation of Choice 1. **Functional imaging** — detects iodine-avid metastases (thyroid follicular cells concentrate iodine) 2. **High sensitivity for DTC metastases** — 85–90% sensitivity for radioactive iodine-avid lesions [cite:Robbins 10e Ch 24] 3. **Guides radioactive iodine therapy** — identifies patients who will benefit from I-131 ablation 4. **Standardized protocol** — TSH stimulation (levothyroxine withdrawal or recombinant TSH) increases iodine uptake by residual thyroid tissue and metastases 5. **Therapeutic and diagnostic** — the same I-131 dose used for imaging can treat metastases ### TSH Stimulation Protocol **High-Yield:** TSH must be elevated (>30 mIU/L) to maximize iodine uptake by thyroid cells and metastases: - **Levothyroxine withdrawal** — discontinue for 4–6 weeks (hypothyroid state) - **Recombinant human TSH (rhTSH)** — faster alternative, given as intramuscular injections over 3 days, no hypothyroid symptoms ### Comparison of Imaging Modalities | Investigation | Sensitivity | Specificity | Role in DTC | |---|---|---|---| | **I-131 scan (TSH-stimulated)** | 85–90% | High | Gold standard for radioactive iodine-avid metastases | | **FDG-PET** | 60–80% | Moderate | Detects poorly differentiated/dedifferentiated metastases (I-131 non-avid) | | **Chest X-ray** | 40–60% | Moderate | Detects pulmonary metastases >5 mm; insensitive for small lesions | | **Abdominal ultrasound** | 70–80% | Moderate | Good for hepatic metastases; operator-dependent | | **Serum thyroglobulin** | Variable | High | Marker of disease burden, not localization | **Clinical Pearl:** In poorly differentiated or anaplastic thyroid cancer, metastases may be I-131 non-avid; in these cases, FDG-PET is more sensitive. However, this patient has minimally invasive FTC, which typically retains iodine-avidity. ### Role of Serum Thyroglobulin **Warning:** Serum thyroglobulin is a **tumor marker**, not an imaging investigation. It indicates disease burden and recurrence risk but does NOT localize metastases. It is measured after thyroidectomy and TSH stimulation but cannot replace imaging. ### Management Algorithm Post-Thyroidectomy ```mermaid flowchart TD A[Thyroidectomy for FTC with capsular invasion]:::outcome --> B[TSH stimulation]:::action B --> C[Serum thyroglobulin measurement]:::action C --> D{Thyroglobulin elevated?}:::decision D -->|Yes| E[I-131 scan TSH-stimulated]:::action D -->|No| F[Consider I-131 ablation based on risk]:::action E --> G{Metastases detected?}:::decision G -->|Yes| H[Radioactive iodine therapy]:::action G -->|No| I[Follow-up imaging & thyroglobulin monitoring]:::action ``` **Mnemonic:** **I-131-SCAN** — Iodine-131 Scan for Characterization And Nuclide therapy in differentiated thyroid cancer. 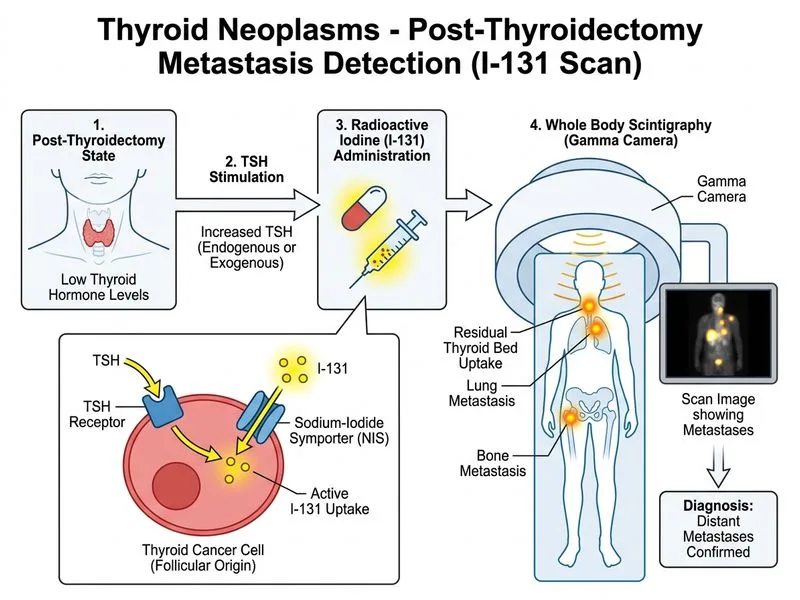
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.