## Diagnosis: Papillary Carcinoma of Thyroid ### Clinical Presentation The patient presents with a firm, fixed thyroid nodule with cervical lymphadenopathy—classic for papillary carcinoma (PTC), the most common thyroid malignancy (70–80% of all thyroid cancers). ### FNAC Findings The cytological hallmark of PTC includes: - **Papillary architecture** with branching fronds - **Nuclear grooves** (coffee-bean appearance) — pathognomonic - **Intranuclear pseudoinclusions** — cytoplasm invaginating into the nucleus - **Psammoma bodies** — calcified, concentric lamellae (present in ~40% of cases) **Key Point:** These nuclear features (grooves + pseudoinclusions) are diagnostic of PTC and distinguish it from other thyroid malignancies. ### Prognostic Features | Feature | Significance | |---------|-------------| | Firm, fixed nodule | Suggests extrathyroidal extension | | Cervical lymphadenopathy | Regional nodal metastasis (does NOT worsen prognosis significantly) | | Euthyroid TSH | PTC does not typically cause hyperthyroidism | | Age 42 years | Intermediate risk; age >45 is higher risk | **High-Yield:** PTC has the best prognosis among thyroid malignancies (10-year survival ~90%), even with lymph node metastases, because it grows slowly and is radiosensitive. ### Pathological Classification **Key Point:** PTC is classified as a **differentiated thyroid carcinoma** (DTC) and retains the ability to take up radioactive iodine (RAI), making it amenable to radioiodine therapy post-thyroidectomy. ### Management Implications 1. Total thyroidectomy with central compartment lymph node dissection 2. Radioactive iodine ablation (if high-risk features present) 3. TSH suppression therapy with levothyroxine 4. Long-term surveillance with TSH and thyroglobulin levels 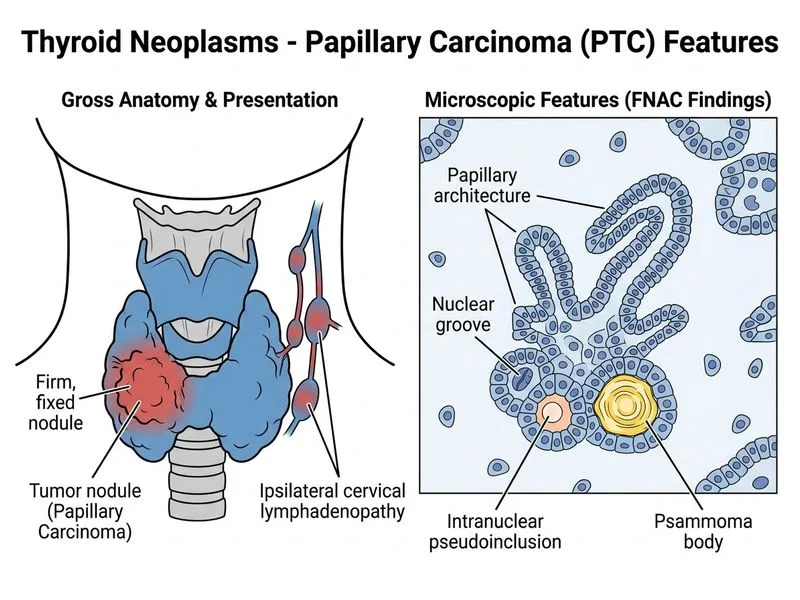
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.