## Diagnosis: Trachoma — Active Infection ### Clinical Presentation This child presents with classic features of trachoma caused by **Chlamydia trachomatis** (serovars A, B, Ba, C): - **Epidemiology:** Rural Rajasthan — an endemic region with poor sanitation and hygiene - **Age:** School-age child (peak transmission age group) - **Duration:** Chronic, recurrent course (6 months) - **Symptoms:** Mild discharge, photophobia - **Signs:** Conjunctival injection, mucoid discharge, **fine linear scars on upper tarsal conjunctiva** ### Diagnostic Confirmation **Giemsa staining showing intracytoplasmic inclusion bodies** confirms *Chlamydia trachomatis* infection. These basophilic inclusions (Halberstaedter–Prowazek bodies) are found within conjunctival epithelial cells and are pathognomonic for chlamydial infection. ### WHO Classification of Trachoma (Thylefors Grading) | Stage | Clinical Features | |-------|------------------| | **TF** | ≥5 follicles on upper tarsal conjunctiva (active infection) | | **TI** | Papillary hypertrophy, diffuse intense inflammation | | **TS** | Linear/Arlt's scars on upper tarsal conjunctiva (fibrosis) | | **TT** | Trichiasis — inturned eyelashes | | **CO** | Corneal opacity from repeated scarring | **Important staging note:** The presence of **fine linear scars on the upper tarsal conjunctiva** technically corresponds to the **TS (Trachomatous Scarring)** stage in the WHO grading system, indicating prior or ongoing chronic infection. In clinical practice, active infection (TF/TI) and early scarring (TS) frequently coexist in endemic settings, especially in children with recurrent disease. The Giemsa-confirmed intracytoplasmic inclusions confirm ongoing active *Chlamydia trachomatis* infection superimposed on early scarring — a mixed TF+TS presentation. The overall diagnosis remains **trachoma**, which is the only option consistent with all findings. ### Why Other Options Are Wrong - **Adenoviral keratoconjunctivitis:** Acute onset, follicles predominantly on *bulbar* (not tarsal) conjunctiva, preauricular lymphadenopathy, NO intracytoplasmic inclusions on Giemsa - **Allergic conjunctivitis:** Bilateral itching, papillae (not follicles), eosinophils on smear, no inclusion bodies - **Staphylococcal bacterial conjunctivitis:** Purulent discharge, gram-positive cocci on smear, no intracytoplasmic inclusions, no tarsal scarring ### Pathophysiology 1. *C. trachomatis* infects columnar conjunctival epithelium → intracytoplasmic inclusions 2. Chronic inflammation → follicle formation on upper tarsal conjunctiva 3. Repeated infection → progressive fibrosis → **Arlt's line** (horizontal scar on upper tarsal conjunctiva) 4. Advanced disease → trichiasis, entropion, corneal pannus → blindness **High-Yield:** Trachoma is the **leading infectious cause of preventable blindness worldwide** (WHO). The **Arlt's line** (linear scar on upper tarsal conjunctiva) is pathognomonic for trachomatous scarring. ### Treatment (SAFE Strategy — WHO) - **S**urgery: For trichiasis/entropion - **A**ntibiotics: Azithromycin 20 mg/kg single dose (community-wide); topical tetracycline 1% ointment BD × 6 weeks - **F**acial cleanliness - **E**nvironmental improvement **Clinical Pearl:** Per *Khurana's Comprehensive Ophthalmology* and *Park's Textbook of Preventive and Social Medicine*, the combination of tarsal conjunctival scarring + Giemsa-confirmed intracytoplasmic inclusions in a child from an endemic region is diagnostic of trachoma, regardless of the precise WHO stage. 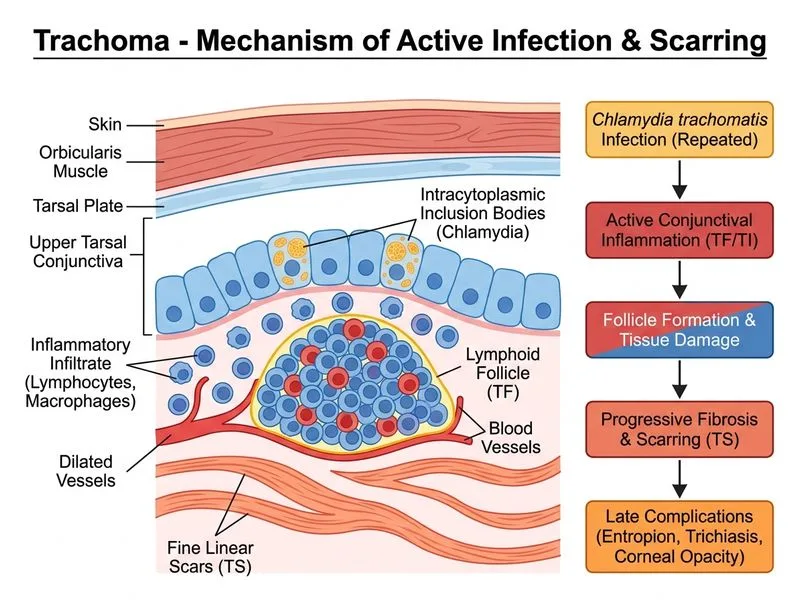
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.