## HPV Testing in Cervical Cancer: Diagnostic and Prognostic Role ### Clinical Context This patient has histologically confirmed invasive cervical cancer (SCC). HPV testing, particularly for high-risk types (16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 66, 68), provides critical information beyond diagnosis. ### Role of HPV Testing in Cervical Cancer **Key Point:** HPV is the causative agent in >99% of cervical cancers. HPV testing in confirmed cervical cancer serves multiple purposes: | Role | Clinical Significance | Application | |------|----------------------|-------------| | **Etiology confirmation** | Identifies causative agent | Establishes HPV-driven pathogenesis | | **Prognostication** | HPV+ status associated with better prognosis in early-stage disease | Guides treatment intensity | | **Treatment response** | HPV+ tumors show better response to chemoradiation | Predicts treatment efficacy | | **Follow-up surveillance** | HPV DNA clearance post-treatment indicates good response | Detects recurrence early | | **Immunotherapy selection** | HPV+ status may predict response to checkpoint inhibitors | Emerging therapeutic target | **High-Yield:** HPV-positive cervical cancers (especially types 16/18) have: - Better prognosis in early-stage disease (paradoxically) - Higher response rates to chemoradiation - Better 5-year survival compared to HPV-negative cancers - Potential for immunotherapy (pembrolizumab approved for recurrent/metastatic HPV+ cervical cancer) ### Diagnostic vs. Prognostic Role **Clinical Pearl:** While HPV testing is NOT the primary diagnostic tool (histology is), it provides essential prognostic and therapeutic information: - **Diagnosis:** Confirmed by cervical biopsy showing invasive SCC (as in this case) - **HPV testing:** Confirms causative agent, guides treatment decisions, and predicts response ### HPV Testing in Different Clinical Scenarios ```mermaid flowchart TD A[Cervical Lesion]:::outcome --> B{Histology confirms cancer?}:::decision B -->|No| C[Screening/surveillance with HPV]:::action B -->|Yes| D[HPV testing for prognosis & treatment]:::action D --> E{HPV 16/18 positive?}:::decision E -->|Yes| F[Better prognosis, consider immunotherapy]:::action E -->|No| G[HPV+ other types or HPV-negative]:::outcome G --> H[Risk stratify, plan adjuvant therapy]:::action ``` **Key Point:** In this patient with confirmed invasive cervical cancer, HPV 16/18 positivity indicates: - Aggressive tumor biology but paradoxically better treatment response - Eligibility for checkpoint inhibitor therapy (pembrolizumab) if recurrent/metastatic - Need for close follow-up with HPV DNA monitoring post-treatment ### Screening vs. Diagnostic HPV Testing **Warning:** ~~HPV testing is only for screening~~ — this is outdated. HPV testing has expanded roles: - **Screening:** Primary HPV testing in asymptomatic women (age 25–65) - **Triage:** HPV testing in women with abnormal cytology - **Diagnostic:** Confirms HPV status in confirmed cervical cancer - **Prognostication:** Predicts treatment response and survival - **Surveillance:** Detects recurrence post-treatment **Mnemonic: HPV ROLES in Cervical Cancer** - **R**isk stratification (prognosis) - **O**utcome prediction (treatment response) - **L**ong-term surveillance (recurrence detection) - **E**ligibility for immunotherapy - **S**tratification for adjuvant therapy [cite:Robbins 10e Ch 19; NCCN Cervical Cancer Guidelines 2023] 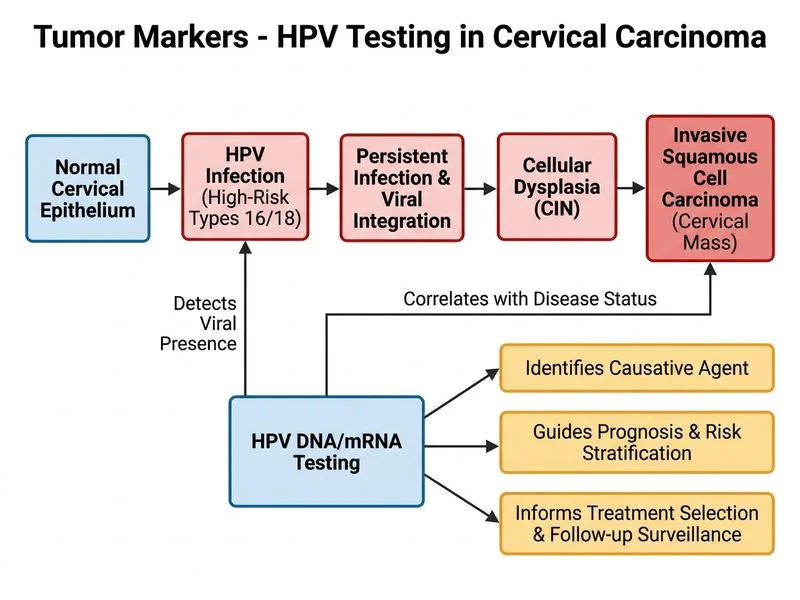
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.