## Clinical Presentation and Diagnosis **Key Point:** OTC deficiency is the most common urea cycle disorder (40–50% of all cases) and presents with hyperammonemia, encephalopathy, and markedly elevated urinary orotic acid. ### Pathophysiology of OTC Deficiency 1. **Enzyme defect:** Ornithine transcarbamylase catalyzes the condensation of carbamoyl phosphate and ornithine to form citrulline — the second step of the urea cycle. 2. **Consequence of block:** Carbamoyl phosphate accumulates and is shunted into the pyrimidine synthesis pathway, causing massive orotic acid production and urinary excretion. 3. **Ammonia accumulation:** Without citrulline formation, the urea cycle stalls, ammonia cannot be incorporated into urea, and hyperammonemia ensues. ### Why Elevated Urotic Acid is Diagnostic **High-Yield:** Elevated urinary orotic acid is **pathognomonic** for OTC deficiency among urea cycle disorders. This distinguishes it from other defects: | Urea Cycle Defect | Urinary Orotic Acid | Key Plasma Finding | |---|---|---| | OTC deficiency | **Markedly elevated** | ↑ Glutamine, ↑ Alanine, ↑ Ammonia | | CPS I deficiency | Normal or low | ↑ Ammonia, normal orotic acid | | Argininosuccinate lyase deficiency | Normal | ↑ Argininosuccinate | | Argininosuccinate synthetase deficiency | Normal | ↑ Citrulline | **Clinical Pearl:** The neonatal presentation (day 3 of life) with poor feeding, lethargy, hypotonia, and respiratory alkalosis with metabolic acidosis is classic for severe hyperammonemia in a urea cycle defect. The markedly elevated ammonia (280 µmol/L) and normal liver function tests rule out hepatic encephalopathy. **Mnemonic:** **COAT** — Carbamoyl phosphate accumulates → Orotic acid elevated → Ammonia toxic → Transcarbamylase (OTC) deficiency. ### Inheritance and Severity - **X-linked recessive inheritance** (males more severely affected). - Heterozygous females may present later with milder symptoms triggered by infection, high protein intake, or pregnancy. - Neonatal-onset (as in this case) indicates severe deficiency with poor prognosis without immediate intervention. ### Management 1. **Acute:** Hemodialysis or continuous venovenous hemofiltration to remove ammonia. 2. **Chronic:** Protein restriction, arginine supplementation (bypasses the block), and sodium benzoate or sodium phenylbutyrate (alternative pathway for nitrogen disposal). 3. **Genetic counseling:** X-linked inheritance; prenatal diagnosis available. [cite:Robbins 10e Ch 7] 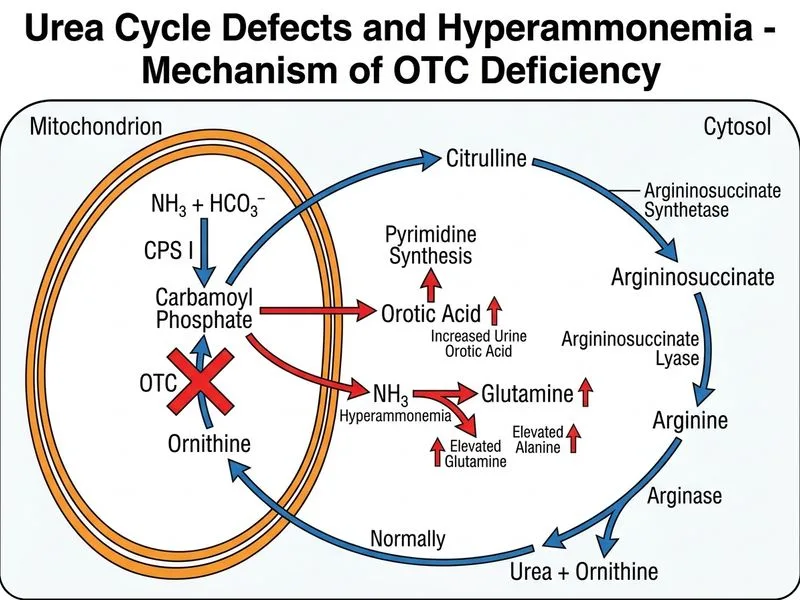
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.