## Diagnosis: Citrullinemia Type I **Key Point:** Citrullinemia type I is caused by argininosuccinate synthetase (ASS) deficiency and presents with markedly elevated plasma citrulline (>1000 µmol/L) combined with hyperammonemia and normal or low argininosuccinate — a pathognomonic biochemical triad. ### Pathophysiology of Argininosuccinate Synthetase Deficiency ```mermaid flowchart TD A[Carbamoyl phosphate + Ornithine]:::action --> B[Citrulline]:::outcome B --> C[Citrulline + Aspartate]:::action C --> D{ASS enzyme present?}:::decision D -->|Yes| E[Argininosuccinate]:::outcome D -->|No| F[Citrulline accumulates]:::urgent F --> G[Hypercitrullinemia]:::outcome F --> H[Urea cycle blocked]:::urgent H --> I[Hyperammonemia]:::urgent E --> J[Arginine + Fumarate]:::outcome ``` ### Biochemical Hallmarks | Feature | Citrullinemia Type I | OTC Deficiency | CPS I Deficiency | |---|---|---|---| | **Plasma citrulline** | **Markedly ↑↑ (>1000 µmol/L)** | Normal/low | Low/absent | | **Plasma ammonia** | ↑↑ (200–500 µmol/L) | ↑↑ | ↑↑ | | **Argininosuccinate** | Low/undetectable | Normal | Normal | | **Urinary orotic acid** | Normal | **Markedly elevated** | Normal/low | | **Inheritance** | Autosomal recessive | X-linked recessive | Autosomal recessive | **High-Yield:** The combination of **hypercitrullinemia + hyperammonemia + normal/low argininosuccinate** is diagnostic for citrullinemia type I. This patient's plasma citrulline of 1200 µmol/L is pathognomonic. ### Clinical Presentation **Mnemonic:** **CITRULLINE** — Citrulline ↑↑, Immune deficiency (recurrent infections), Tubulopathy (renal tubular dysfunction), Recurrent hyperammonemic crises, Urea cycle block, Liver involvement (hepatomegaly), Lethargy/encephalopathy, Intellectual disability (if untreated), Neonatal or infantile onset, Encephalopathy (acute). - **Neonatal-onset form:** Severe hyperammonemia within first week of life; poor prognosis without treatment. - **Late-infantile form (this case):** Presents at 6 months to 2 years with developmental delay, recurrent encephalopathy triggered by protein intake, infection, or stress. - **Protein sensitivity:** High-protein meals precipitate hyperammonemic crises (as in this vignette). ### Why This Case is Citrullinemia Type I 1. **Marked hypercitrullinemia (1200 µmol/L):** Diagnostic; citrulline cannot be converted to argininosuccinate due to ASS deficiency. 2. **Undetectable argininosuccinate:** Confirms the block is at the ASS step. 3. **Hyperammonemia (450 µmol/L):** Urea cycle stalls; ammonia accumulates. 4. **Normal liver function:** Rules out hepatic encephalopathy; this is a primary urea cycle defect. 5. **Trigger:** High-protein meal precipitated the acute crisis — classic for citrullinemia type I. ### Management 1. **Acute:** Hemodialysis or hemofiltration to reduce ammonia and citrulline. 2. **Chronic:** - **Protein restriction:** 1.0–1.5 g/kg/day (age-dependent). - **Arginine supplementation:** 100–200 mg/kg/day (bypasses the block; arginine is essential in this defect). - **Sodium benzoate or sodium phenylbutyrate:** Alternative pathway for nitrogen disposal (conjugation with glycine or glutamine). 3. **Genetic counseling:** Autosomal recessive; both parents are carriers. **Clinical Pearl:** Unlike OTC deficiency (X-linked), citrullinemia type I is autosomal recessive, so both males and females are equally affected. Prenatal diagnosis and newborn screening (elevated citrulline on tandem mass spectrometry) are available. [cite:KD Tripathi 8e Ch 12] 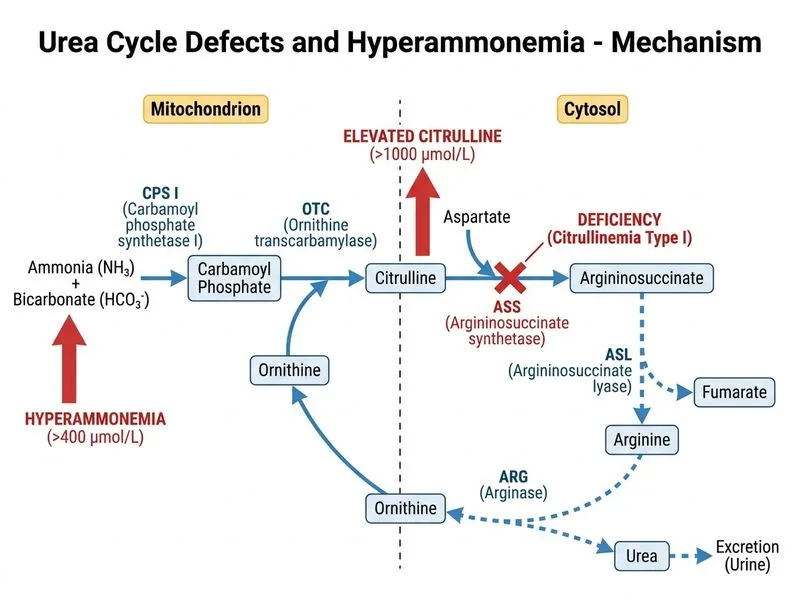
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.