## Management of Behçet Disease Uveitis ### Clinical Diagnosis: Behçet Disease **Key Point:** The triad of recurrent oral ulcers, genital ulcers, and acute severe uveitis with hypopyon and retinal vasculitis is diagnostic of Behçet disease. This is a systemic vasculitis requiring aggressive systemic immunosuppression. ### Why Topical Therapy Alone Is Insufficient **High-Yield:** Behçet uveitis is notoriously aggressive and vision-threatening. Topical corticosteroids alone fail to control the inflammation and prevent posterior segment complications (retinal vasculitis, optic atrophy, neovascularization). ### Management Algorithm for Behçet Uveitis ```mermaid flowchart TD A[Behçet disease uveitis diagnosed]:::outcome --> B{Severity assessment}:::decision B -->|Mild anterior uveitis| C[Topical corticosteroids + cycloplegics]:::action B -->|Severe or posterior involvement| D[Systemic corticosteroids]:::action D --> E[Immunosuppressive agents]:::action E --> F[Azathioprine or Mycophenolate mofetil]:::action F --> G[Monitor for remission and taper]:::action A --> H{Retinal vasculitis present?}:::decision H -->|Yes| I[Add anti-TNF agents if inadequate response]:::action H -->|No| J[Continue systemic therapy]:::action ``` ### Systemic Therapy Regimen | Agent | Dose | Indication | Rationale | |-------|------|-----------|----------| | **Prednisolone** | 1 mg/kg/day, taper | Initial control | Rapid anti-inflammatory effect | | **Azathioprine** | 1–2.5 mg/kg/day | Steroid-sparing | Reduces relapse rate by 50% | | **Mycophenolate mofetil** | 1–3 g/day divided | Alternative to AZA | Effective, better tolerated | | **Infliximab** | 5 mg/kg IV at weeks 0, 2, 6 | Refractory posterior uveitis | Anti-TNF; prevents vision loss | **Clinical Pearl:** Behçet uveitis has a relapsing-remitting course with 50% of untreated patients becoming blind within 5 years. Early aggressive systemic immunosuppression is the standard of care. ### Why Each Distractor Fails **Topical therapy alone:** - Does not penetrate the posterior segment adequately - Cannot suppress the systemic vasculitis - Leads to chronic inflammation, cataract, glaucoma, and optic atrophy **Antituberculous therapy:** - TB-uveitis presents with caseating lesions, not hypopyon - No TB history or serology in this case - Delays appropriate immunosuppression **Antiviral therapy:** - HSV/VZV uveitis does not present with hypopyon or retinal vasculitis - Oral ulcers in Behçet are aphthous, not herpetic ### Monitoring During Treatment **Key Point:** Monitor for: - Remission of anterior chamber cells (goal: 0–0.5+ cells) - Resolution of vitritis - Stabilization of retinal vasculitis - Steroid-sparing effect (taper prednisolone to ≤7.5 mg/day) - Immunosuppressive agent toxicity (CBC, LFTs every 3 months) **Mnemonic: BEAM** — **B**ehçet uveitis requires **E**arly **A**ggressive **M**anagement with systemic immunosuppression. [cite:Kanski Clinical Ophthalmology 9e Ch 8; American Academy of Ophthalmology Preferred Practice Pattern on Uveitis] 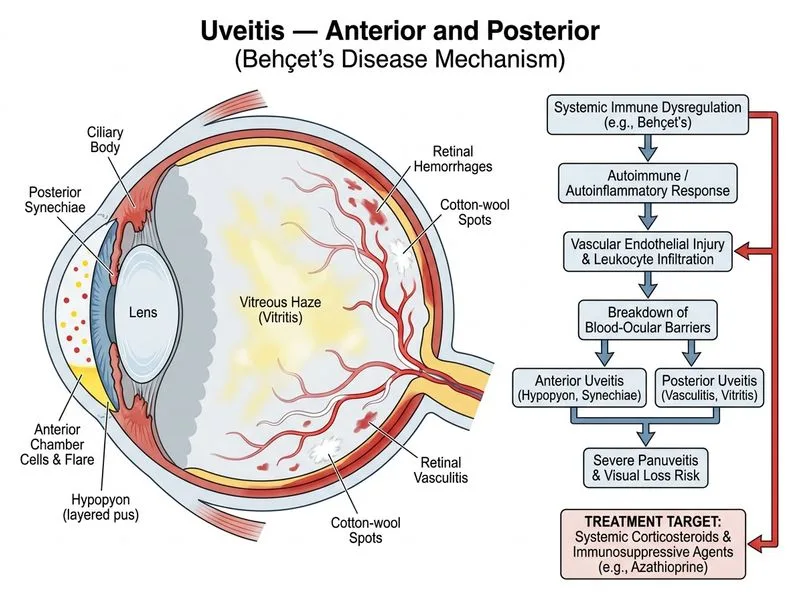
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.