## Acute Anterior Uveitis in Ankylosing Spondylitis ### Clinical Context **High-Yield:** Ankylosing spondylitis (AS) is the most common systemic cause of acute anterior uveitis (AAU) in young males, with HLA-B27 positivity in >90% of cases. Acute AAU in AS typically presents with **sudden onset pain, photophobia, and marked anterior chamber inflammation**. **Key Point:** The clinical presentation — acute pain, photophobia, 4+ anterior chamber reaction with hypopyon, posterior synechiae, and normal IOP — is classic for acute anterior uveitis. The normal fundus and absence of systemic symptoms at presentation argue against infectious or posterior segment involvement. ### Management Algorithm ```mermaid flowchart TD A[Acute Anterior Uveitis]:::outcome --> B{Infectious cause?}:::decision B -->|Yes: hypopyon, pain, fever| C[Culture, tap, antibiotic]:::action B -->|No: idiopathic/systemic| D[Topical corticosteroids]:::action D --> E[Cycloplegic agent]:::action E --> F[Systemic NSAIDs/steroids]:::action F --> G[Monitor IOP, synechiae]:::action G --> H{Controlled?}:::decision H -->|Yes| I[Taper steroids over weeks]:::action H -->|No| J[Escalate: systemic steroids ± immunosuppression]:::action ``` ### Step-by-Step Initial Management 1. **Topical corticosteroids** (prednisolone acetate 1% every 1–2 hours initially) - Reduces anterior chamber inflammation rapidly - Prevents posterior synechiae formation (already present here, but prevents progression) 2. **Cycloplegic agents** (cyclopentolate 1% or tropicamide 1% three times daily) - Relieves ciliary muscle spasm and pain - Reduces posterior synechiae formation 3. **Systemic NSAIDs** (indomethacin 50–75 mg/day or ibuprofen 1200 mg/day) - First-line systemic agent for AAU in AS - Addresses both uveitis and underlying spondylitis - Particularly effective in HLA-B27–associated uveitis 4. **Close monitoring** - Slit-lamp examination every 2–3 days initially - IOP measurement (risk of secondary glaucoma if inflammation not controlled) - Assess for posterior synechiae progression **Clinical Pearl:** Systemic corticosteroids are NOT first-line in uncomplicated acute anterior uveitis; NSAIDs are preferred because they address both the uveitis and the underlying spondylitis. Systemic steroids are reserved for: - Severe inflammation unresponsive to NSAIDs - Bilateral disease - Immunocompromised patients - Infectious causes ruled out ### Why NOT Immediate Anterior Chamber Tap? **Warning:** Anterior chamber tap is indicated only when **infectious uveitis is suspected** (bacterial, fungal, or viral keratouveitis). This patient has: - No fever or systemic infection signs - Clear history of AS (known systemic cause) - No corneal infiltrate or ulceration - Normal IOP (argues against endophthalmitis) Tapping would be unnecessary and traumatic. ### Why NOT Systemic Corticosteroids Alone? While systemic steroids are used in severe AAU, **NSAIDs are superior in HLA-B27–associated disease** because they: - Reduce uveitis recurrence rates - Treat the underlying spondylitis - Avoid long-term steroid side effects [cite:Kanski & Bowling 8e Ch 12; American Academy of Ophthalmology Uveitis Preferred Practice Pattern] 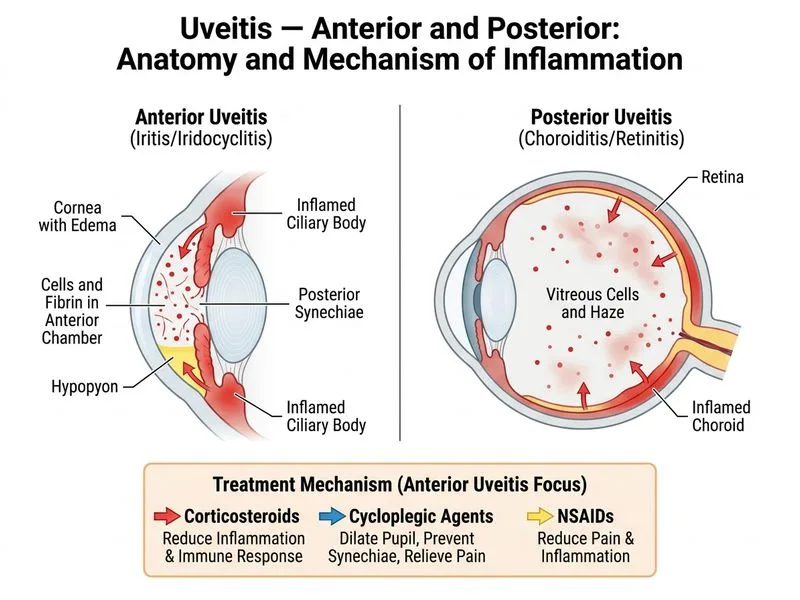
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.