## Diagnosis: Sarcoidosis ### Clinical Presentation Analysis **Key Point:** The combination of granulomatous anterior uveitis with irregular fixed pupil (posterior synechiae), vitritis, retinal infiltrates, AND systemic findings (bilateral hilar lymphadenopathy, elevated ACE) is pathognomonic for sarcoidosis. ### Diagnostic Features of Sarcoidosis | Feature | Finding in This Case | Significance | |---------|----------------------|---------------| | **Keratic Precipitates** | Fine, granulomatous pattern | Indicates granulomatous inflammation | | **Anterior Chamber** | 3+ cells | Moderate-to-severe granulomatous uveitis | | **Pupil** | Irregular, fixed | Posterior synechiae from chronic inflammation | | **Vitreous** | 2+ haze with infiltrates | Posterior segment involvement (pars planitis pattern) | | **Systemic Findings** | Hilar lymphadenopathy, elevated ACE | Confirms systemic sarcoidosis | ### Pathophysiology **High-Yield:** Sarcoidosis is a multisystem granulomatous disorder of unknown etiology. Ocular involvement occurs in ~25% of systemic sarcoidosis cases and presents as: 1. **Anterior uveitis** (most common) — granulomatous type 2. **Posterior uveitis** — retinal infiltrates, optic nerve involvement, pars planitis 3. **Lacrimal gland enlargement** — dry eye syndrome ### Why Sarcoidosis Over Other Granulomatous Uveitis? **Clinical Pearl:** The presence of **elevated serum ACE level** combined with **bilateral hilar lymphadenopathy** on chest X-ray makes sarcoidosis the single most likely diagnosis. TB and syphilis do not typically elevate ACE. ### Differential Diagnosis of Granulomatous Uveitis | Diagnosis | Keratic Precipitates | Systemic Findings | ACE Level | Diagnosis Confirmation | |-----------|----------------------|-------------------|-----------|------------------------| | **Sarcoidosis** | Fine, granulomatous | Hilar LAD, elevated ACE | ↑ | ACE, serum Ca²⁺, chest imaging | | **TB** | Granulomatous | Pulmonary infiltrates, constitutional symptoms | Normal | Mantoux, GeneXpert, IGRA | | **Syphilis** | Granulomatous or non-granulomatous | Rash, mucous patches, condyloma | Normal | RPR/VDRL, FTA-ABS, dark-field | | **Toxoplasmosis** | Non-granulomatous | None (congenital or reactivation) | Normal | Serology, PCR, focal retinal necrosis | **Mnemonic for Granulomatous Uveitis:** **SATIN** = **S**arcoidosis, **A**utoimmune (Vogt-Koyanagi-Harada), **T**uberculosis, **I**nfectious (syphilis, leprosy, TB), **N**eoplasm (lymphoma, carcinoma) ### Management Approach 1. **Confirm diagnosis:** Serum ACE, serum calcium, chest HRCT, ophthalmology referral 2. **Systemic workup:** Rule out pulmonary, cardiac, renal involvement 3. **Treatment:** Topical corticosteroids (prednisolone acetate 1% QID) + systemic corticosteroids (prednisolone 0.5–1 mg/kg/day) for posterior segment involvement 4. **Immunosuppression:** Methotrexate or mycophenolate mofetil for steroid-dependent or refractory cases [cite:Kanski Clinical Ophthalmology 9e Ch 9] 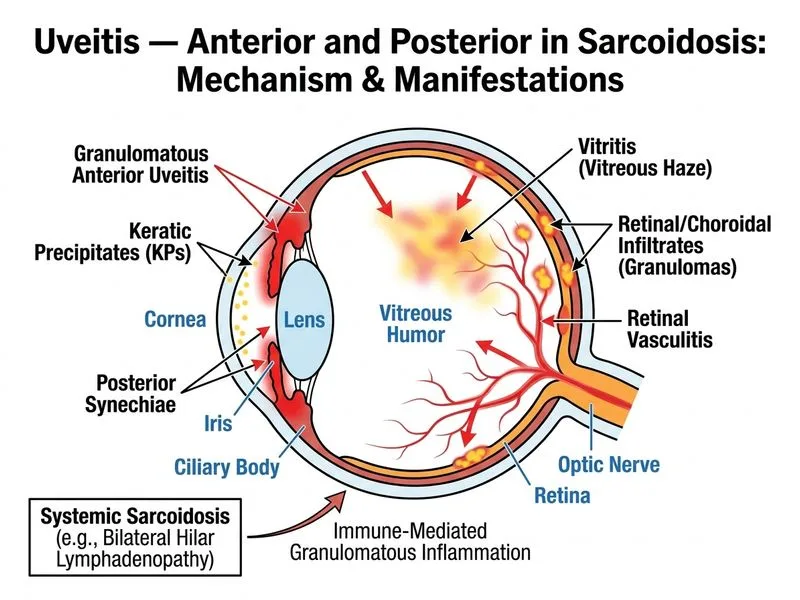
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.