## Clinical Diagnosis **Key Point:** This patient has **severe chronic aortic regurgitation (AR)** with **symptomatic left ventricular dysfunction** (EF 35%, LVEDD 58 mm, exertional dyspnea and chest discomfort). ### Diagnostic Features of Chronic AR - **Early diastolic murmur** (high-pitched, blowing) → incompetent aortic valve during diastole - **Best heard at left sternal border, leaning forward** → aortic area, with patient optimizing aortic regurgitant flow - **Increases with Valsalva** → increased LV volume increases regurgitant flow - **Brisk pulses, wide pulse pressure** → hyperdynamic circulation (large stroke volume) - **Dilated LV with reduced EF** → chronic volume overload causing eccentric LV remodeling and systolic dysfunction - **Regurgitant volume 60 mL/beat** → severe AR (>50 mL/beat is severe) ### Echocardiographic Severity of AR | Parameter | Mild | Moderate | Severe | |-----------|------|----------|--------| | Jet width (% LVOT) | <25 | 25–65 | >65 | | Regurgitant volume (mL) | <30 | 30–59 | ≥60 | | Regurgitant fraction (%) | <30 | 30–49 | ≥50 | | LV dilatation | Normal | Mild–moderate | Severe (LVEDD >55 mm) | **High-Yield:** This patient meets **Class I indication for aortic valve replacement** [cite:Harrison 21e Ch 297]. ## Indications for AVR in Chronic AR ### Symptomatic Patients (Class I) - **Symptoms of heart failure** (dyspnea, chest discomfort) + severe AR ✓ (this patient) - **Angina** from increased myocardial oxygen demand ### Asymptomatic Patients (Class IIa–IIb) - EF <50% (this patient: EF 35%, **Class I**) - LVEDD >55 mm (this patient: 58 mm, **Class I**) - LVESD >40 mm **Clinical Pearl:** Waiting for "further deterioration" in a patient with **symptomatic severe AR and EF 35%** risks irreversible myocardial damage, atrial fibrillation, and sudden cardiac death. The window for optimal surgical outcomes is **now** [cite:Harrison 21e Ch 297]. ## Management Strategy ### Preoperative Medical Optimization (Bridge to Surgery) 1. **ACE inhibitor** (e.g., lisinopril 10 mg daily) - Reduces afterload → decreases regurgitant volume - Slows LV remodeling - Improves symptoms 2. **Beta-blocker** (e.g., metoprolol 50 mg BD) - Slows heart rate → prolongs diastole, worsening AR - BUT reduces myocardial contractility demand - Net benefit in symptomatic patients 3. **Avoid diuretics** unless pulmonary edema present (reduce preload, worsening regurgitation) 4. **Avoid vasodilators like hydralazine** as monotherapy (less effective than ACE inhibitors; no mortality benefit) **Mnemonic: Chronic AR Medical Therapy — ACE-B** - **A** = ACE inhibitor (first-line) - **C** = Control heart rate (beta-blocker) - **E** = Evaluate for surgery (do NOT delay) - **B** = Bridge to definitive intervention ### Definitive Management: Aortic Valve Replacement **Indications MET:** - ✓ Symptomatic (dyspnea, chest discomfort) - ✓ Severe AR (regurgitant volume 60 mL) - ✓ LV dysfunction (EF 35%, LVEDD 58 mm) **Timing:** **URGENT** (within weeks, not months) - Delay risks irreversible LV dysfunction, arrhythmias, and sudden death - Prognosis after AVR is excellent if EF >30% and LVEDD <65 mm **Valve choice:** - Age 72 → **Mechanical valve** (durability) if patient willing to take lifelong warfarin - OR **Bioprosthetic valve** (lower bleeding risk, but limited durability; may need redo surgery) **Percutaneous aortic valve implantation (TAVI)** is NOT appropriate here: - Primarily for **aortic stenosis**, not regurgitation - Poor outcomes in pure AR (valve migration, paravalvular leak) - Reserved for inoperable/high-risk patients with AS 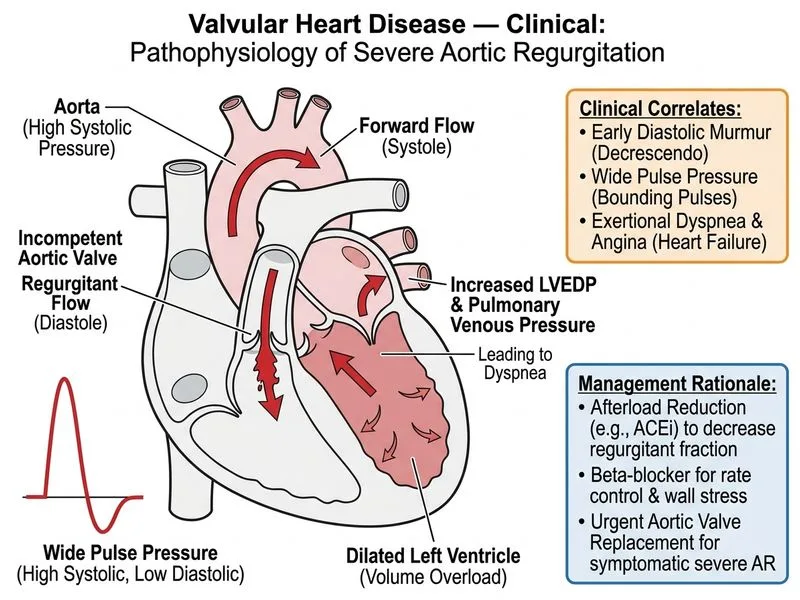
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.