## Clinical Scenario: Acute Decompensated MS with New-Onset AF This patient has **acute pulmonary edema secondary to mitral stenosis complicated by new-onset atrial fibrillation (AF) with rapid ventricular response**. The hemoptysis, orthopnea, and Kerley B lines indicate **acute left heart failure** from increased transmitral gradient due to loss of atrial kick and shortened diastolic filling time. **Key Point:** The immediate priority is **hemodynamic stabilization** through rate control, diuresis, and anticoagulation — NOT rhythm conversion or structural intervention. ## Acute Decompensated MS with AF: Management Algorithm ```mermaid flowchart TD A["Acute MS + AF<br/>Pulmonary edema"]:::outcome --> B["Assess hemodynamics"]:::action B --> C{"Hemodynamically<br/>unstable?"}:::decision C -->|"No"| D["Rate control<br/>Diuretics<br/>Anticoagulation"]:::action C -->|"Yes<br/>Cardiogenic shock<br/>Severe hypoxia"|E["Urgent intervention<br/>PMBV or MVR"]:::urgent D --> F["IV digoxin or<br/>beta-blocker"]:::action F --> G["IV furosemide"]:::action G --> H["UFH or LMWH"]:::action H --> I["Stabilization<br/>Plan definitive therapy"]:::outcome ``` ## Rationale for Immediate Medical Management | Step | Intervention | Rationale | |------|--------------|----------| | **Rate control** | IV digoxin (or IV beta-blocker if not contraindicated) | Slow AV nodal conduction; restore diastolic filling time; reduce transmitral gradient | | **Diuresis** | IV furosemide | Reduce pulmonary congestion; improve oxygenation | | **Anticoagulation** | Unfractionated heparin (UFH) | AF + MS = high thromboembolism risk; UFH allows rapid reversal if intervention needed | | **Oxygenation** | Supplemental O₂, consider CPAP | Improve PaO₂; reduce work of breathing | **High-Yield:** In **acute MS + AF with pulmonary edema**, the goal is **rate control, not rhythm control**. Attempting cardioversion or amiodarone without rate control and diuresis risks hemodynamic collapse because: - Restoring sinus rhythm suddenly increases atrial kick in a stenotic mitral valve → acute rise in LA pressure → pulmonary edema worsens - The stenotic valve cannot accommodate the increased flow **Clinical Pearl:** **Digoxin is preferred** in acute MS + AF because it: - Slows AV conduction (rate control) - Has positive inotropic effect (supports cardiac output) - Allows rapid reversal with digoxin-specific antibody if needed - Does not require IV access for continuous infusion (unlike amiodarone) ## Why Other Options Are Incorrect **Surgical MVR (Option 2):** Indicated only after medical stabilization fails or if the patient is in cardiogenic shock. This patient is hemodynamically compromised but not in shock; medical management is the first step. **PMBV (Option 3):** While PMBV may be considered once the patient is stabilized, it is **not** the immediate intervention. The acute decompensation is driven by AF with rapid ventricular response and loss of atrial kick — rate control and diuresis are urgent. PMBV can be planned electively after stabilization. **Amiodarone + cardioversion (Option 4):** Amiodarone is a rhythm-control agent, not rate control. Attempting cardioversion or rhythm control in acute MS + AF with pulmonary edema is **dangerous** because: - Sudden restoration of sinus rhythm increases LA pressure acutely - The stenotic mitral valve cannot accommodate the increased diastolic flow - Pulmonary edema worsens; cardiogenic shock may develop - Amiodarone is also negatively inotropic and can worsen hemodynamics **Mnemonic:** **DURA** for acute MS + AF management: - **D**iuretics (IV furosemide) - **U**nfractionated heparin (anticoagulation) - **R**ate control (digoxin or beta-blocker) - **A**fter stabilization → plan definitive therapy (PMBV or MVR) [cite:Harrison 21e Ch 297; KD Tripathi 8e Ch 12] 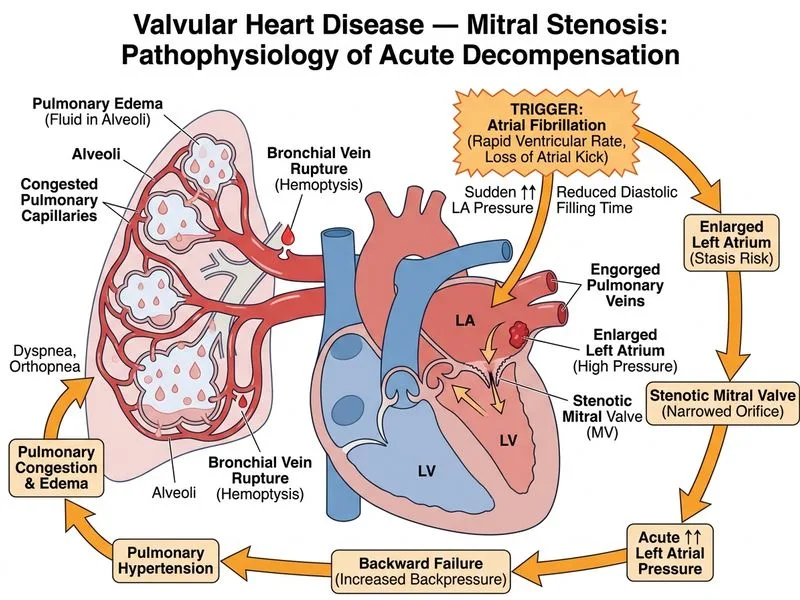
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.