## Clinical Diagnosis: Granulomatosis with Polyangiitis (GPA) ### Key Diagnostic Criteria for GPA **Key Point:** GPA is a systemic necrotizing vasculitis of small and medium vessels characterized by the classic triad of upper respiratory tract involvement, pulmonary hemorrhage, and glomerulonephritis—all supported by c-ANCA/PR3 positivity and necrotizing vasculitis on biopsy. ### Pathognomonic Features in This Case | Feature | GPA | MPA | Goodpasture | SLE | |---------|-----|-----|-------------|-----| | **ANCA status** | c-ANCA/PR3+ | p-ANCA/MPO+ | ANCA-negative | ANCA-negative | | **Anti-GBM antibodies** | Absent | Absent | Present | Absent | | **Pulmonary hemorrhage** | Yes (hemoptysis) | Yes | Yes | Rare | | **Glomerulonephritis** | Crescentic (RPGN) | Crescentic (RPGN) | Anti-GBM crescentic | Lupus nephritis (various) | | **Upper respiratory involvement** | Yes (sinusitis, nasal crusting) | No | No | No | | **Granulomas on biopsy** | Yes (necrotizing) | No | No | No | | **Small-vessel vasculitis** | Yes | Yes | No (linear IgG on IFM) | Immune complex | | **Medium-vessel involvement** | Yes | No | No | No | ### Why This Patient Has GPA, Not MPA **High-Yield:** The critical distinguishing feature is **c-ANCA/PR3 positivity with necrotizing vasculitis on renal biopsy**. While both GPA and MPA present with pulmonary hemorrhage and crescentic GN, GPA has: 1. **c-ANCA/PR3 serology** (this patient is c-ANCA+) — MPA is p-ANCA/MPO+ 2. **Necrotizing vasculitis of small AND medium vessels** — MPA affects small vessels only 3. **Granulomatous inflammation** — MPA lacks granulomas 4. **Upper respiratory tract involvement** — Although not explicitly stated in the vignette, GPA commonly presents with sinusitis, nasal crusting, or otitis media; MPA does not **Clinical Pearl:** The presence of c-ANCA/PR3 serology is the single most reliable discriminator between GPA (c-ANCA+) and MPA (p-ANCA+). Both cause pulmonary-renal syndrome, but serology and biopsy findings (granulomas in GPA) settle the diagnosis. ### Distinguishing GPA from Goodpasture Syndrome - **Goodpasture** presents with pulmonary hemorrhage and crescentic GN but is **ANCA-negative** and **anti-GBM antibody-positive** - **GPA** is **c-ANCA/PR3-positive** and **anti-GBM-negative** - Goodpasture causes linear IgG deposition on immunofluorescence microscopy; GPA shows pauci-immune pattern ### Distinguishing GPA from SLE - **SLE** causes lupus nephritis (various patterns: diffuse proliferative, membranous, etc.) but NOT crescentic GN with necrotizing vasculitis - **SLE** is ANCA-negative and ANA-positive (not tested here, but would be positive) - **SLE** causes immune-complex-mediated glomerulonephritis, not pauci-immune vasculitis ### Pathophysiology of GPA GPA is an ANCA-associated vasculitis (AAV) driven by anti-PR3 (proteinase-3) antibodies. These antibodies bind to PR3 on the surface of activated neutrophils, triggering: 1. Complement activation and neutrophil recruitment 2. Fibrinoid necrosis of small and medium vessels 3. Granulomatous inflammation (epithelioid histiocytes and giant cells) 4. Tissue destruction in the upper respiratory tract, lungs, and kidneys The renal biopsy findings—segmental fibrinoid necrosis with crescent formation and necrotizing vasculitis—are classic for ANCA-associated GN (pauci-immune pattern on immunofluorescence). **Mnemonic: "GPA = c-ANCA/PR3 + Granulomas + Glomerulonephritis (crescentic) + Gaps in upper respiratory tract"** [cite:Robbins 10e Ch 11; Harrison 21e Ch 298] 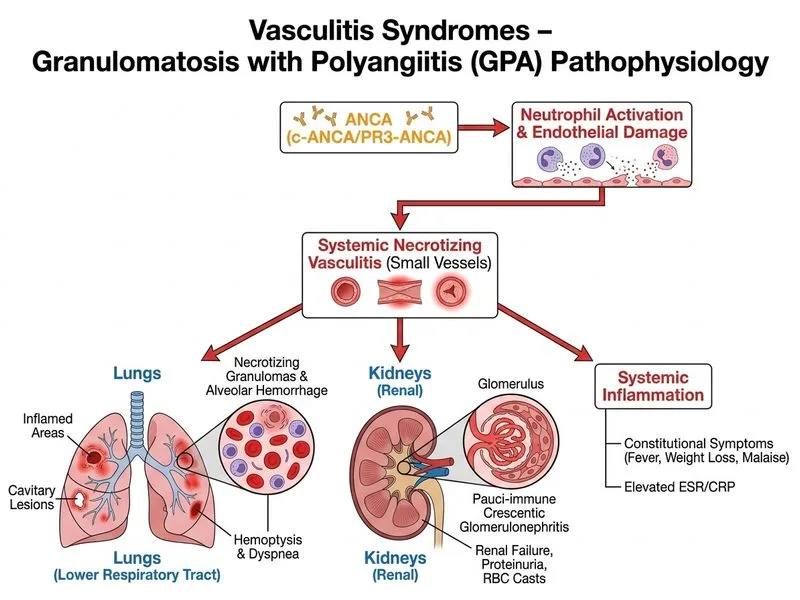
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.