## Clinical Diagnosis: Takayasu Arteritis ### Key Distinguishing Features **Key Point:** Takayasu arteritis is a large-vessel granulomatous vasculitis affecting the aorta and its major branches, with a strong predilection for young females from Asia, but can occur in males and older individuals. ### Clinical Presentation Matching This Case 1. **Large-vessel involvement**: Aorta and proximal branches (femoral, iliac, subclavian) 2. **Progressive claudication**: Due to smooth, concentric narrowing of major vessels 3. **Elevated inflammatory markers**: ESR and CRP reflect active vasculitis 4. **Angiographic findings**: Smooth, tapered ("pencil-like") narrowing with skip lesions is characteristic of Takayasu arteritis. Note: The classic "string of beads" pattern is more precisely associated with fibromuscular dysplasia; in Takayasu, the angiographic hallmark is smooth, concentric stenosis of the aorta and its branches. 5. **Hypertension**: From renal artery involvement or aortic coarctation-like narrowing ### Pathological Features | Feature | Takayasu | GCA | PAN | Behçet | |---------|----------|-----|-----|--------| | **Vessel size** | Large (aorta, proximal branches) | Large (temporal, carotid) | Medium | Medium/large | | **Aorta involvement** | Yes, characteristic | Rare | No | Possible | | **Age group** | Young females, young adults | >50 years | 40–60 years | 20–40 years | | **Geography** | Asia, Latin America | Caucasian | Any | Mediterranean, Asia | | **Angiography pattern** | Smooth, tapered narrowing; skip lesions | N/A (clinical diagnosis) | Beading, microaneurysms | Occlusions, aneurysms | **High-Yield:** Takayasu is the most common cause of aortic narrowing in young patients worldwide; it causes "pulseless disease" (absent pulses) as seen here. Giant cell arteritis (GCA) is excluded by the patient's age (<60 is borderline, but GCA typically involves temporal/cranial arteries and rarely causes lower-limb claudication). Polyarteritis nodosa affects medium vessels and does not involve the aorta. Behçet disease causes venous thrombosis and mucocutaneous lesions rather than this angiographic pattern. ### Diagnostic Criteria (ACR / Sharma Classification) 1. Age <40 years at onset 2. Claudication of extremities 3. Decreased brachial artery pulse 4. Blood pressure difference >10 mmHg between arms 5. Aortic/subclavian artery bruit 6. Aortic/subclavian artery narrowing on angiography **Clinical Pearl:** This patient meets criteria 2 (claudication), 3 (absent femoral and distal pulses), and 6 (smooth aortic narrowing on angiography), making Takayasu arteritis the most likely diagnosis. The angiographic appearance in Takayasu is smooth, concentric stenosis — distinct from the "string of beads" of fibromuscular dysplasia, which shows alternating stenoses and dilatations. ### Management Approach - **First-line**: High-dose corticosteroids (prednisolone 1 mg/kg/day) - **Steroid-sparing / refractory**: Methotrexate, azathioprine, mycophenolate mofetil - **Biologic agents**: TNF-α inhibitors (infliximab, etanercept) for refractory disease - **Revascularization**: Surgical bypass or angioplasty during remission phase **Key Point:** Monitor disease activity with ESR, CRP, and serial imaging (MR angiography preferred over conventional angiography for follow-up). [cite: Robbins & Cotran Pathologic Basis of Disease, 10e, Ch 11; Harrison's Principles of Internal Medicine, 21e] 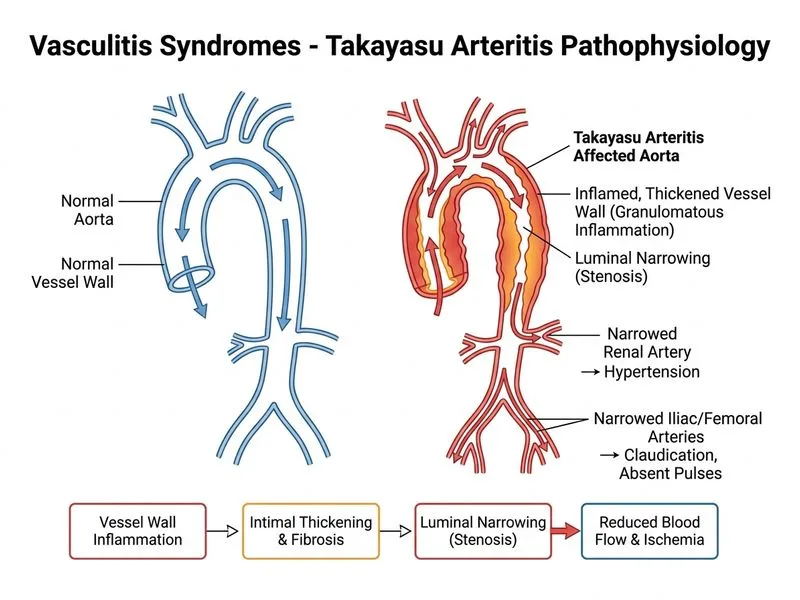
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.