## Clinical Diagnosis: Giant Cell Arteritis (Temporal Arteritis) with Arteritic AION ### Key Diagnostic Features **Key Point:** Giant cell arteritis (GCA) is a large-vessel vasculitis affecting the temporal, carotid, and vertebral arteries, presenting classically in patients >50 years with headache, scalp tenderness, jaw claudication, and vision loss. ### Classic Triad of GCA 1. **Headache** (often severe, localized to temporal region) 2. **Jaw claudication** (pain while chewing, pathognomonic) 3. **Vision loss** (from arteritic anterior ischemic optic neuropathy—AAION) **High-Yield:** Arteritic AION is a medical emergency; vision loss occurs in 15–20% of untreated GCA and is often irreversible if not treated urgently. ### Pathological Findings | Feature | GCA | Takayasu | PAN | GPA | |---------|-----|----------|-----|-----| | **Age at onset** | >50 years | Young adults | 40–60 years | 40–60 years | | **Temporal artery involvement** | Yes, characteristic | No | No | No | | **Biopsy findings** | Granulomatous, giant cells, IEL fragmentation | Granulomatous, giant cells, IEL fragmentation | Fibrinoid necrosis, no granulomas | ANCA+, necrotizing, no granulomas | | **Jaw claudication** | Yes, classic | No | No | No | | **Vision loss pattern** | AAION (sudden, painless) | Rare | Rare | Orbital inflammation | | **ESR/CRP** | Markedly elevated | Elevated | Elevated | Variable | **Clinical Pearl:** Jaw claudication is nearly pathognomonic for GCA and should always prompt urgent evaluation and biopsy. ### Mechanism of Vision Loss in GCA ```mermaid flowchart TD A[GCA: Inflammation of temporal artery]:::outcome --> B[Narrowing of posterior ciliary arteries]:::action B --> C[Ischemia of optic nerve head]:::action C --> D[Arteritic anterior ischemic optic neuropathy AAION]:::outcome D --> E{Treated <2 weeks?}:::decision E -->|Yes| F[Vision loss may stabilize]:::action E -->|No| G[Permanent vision loss likely]:::urgent ``` **Warning:** Vision loss in GCA is a medical emergency. High-dose corticosteroids must be started immediately, even before biopsy confirmation if clinical suspicion is high. ### Diagnostic Workup 1. **ESR and CRP**: Both markedly elevated (ESR often >90 mm/h) 2. **Temporal artery biopsy**: Gold standard - Granulomatous inflammation - Giant cells (multinucleated) - Fragmentation of internal elastic lamina (IEL) - Intimal proliferation 3. **Imaging**: Temporal artery ultrasound (halo sign), PET-CT for large-vessel involvement **High-Yield:** Biopsy findings of granulomatous inflammation with giant cells and IEL fragmentation are diagnostic; this patient's biopsy is classic for GCA. ### Management Algorithm ```mermaid flowchart TD A[Suspected GCA with vision loss]:::urgent --> B[Start high-dose corticosteroids immediately]:::action B --> C[Perform temporal artery biopsy within 1 week]:::action C --> D{Biopsy positive?}:::decision D -->|Yes| E[Confirm GCA diagnosis]:::outcome D -->|No| F[Reconsider diagnosis, imaging]:::action E --> G[Taper corticosteroids slowly over months]:::action G --> H[Monitor ESR/CRP, symptoms]:::action H --> I{Relapse?}:::decision I -->|Yes| J[Add methotrexate or biologic agents]:::action I -->|No| K[Continue maintenance therapy]:::action ``` **Key Point:** Initial corticosteroid dose is 40–60 mg/day prednisone; vision loss requires urgent treatment to prevent further ischemia. [cite:Harrison 21e Ch 297] 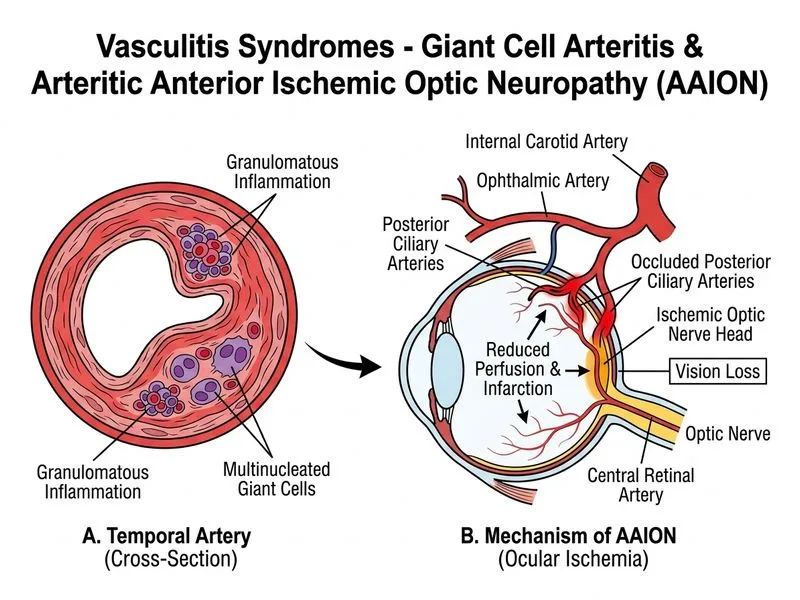
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.