## Clinical Diagnosis: Herpes Zoster Keratitis (Herpes Zoster Ophthalmicus) ### Key Clinical Features **Key Point:** The combination of dermatomal vesicular rash (forehead and upper eyelid — V1 distribution) with dendritic corneal ulcers, anterior chamber reaction, and reduced corneal sensation is pathognomonic for **Herpes Zoster Ophthalmicus (HZO)**, caused by reactivation of Varicella-Zoster Virus (VZV). ### Why Option C (Herpes Zoster Keratitis) is Correct "Herpes zoster keratitis" is the precise, standard clinical term for corneal involvement in HZO. Option B ("VZV keratitis with dermatomal distribution") is redundant and non-standard — VZV keratitis is by definition dermatomal. Option C is the textbook diagnosis (Kanski's Clinical Ophthalmology; Yanoff & Duker). ### Distinguishing Features: HSV vs VZV (Herpes Zoster) Keratitis | Feature | HSV Keratitis | Herpes Zoster Keratitis | |---------|---------------|------------------------| | **Skin involvement** | Rare; non-dermatomal if present | Dermatomal vesicular rash (V1 distribution) | | **Corneal ulcer morphology** | Classic dendritic with terminal bulbs | Dendritic (coarser, less well-defined bulbs) or geographic | | **Anterior chamber reaction** | Mild to moderate | Often more pronounced | | **Corneal sensation** | Reduced early | Reduced (may persist longer) | | **Recurrence** | Common (50% within 5 years) | Rare after initial episode | | **Age of presentation** | Any age | Typically >50 years (immunocompromised at any age) | | **Prodrome** | Mild or absent | Dermatomal pain precedes rash by 3–5 days | **High-Yield:** The dermatomal vesicular rash in the ophthalmic division (V1) of the trigeminal nerve is the single most important discriminator. HSV keratitis does NOT present with a dermatomal rash. ### Pathophysiology 1. Reactivation of latent VZV in the trigeminal (Gasserian) ganglion 2. Viral dissemination along V1 (ophthalmic) nerve branches — frontal, lacrimal, nasociliary 3. Epithelial necrosis → dendritic/geographic ulceration 4. Stromal inflammation and anterior uveitis 5. Chronic sequelae: stromal scarring, neovascularization, post-herpetic neuralgia ### Management Principles **Key Point:** Systemic antiviral therapy is MANDATORY in herpes zoster keratitis. - **First-line:** Acyclovir 800 mg 5 times daily × 7–10 days (or Valacyclovir 1 g TID) - **Topical:** Preservative-free lubricants; topical antivirals have limited role in VZV - **Avoid:** Topical corticosteroids in active epithelial disease - **Adjunctive:** Cycloplegics for anterior uveitis; analgesics for post-herpetic neuralgia **Clinical Pearl:** Hutchinson's sign (vesicles on the tip/side of the nose — nasociliary branch involvement) predicts a higher risk of ocular complications in HZO. Early systemic antivirals reduce post-herpetic neuralgia incidence (Harrison's Principles of Internal Medicine, 21st ed.). ### Why Not the Other Options? - **A (Adenoviral keratitis):** Presents as epidemic keratoconjunctivitis with subepithelial infiltrates, NO dendritic ulcers, NO dermatomal rash. - **B (VZV keratitis with dermatomal distribution):** Redundant, non-standard phrasing; "Herpes zoster keratitis" (Option C) is the correct clinical term. - **D (HSV keratitis):** Classic dendritic ulcers with terminal bulbs occur, but NO dermatomal vesicular rash; corneal sensation reduced but rash distribution is non-dermatomal. 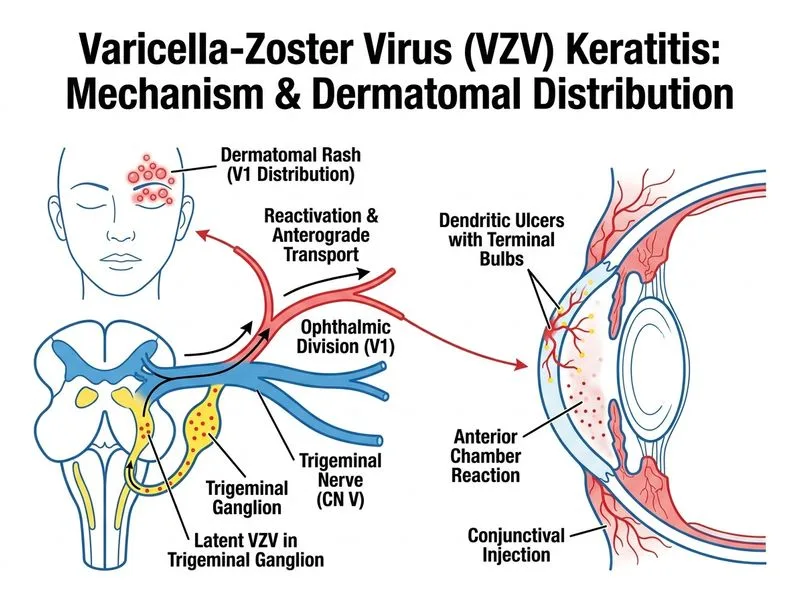
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.