## Clinical Diagnosis: Herpes Zoster Keratitis (Herpes Zoster Ophthalmicus) ### Key Clinical Features **Key Point:** This patient presents with the classic triad of herpes zoster ophthalmicus (HZO): (1) dermatomal vesicular rash in the V1 (ophthalmic) distribution — forehead and upper eyelid — preceding ocular symptoms, (2) dendritic corneal ulcers on slit-lamp examination, and (3) fluorescein uptake at ulcer margins. The causative agent is Varicella-Zoster Virus (VZV) reactivating from the trigeminal ganglion. ### Why Option D (Herpes Zoster Keratitis) is Correct The dermatomal distribution of the vesicular rash (forehead + right upper eyelid = V1/ophthalmic division of trigeminal nerve) is the **key discriminator** pointing to VZV reactivation, not HSV. HZO is the clinical syndrome when zoster involves the ophthalmic division of CN V. VZV keratitis can produce dendritic ulcers, though they tend to be more coarse/geographic compared to HSV; however, the dermatomal rash is pathognomonic for zoster etiology. ### Distinguishing Features: VZV vs HSV Keratitis | Feature | Herpes Zoster Keratitis (VZV) | Herpes Simplex Keratitis (HSV) | |---------|-------------------------------|-------------------------------| | **Skin rash** | Dermatomal vesicular rash (V1 in HZO) | Periocular vesicles, NOT dermatomal | | **Dendritic ulcers** | Present; coarser, less well-defined terminal bulbs | Classic fine branching dendrites with well-defined terminal bulbs | | **Age** | Typically >50 years (immunosenescence) | Any age | | **Corneal sensation** | Markedly reduced (hypoesthesia) | Reduced in recurrent disease | | **Hutchinson's sign** | Nasociliary involvement → high ocular risk | Not applicable | | **Recurrence** | Less frequent than HSV | High (up to 50% within 5 years) | ### Why Other Options Are Incorrect - **A) Adenoviral keratitis:** Causes epidemic keratoconjunctivitis with subepithelial infiltrates, NOT dendritic ulcers. No vesicular skin rash. - **B) Herpes simplex keratitis:** Classic for fine branching dendrites with terminal bulbs, but WITHOUT a dermatomal vesicular rash. The dermatomal skin involvement here rules out HSV as the primary diagnosis. - **C) Varicella-zoster keratitis with dermatomal distribution:** This option is essentially synonymous with Option D (Herpes Zoster Keratitis) but is a less precise/standard clinical term. "Herpes Zoster Keratitis" (Option D) is the accepted, standard clinical nomenclature for this condition. ### Clinical Pearl **Clinical Pearl:** Hutchinson's sign — vesicles on the tip or side of the nose (nasociliary nerve involvement) — predicts a higher risk of ocular involvement in HZO and mandates urgent ophthalmologic evaluation. (Kanski's Clinical Ophthalmology, 9th ed.) ### Management - **Systemic antivirals:** Acyclovir 800 mg 5× daily OR valacyclovir 1 g TID for 7–10 days (initiated within 72 hours of rash onset) - **Topical antivirals:** Adjunctive acyclovir ointment - **Cycloplegia:** If anterior uveitis present - **Topical steroids:** Only under specialist supervision for stromal/immune keratitis; contraindicated in active epithelial disease **High-Yield:** In any patient with a dermatomal vesicular rash in the V1 distribution + corneal dendrites, the diagnosis is Herpes Zoster Keratitis (HZO) — a medical emergency requiring urgent systemic antiviral therapy to prevent corneal scarring and vision loss. (Kanski's Clinical Ophthalmology; AAO Basic and Clinical Science Course, Section 8) 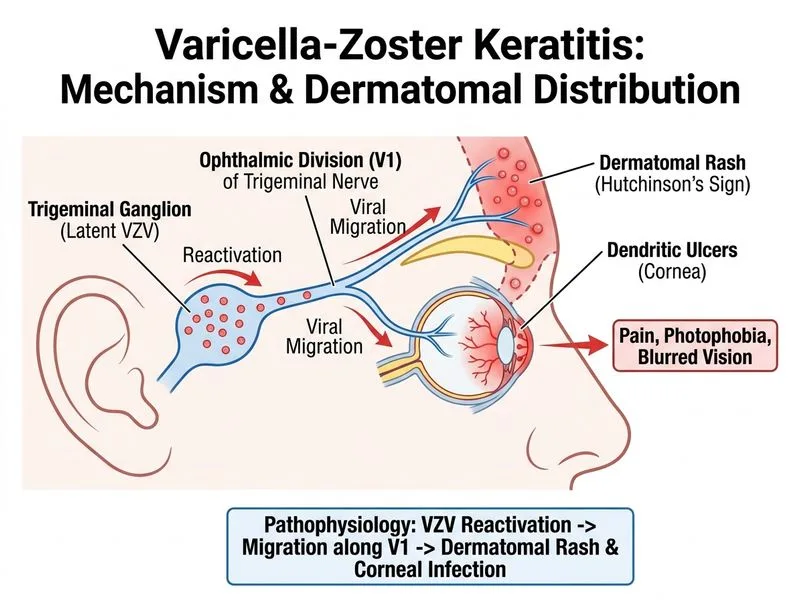
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.