## Management of Herpes Simplex Keratitis **Key Point:** Dendritic keratitis caused by HSV requires dual antiviral therapy — both topical and systemic — to prevent recurrence, stromal involvement, and vision-threatening complications. ### Clinical Recognition of HSV Dendritic Ulcer **High-Yield:** The pathognomonic findings are: - Fine, branching dendritic pattern with **terminal bulbs** (pathognomonic) - Edges stain with fluorescein (ulcer edges) - Center may stain with rose bengal or lissamine green (infected epithelial cells) - Mildly reduced corneal sensation (distinguishes from VZV, which has severe hypesthesia) - History of recurrent oral herpes (cold sores) strongly supports HSV ### Why This Patient Has HSV, Not VZV | Finding | HSV | VZV | |---------|-----|-----| | **History** | Recurrent cold sores (oral HSV) | Dermatomal vesicular rash | | **Dendritic pattern** | Fine, delicate with terminal bulbs | Coarser, broader | | **Corneal sensation** | Mildly reduced | Severely reduced/absent | | **Age** | Any age (recurrent) | Typically >50 years | | **Recurrence rate** | 25–50% | 5–10% | **Clinical Pearl:** The presence of a history of recurrent oral herpes (cold sores) is a major clue that subsequent keratitis is due to HSV, not VZV. This patient's mild corneal hypesthesia and fine dendritic ulcer with terminal bulbs confirm HSV. ### Pathophysiology of HSV Epithelial Keratitis 1. Reactivation of latent HSV-1 in the trigeminal ganglion 2. Anterograde axonal transport to cornea 3. Viral replication in corneal epithelial cells 4. Dendritic ulceration as infected cells slough 5. Immune response (antibodies, T cells) clears virus 6. Epithelial healing over 1–2 weeks with antiviral therapy ### Recommended Treatment Protocol ```mermaid flowchart TD A[HSV Epithelial Keratitis Confirmed]:::outcome --> B[Start Dual Antiviral Therapy]:::action B --> C[Topical acyclovir 5% ointment<br/>5 times daily × 7-10 days]:::action B --> D[Oral acyclovir 400 mg<br/>5 times daily × 7-10 days]:::action C --> E[Avoid topical corticosteroids<br/>in epithelial phase]:::urgent D --> E E --> F{Ulcer Healing?}:::decision F -->|Yes, epithelial healing| G[Continue antivirals<br/>Monitor for stromal involvement]:::action F -->|No improvement by day 7| H[Consider stromal keratitis<br/>Add topical corticosteroids<br/>+ systemic antivirals]:::action G --> I[Healing within 7-14 days]:::outcome ``` **Warning:** Do NOT use topical corticosteroids alone or as monotherapy in HSV epithelial keratitis — risk of **geographic ulceration** (coalescence of dendritic ulcers into large, irregular ulcer) and corneal perforation. Corticosteroids are only added if stromal keratitis develops (immune-mediated inflammation). **Mnemonic:** **ACYCLOVIR-HSV** = Antiviral (topical + systemic), Cold sores history, Youthful/any age, Cold sore recurrence, Lesion fine dendritic, Oral acyclovir essential, Vision-threatening if untreated, Initial phase: no steroids, Recurrent (25–50%), Stromal involvement later. ### Why Topical Corticosteroids Are Contraindicated Initially - Suppress local immune response - Allow unchecked viral replication - Risk of geographic ulceration (coalescence of dendritic ulcers) - Risk of stromal invasion and perforation - Corticosteroids are ONLY added if stromal keratitis develops (immune-mediated, not viral replication) ### Prognosis and Follow-up - Epithelial ulcers heal within 7–14 days with antiviral therapy - Recurrence rate: 25–50% within 5 years (risk increases with immunosuppression, UV exposure, stress) - Long-term suppressive therapy (oral acyclovir 400 mg daily) may be considered for frequent recurrences - Monitor for neurotrophic keratopathy and stromal scarring 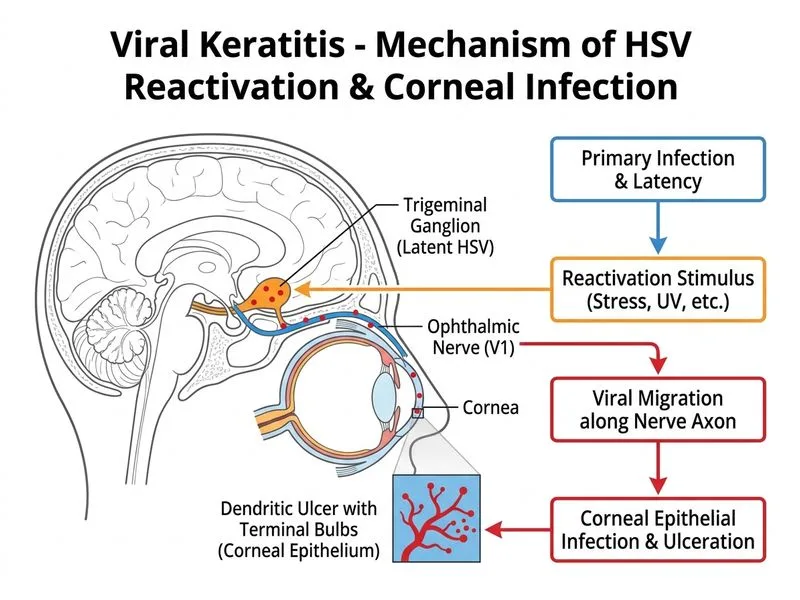
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.