## Clinical Presentation and Diagnosis **Key Point:** Bitemporal hemianopsia (loss of the temporal half of visual field in both eyes) is the classic sign of compression of the optic chiasm from below. ### Anatomical Basis The optic chiasm contains crossing nasal retinal fibers (which represent the temporal visual fields). When compressed from below, the inferior nasal fibers are affected first, producing superior temporal quadrantanopsia, which progresses to complete bitemporal hemianopsia as compression worsens. ### Differential Diagnosis of Sellar/Suprasellar Masses | Feature | Pituitary Adenoma | Craniopharyngioma | Meningioma | Optic Nerve Glioma | |---------|-------------------|-------------------|-----------|--------------------| | **Age of onset** | 40–60 years | Bimodal: 5–14 and 50–74 years | 40–70 years | Childhood (< 20 years) | | **Location** | Intrasellar, compresses from below | Suprasellar, above chiasm | Tuberculum sellae (suprasellar) | Along optic nerve | | **VF defect** | Bitemporal hemianopsia (inferior first) | Bitemporal hemianopsia (superior first) | Bitemporal or monocular | Monocular or arcuate | | **Endocrine signs** | Common (prolactin, ACTH, GH excess) | Rare | Absent | Absent | | **Imaging** | Sellar, homogeneous enhancement | Suprasellar, cystic, calcification common | Dural attachment, hyperostotic | Along nerve, T2 hyperintense | **High-Yield:** In this patient, the mass is described as compressing the chiasm **from below**, which is pathognomonic for a **pituitary adenoma**. Craniopharyngiomas typically arise above the chiasm and compress it from above, producing superior temporal quadrantanopsia initially. ### Clinical Pearl Bitemporal hemianopsia with inferior temporal quadrantanopsia progressing to complete bitemporal loss suggests pituitary adenoma until proven otherwise. The patient should be screened for hormonal excess (prolactin, ACTH, GH, TSH). ### Why Pituitary Adenoma Fits 1. Compresses chiasm **from below** (sellar origin) 2. Produces classic bitemporal hemianopsia 3. Age 58 fits typical presentation (40–60 years) 4. Gradual onset over 6 months is typical [cite:Neuro-ophthalmology, Kline & Bajandas] 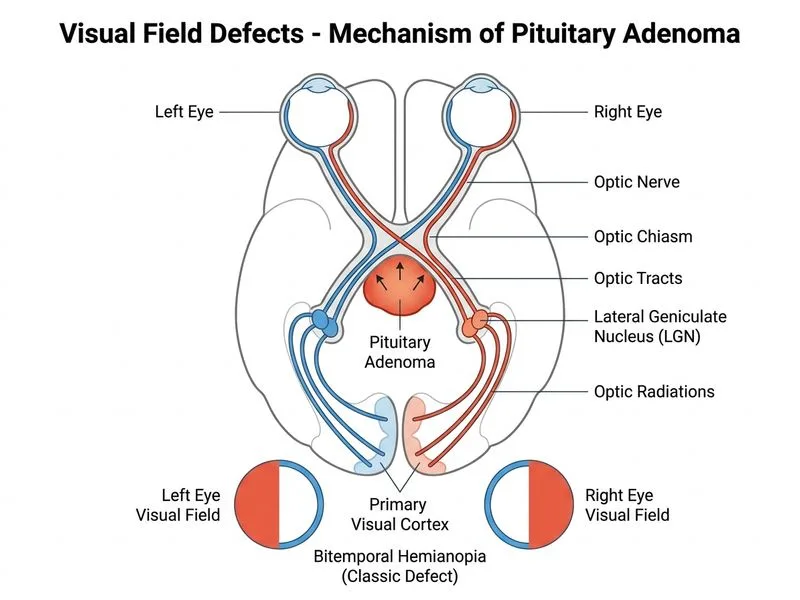
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.