## Clinical Assessment This child presents with **corneal xerosis with ulceration (WHO stage X3A)** — a **sight-threatening complication** of vitamin A deficiency. Key features: - **Corneal haziness** (loss of transparency) - **Central corneal ulcer** (3 × 2 mm) - **Soft cornea** (risk of perforation and permanent scarring) - **Conjunctival xerosis + Bitot's spots** (systemic VAD) - **Risk factors:** severe malnutrition + recent measles (measles depletes vitamin A stores) ## Pathophysiology of Corneal Xerosis **Key Point:** Vitamin A deficiency causes loss of **mucin-secreting goblet cells** and **squamous metaplasia** of corneal epithelium, leading to: 1. Loss of corneal transparency (haze) 2. Epithelial breakdown and ulceration 3. Stromal softening (keratomalacia) 4. Risk of perforation and permanent scarring/blindness **High-Yield:** Corneal involvement (X2 or worse) is a **medical emergency** because it can lead to **irreversible blindness** within days to weeks if not treated aggressively. ## WHO Dosing for VAD with Corneal Involvement | Stage | Route | Dose | Schedule | |-------|-------|------|----------| | **XN, X1A, X1B** (pre-corneal) | Oral | 200,000 IU | Days 1, 2, 14 | | **X2, X3A, X3B** (corneal) | **IM/IV** | **100,000 IU** | **Stat, then 50,000 IU daily × 14 days** | | **Severe malabsorption** | IM/IV | 100,000 IU | Stat, then 50,000 IU daily × 14 days | **Clinical Pearl:** Once the cornea is involved, **parenteral vitamin A is mandatory** because: 1. Systemic absorption is critical and cannot be delayed 2. Oral absorption may be impaired by malnutrition 3. Rapid restoration of epithelial integrity is needed to prevent perforation ## Additional Management for Corneal Xerosis **Key Point:** Supportive care is **equally critical** as vitamin A supplementation: - **Topical antibiotics** (chloramphenicol or gentamicin ointment) to prevent secondary bacterial infection - **Topical lubricants** (artificial tears, ointment) to protect the cornea - **Cycloplegia** (tropicamide or atropine) to reduce ciliary spasm and pain - **Eye padding/protective glasses** to prevent mechanical trauma - **Nutritional rehabilitation:** high-protein diet, micronutrient supplementation - **Treat underlying cause:** measles vaccination, nutritional counseling **Warning:** Do NOT defer vitamin A supplementation or use oral-only therapy in corneal disease — this risks permanent blindness. ## Why This Answer Is Correct Option 1 (IM vitamin A 100,000 IU stat, then 50,000 IU daily × 14 days) is the **WHO-recommended protocol for corneal xerophthalmia**. This approach: 1. **Rapidly replenishes systemic retinol** via parenteral route (bypassing malabsorption) 2. **Halts corneal softening** and prevents perforation 3. **Restores epithelial integrity** and reduces scarring risk 4. **Combined with topical antibiotics and lubricants** to prevent secondary infection and mechanical trauma [cite:Park 26e Ch 10; WHO Guidelines on Vitamin A Supplementation] ## Prognosis - **If treated early (X2 stage):** Full recovery with clear cornea - **If treated at X3A stage:** May leave corneal opacity or scar, but vision salvageable - **If untreated or delayed:** Corneal perforation → permanent blindness (corneal scar stage XS) 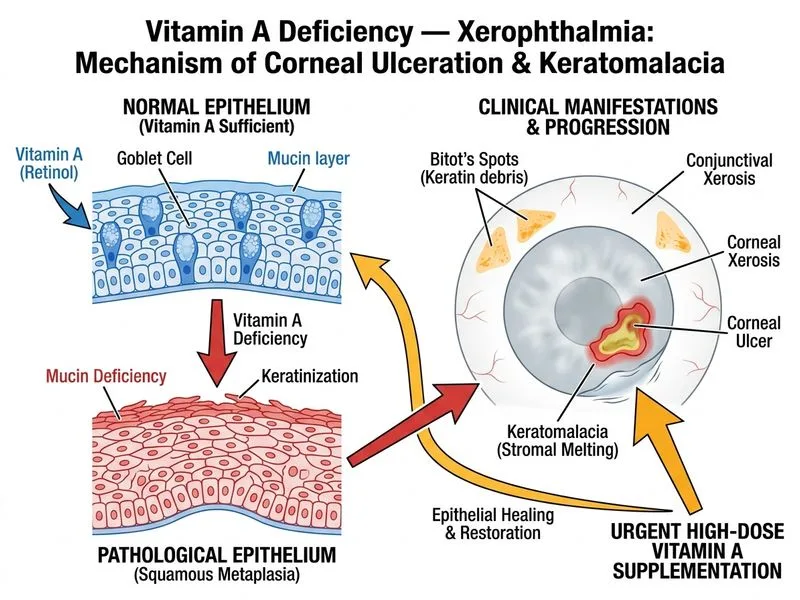
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.