Carbohydrate Metabolism — Glycolysis, TCA, ETC for NEET PG 2026
Master glycolysis, gluconeogenesis, glycogen metabolism, TCA cycle, ETC, oxidative phosphorylation, PPP, and G6PD deficiency for NEET PG 2026 biochemistry.
Quick Answer
Carbohydrate metabolism contributes 3 to 4 NEET PG questions per paper and is the densest biochemistry block — examiners reuse the same regulatory-enzyme, ATP-yield, and clinical-deficiency stems year after year. Lock these:
- Glycolysis — 3 irreversible steps (HK, PFK-1, PK); net 2 ATP anaerobic, 6 to 8 ATP aerobic.
- Gluconeogenesis — bypasses 3 irreversible glycolytic steps using G6Pase, F1,6BPase, PEPCK plus PC.
- Glycogen storage diseases — von Gierke (I), Pompe (II), Cori (III), Andersen (IV), McArdle (V), Hers (VI).
- TCA cycle — 3 NADH plus 1 FADH2 plus 1 GTP per pyruvate; regulated by NADH/CoA ratio.
- ETC — 4 complexes plus ATP synthase; chemiosmotic theory; uncouplers DNP, thermogenin.
- PPP — G6PDH rate-limiting; NADPH and ribose-5-P; deficiency causes hemolysis.
- Cori cycle — muscle lactate to liver glucose; 4 ATP cost per glucose.
Biochemistry feels heavy, but carbohydrate metabolism is the section with the highest yield per minute of study — pathways are linear, regulators are countable on one hand, and clinical correlates are clean (G6PD deficiency, McArdle, von Gierke). India-specific stems on G6PD-related fava-bean hemolysis and tropical-pancreatitis-related hyperglycemia keep this topic central to NEET PG.
This NEETPGAI deep dive walks through glycolysis, gluconeogenesis, glycogen metabolism, glycogen storage diseases, the TCA cycle, the electron transport chain and oxidative phosphorylation, the pentose phosphate pathway, the Cori cycle, and the most common NEET PG MCQ traps. Pair it with the lipid metabolism guide for a complete bioenergetics map.
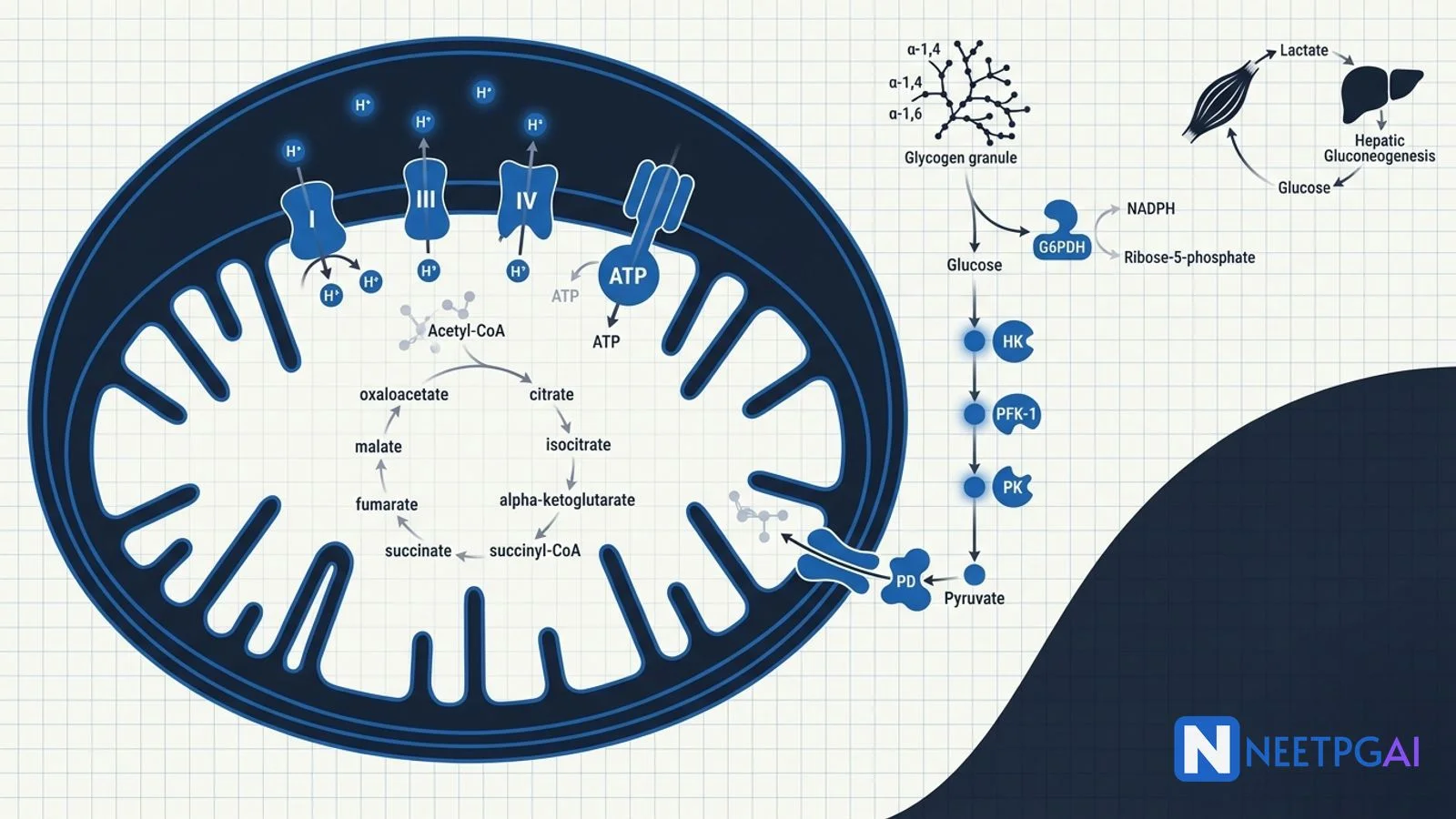
Glycolysis — the Embden-Meyerhof pathway
Glycolysis converts one glucose (6C) to two pyruvate (3C) in the cytoplasm — anaerobic or aerobic, ubiquitous to all cells.
Key steps
- Hexokinase / glucokinase — glucose → G6P; 1 ATP consumed; irreversible.
- PFK-1 — fructose-6-P → fructose-1,6-BP; 1 ATP consumed; irreversible; rate-limiting.
- Aldolase splits F1,6BP into DHAP and G3P (interconverted by triose-P-isomerase).
- G3P dehydrogenase — G3P → 1,3-BPG, produces 1 NADH (×2).
- Phosphoglycerate kinase — 1 ATP per triose (×2 = 2 ATP); substrate-level phosphorylation.
- Enolase — 2-PG → PEP; inhibited by fluoride (basis of grey-top sample tube for glucose).
- Pyruvate kinase — PEP → pyruvate; 1 ATP per triose (×2 = 2 ATP); irreversible.
Hexokinase vs glucokinase
| Feature | Hexokinase | Glucokinase |
|---|---|---|
| Tissue | All cells | Liver, pancreatic beta cells |
| Km / Vmax | Low / Low | High / High |
| Inhibition by G6P | Yes | No |
| Induction by insulin | No | Yes |
Regulation of PFK-1
Activators — AMP, fructose-2,6-bisphosphate (most potent). Inhibitors — ATP, citrate, low pH. F2,6-BP is made by PFK-2: kinase activity dominates when insulin is high (high glycolysis); fasting glucagon raises cAMP → PKA phosphorylates PFK-2 → its phosphatase activity dominates → F2,6-BP falls → glycolysis off, gluconeogenesis on.
ATP yield
- Net ATP from glycolysis = 4 produced (steps 7 and 10) minus 2 consumed (steps 1 and 3) = 2 ATP.
- Plus 2 NADH (each yielding 2.5 ATP via malate-aspartate shuttle or 1.5 via glycerol-phosphate shuttle).
Anaerobic vs aerobic
- Anaerobic — pyruvate → lactate via lactate dehydrogenase (regenerates NAD+). Total 2 ATP per glucose. Sites — red cells (no mitochondria), exercising muscle, hypoxic tissue.
- Aerobic — pyruvate → acetyl-CoA via pyruvate dehydrogenase → TCA. About 30 to 32 ATP per glucose.
Pyruvate dehydrogenase complex
Three enzymes (E1, E2, E3) plus five cofactors — TPP (B1), lipoate, CoA-SH (B5), FAD (B2), NAD+ (B3). B1 (thiamine) deficiency causes pyruvate accumulation → lactic acidosis (Wernicke's, beriberi). Arsenic poisoning inhibits PDH via lipoate.
Gluconeogenesis
Synthesises glucose from non-carbohydrate precursors (lactate, glycerol, glucogenic amino acids — alanine especially). Mostly liver (90 percent), some kidney cortex.
Bypasses the 3 irreversible steps of glycolysis —
- Pyruvate → oxaloacetate by pyruvate carboxylase (mitochondrial; biotin cofactor; activated by acetyl-CoA). OAA → malate → cytosol → OAA → PEP by PEPCK (cytosolic).
- Fructose-1,6-BP → fructose-6-P by fructose-1,6-bisphosphatase (cytosolic).
- Glucose-6-P → glucose by glucose-6-phosphatase (in ER; absent in muscle — muscle cannot release glucose).
Regulation
- Activators — glucagon, cortisol, fasting.
- Inhibitors — insulin, fed state.
- Acetyl-CoA activates PC; this is why fatty acid oxidation drives gluconeogenesis in fasting.
Cost
Gluconeogenesis costs 4 ATP plus 2 GTP plus 2 NADH per glucose synthesised.
Glycogen metabolism
Glycogen is the branched storage polysaccharide of glucose. Two depots:
- Liver — 100 g; maintains blood glucose.
- Muscle — 400 g; supplies muscle only (no G6Pase).
Synthesis (glycogenesis)
- UDP-glucose donor (formed from G1P plus UTP).
- Glycogen synthase — adds alpha-1,4 linkage. Rate-limiting.
- Branching enzyme (alpha-1,4 → alpha-1,6) — adds branches every 8 to 12 residues.
Breakdown (glycogenolysis)
- Glycogen phosphorylase — removes glucose-1-P from non-reducing ends; alpha-1,4 link. Rate-limiting. Cofactor PLP (B6).
- Debranching enzyme — has alpha-1,4-transferase plus alpha-1,6-glucosidase activities; resolves branch points.
Regulation
- Insulin — activates glycogen synthase (via dephosphorylation), inhibits phosphorylase. Glycogenesis.
- Glucagon, epinephrine — activate phosphorylase (via cAMP-PKA cascade), inhibit synthase. Glycogenolysis.
- Calcium and AMP — activate muscle phosphorylase during exercise.
Glycogen storage diseases (GSDs)
| Type | Name | Enzyme defect | Clue |
|---|---|---|---|
| I | von Gierke | Glucose-6-phosphatase | Severe fasting hypoglycemia, hepatomegaly, lactic acidosis |
| II | Pompe | Lysosomal alpha-1,4-glucosidase | Cardiomyopathy, hypotonia, "floppy baby" |
| III | Cori | Debranching enzyme | Milder hepatomegaly |
| IV | Andersen | Branching enzyme | Cirrhosis, early death |
| V | McArdle | Muscle phosphorylase | Exercise intolerance, second-wind, no rise in blood lactate |
| VI | Hers | Liver phosphorylase | Mild hepatomegaly |
| VII | Tarui | Muscle PFK | Exercise intolerance plus hemolysis |
TCA cycle (Krebs / citric acid cycle)
Eight reactions in the mitochondrial matrix. Per turn, oxidises one acetyl-CoA (2C) to 2 CO2 with the energy harvested as 3 NADH plus 1 FADH2 plus 1 GTP.
Key steps
- Citrate synthase — acetyl-CoA plus OAA → citrate.
- Isocitrate dehydrogenase — isocitrate → alpha-KG plus CO2 (1 NADH); rate-limiting.
- Alpha-KG dehydrogenase — alpha-KG → succinyl-CoA plus CO2 (1 NADH); same five cofactors as PDH.
- Succinyl-CoA synthetase — succinyl-CoA → succinate (1 GTP, substrate-level phosphorylation).
- Succinate dehydrogenase — succinate → fumarate (1 FADH2); only TCA enzyme on inner mitochondrial membrane (= complex II of ETC).
- Malate dehydrogenase — malate → OAA (1 NADH).
Regulation
- Citrate synthase — inhibited by ATP, NADH, citrate, succinyl-CoA.
- Isocitrate dehydrogenase (rate-limiting) — activated by ADP and Ca2+, inhibited by ATP and NADH.
- Alpha-KG dehydrogenase — inhibited by NADH, succinyl-CoA, ATP, activated by Ca2+.
Anaplerotic reactions
Replenish TCA intermediates withdrawn for biosynthesis. Main one — pyruvate carboxylase (pyruvate → OAA).
ATP yield per turn
3 NADH (3 × 2.5 = 7.5) plus 1 FADH2 (1 × 1.5) plus 1 GTP = 10 ATP per acetyl-CoA. Two acetyl-CoA per glucose = 20 ATP.
Electron transport chain and oxidative phosphorylation
Located on the inner mitochondrial membrane. Four complexes pump H+ from matrix to intermembrane space; ATP synthase (complex V) uses the gradient to make ATP.
| Complex | Name | Function | Inhibitors |
|---|---|---|---|
| I | NADH dehydrogenase | NADH → ubiquinone; 4 H+ pumped | Rotenone, amobarbital, MPP+ |
| II | Succinate dehydrogenase | FADH2 → ubiquinone; no H+ pumped | Malonate |
| III | Cytochrome bc1 | Ubiquinol → cyt c; 4 H+ pumped | Antimycin A |
| IV | Cytochrome c oxidase | Cyt c → O2 (final acceptor); 2 H+ pumped | Cyanide, carbon monoxide, sodium azide, H2S |
| V | ATP synthase | ADP plus Pi → ATP; uses H+ gradient | Oligomycin |
Chemiosmotic theory (Peter Mitchell, Nobel 1978)
Proton pumping by complexes I, III, IV creates an electrochemical gradient (proton-motive force). ATP synthase uses this gradient to phosphorylate ADP — the F0 component is a proton channel, F1 has catalytic sites.
ATP per electron pair
- NADH — 2.5 ATP (3 pumping complexes)
- FADH2 — 1.5 ATP (2 pumping complexes; bypasses complex I)
Uncouplers
Disrupt the proton gradient without inhibiting electron flow → heat generation instead of ATP.
- 2,4-DNP (dinitrophenol) — old weight-loss drug, withdrawn for fatal hyperthermia.
- Thermogenin (UCP-1) — physiological uncoupler in brown adipose tissue; generates heat in newborns and hibernating mammals.
- Aspirin overdose — uncouples at high doses; hyperthermia.
Shuttles
NADH from cytoplasm cannot cross inner mitochondrial membrane directly. Two shuttles —
- Malate-aspartate shuttle (heart, liver) — NADH delivered as NADH to mitochondrial matrix → 2.5 ATP.
- Glycerol-3-phosphate shuttle (skeletal muscle, brain) — NADH delivered as FADH2 → 1.5 ATP.
This is why total ATP yield is given as 30 to 32 depending on the tissue.
Pentose phosphate pathway (HMP shunt)
A cytoplasmic alternative to glycolysis. Two phases —
Oxidative phase (irreversible)
- Glucose-6-P → 6-phosphogluconolactone by glucose-6-phosphate dehydrogenase (G6PD). Produces NADPH. Rate-limiting.
- 6-PG-lactone → 6-PG → ribulose-5-P by 6-PG dehydrogenase. Produces NADPH plus CO2.
Non-oxidative phase (reversible)
Ribulose-5-P → ribose-5-P (for nucleotide synthesis) or fructose-6-P plus G3P (rejoins glycolysis) via transketolase and transaldolase.
Functions
- NADPH — for reductive biosyntheses (fatty acids, cholesterol, steroid hormones), maintaining reduced glutathione (antioxidant defence), respiratory burst in neutrophils via NADPH oxidase.
- Ribose-5-P — for nucleotide synthesis (DNA, RNA, ATP, NAD).
Key NEET PG cofactor
Transketolase needs TPP (vitamin B1) — basis of erythrocyte transketolase activity test for thiamine deficiency.
G6PD deficiency
- X-linked; most common enzyme defect worldwide (400 million carriers).
- Indian, Mediterranean, African populations.
- Triggers — oxidative stress from drugs (sulphonamides, dapsone, primaquine, nitrofurantoin), fava beans (favism), infection.
- Mechanism — NADPH falls → reduced glutathione falls → oxidised Hb forms Heinz bodies (visible with supravital stain) → splenic macrophages bite out the inclusions creating bite cells.
- Presentation — acute intravascular hemolysis (hemoglobinuria, dark urine, jaundice) 1 to 3 days after trigger.
- Treatment — avoid triggers; transfusion for severe hemolysis.
Cori cycle and alanine cycle
Cori cycle — exercising muscle and RBCs perform anaerobic glycolysis → pyruvate → lactate (via LDH). Lactate exported to liver → pyruvate → glucose via gluconeogenesis. Glucose returned to muscle. Net energy cost — muscle gains 2 ATP, liver spends 6 ATP → net 4 ATP cost. Repays oxygen debt post-exercise.
Alanine cycle — muscle protein breakdown → amino acids → glutamate → alanine by transamination. Alanine to liver → pyruvate → glucose. Also delivers amino-nitrogen to liver for urea synthesis.
NEET PG MCQ traps
- PFK-1 is the rate-limiting enzyme of glycolysis; activated by F2,6-BP and AMP.
- Fluoride inhibits enolase — why glucose samples use grey-top tubes.
- Hexokinase is inhibited by G6P; glucokinase is not.
- PDH cofactors — TPP, lipoate, CoA, FAD, NAD; arsenic inhibits via lipoate.
- Muscle lacks G6Pase — cannot release glucose; only used locally.
- McArdle (GSD V) — no blood lactate rise on exercise; "second-wind".
- von Gierke (GSD I) — severe fasting hypoglycemia, lactic acidosis, hyperuricemia.
- Pompe (GSD II) — only GSD with lysosomal enzyme defect; cardiac involvement.
- Isocitrate dehydrogenase is the rate-limiting TCA step.
- Succinate dehydrogenase is the only TCA enzyme on the inner membrane and is complex II of ETC.
- Complex IV is inhibited by cyanide, CO, sodium azide, H2S.
- DNP and thermogenin uncouple ETC from ATP synthesis — heat without ATP.
- Malate-aspartate shuttle in heart/liver delivers cytoplasmic NADH at full 2.5 ATP value.
- G6PD deficiency — Heinz bodies, bite cells, X-linked, drug-triggered hemolysis.
- Cori cycle costs liver 4 ATP per glucose released.
Recent updates and Indian context
- NMC CBME 2024 — biochemistry teaching emphasises clinical correlates over rote pathways; NEET PG favours integrated stems linking biochemistry deficit to disease presentation.
- G6PD deficiency in India — prevalence 5 to 15 percent in tribal and northern populations; routine screening before dapsone and primaquine therapy.
- Tropical pancreatitis — Indian-subcontinent endemic chronic pancreatitis (Kerala, Tamil Nadu) causing fibrocalcific pancreatic diabetes.
- NEXT — expects pathway diagrams paired with disease vignettes; recent INI-CET trends favour PDH cofactor questions and ETC inhibitor identification.
Frequently asked questions
What are the three irreversible steps of glycolysis?
The three irreversible (regulatory) steps of glycolysis are catalysed by hexokinase (glucokinase in liver), phosphofructokinase-1 (the rate-limiting enzyme, controlled by ATP/AMP and fructose-2,6-bisphosphate), and pyruvate kinase. These three steps are bypassed in gluconeogenesis using different enzymes — glucose-6-phosphatase, fructose-1,6-bisphosphatase, and the pyruvate-carboxylase plus PEP-carboxykinase pair.
What is the net ATP yield of complete glucose oxidation?
Complete aerobic oxidation of one glucose molecule yields about 30 to 32 ATP — 2 net ATP from glycolysis, 2 ATP from TCA (one per pyruvate), 6 ATP from NADH in glycolysis (3 ATP each, modified by shuttle), 6 ATP from NADH in pyruvate decarboxylation, 18 ATP from NADH in TCA, and 4 ATP from FADH2 in TCA. Anaerobic glycolysis yields only 2 ATP.
How does G6PD deficiency cause hemolysis?
Glucose-6-phosphate dehydrogenase is the rate-limiting enzyme of the pentose phosphate pathway, generating NADPH. NADPH maintains reduced glutathione, which detoxifies hydrogen peroxide. In G6PD deficiency, oxidative stress (drugs, fava beans, infection) overwhelms the antioxidant defence — hemoglobin denatures (Heinz bodies), red cells become rigid (bite cells), and intravascular hemolysis follows. X-linked; common in Mediterranean and African populations.
What is the Cori cycle?
The Cori cycle is the lactate-glucose shuttle between exercising muscle (or red cells) and liver. Muscle generates lactate from glucose by anaerobic glycolysis. Lactate is exported to the liver, where gluconeogenesis converts it back to glucose, which is released to blood and re-uptaken by muscle. The cycle costs the liver 4 ATP per glucose produced — energy debt of anaerobic exercise.
Name the glycogen storage diseases and their enzyme defects.
Type I (von Gierke) — glucose-6-phosphatase; hepatomegaly, fasting hypoglycemia. Type II (Pompe) — lysosomal alpha-1,4-glucosidase (acid maltase); cardiomyopathy, hypotonic infant. Type III (Cori) — debranching enzyme; milder hepatomegaly. Type IV (Andersen) — branching enzyme; cirrhosis. Type V (McArdle) — muscle phosphorylase; exercise intolerance, no rise in blood lactate. Type VI (Hers) — liver phosphorylase; mild hepatomegaly.
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Written by: NEETPGAI Editorial Team Reviewed by: Pending SME Review Last reviewed: May 2026
Ready to put this into practice?
Start practicing NEET PG MCQs with AI-powered explanations.
Start Free PracticeYour Next Step
Related Study Guides
Anxiety Disorders, OCD & PTSD for NEET PG 2026: Diagnosis, SSRI, CBT
Master anxiety, OCD, and PTSD for NEET PG 2026 — DSM-5 criteria, Y-BOCS, SSRI first-line, exposure-response prevention, ECT indications, India NMHS data.
Cardiovascular Physiology and Cardiac Cycle for NEET PG 2026
Master cardiac cycle, Wiggers diagram, ECG basis, heart sounds, preload-afterload, Starling's law, JVP waves, and CO measurement for NEET PG 2026 — high-yield MCQ traps.
Acute Appendicitis Management for NEET PG 2026: Diagnosis & Surgery
Master acute appendicitis for NEET PG 2026 — pathophysiology, Alvarado score, imaging, laparoscopic appendicectomy, antibiotic-only therapy, complications, MCQ traps.
Join our NEET PG community
Daily MCQs, study tips, and topper strategies on Telegram.
Join on Telegram →