Image MCQ Walkthrough: Dermatology Vesiculobullous Diseases — Pemphigus, Pemphigoid, DH and More (NEET PG)
Step-by-step vesiculobullous skin disease image interpretation for NEET PG: tense vs flaccid bullae, Nikolsky sign positive vs negative, DIF patterns (intercellular net, linear BMZ, granular BMZ), histology level (intraepidermal vs subepidermal), and a full comparison table across pemphigus vulgaris, bullous pemphigoid, dermatitis herpetiformis, linear IgA disease, and SJS/TEN with practice MCQs.
Version 1.0 — Published March 2026
Quick Answer
Vesiculobullous diseases are autoimmune or drug-induced blistering disorders distinguished by the level of epidermal split, bulla tension, Nikolsky sign, and direct immunofluorescence (DIF) pattern. To correctly interpret vesiculobullous MCQs in NEET PG, master these 5 pattern groups:
- Bulla tension — flaccid (intraepidermal; pemphigus vulgaris, pemphigus foliaceus) vs tense (subepidermal; bullous pemphigoid, DH, linear IgA, EBA)
- Nikolsky sign — positive in intraepidermal splits (PV, PF) AND epidermal necrolysis (SJS/TEN, SSSS); negative in subepidermal splits (BP, DH, linear IgA)
- Histology level — suprabasal split with tombstone row (PV), subcorneal split (PF), subepidermal with neutrophilic microabscesses at dermal papillae tips (DH), subepidermal with eosinophilic infiltrate (BP)
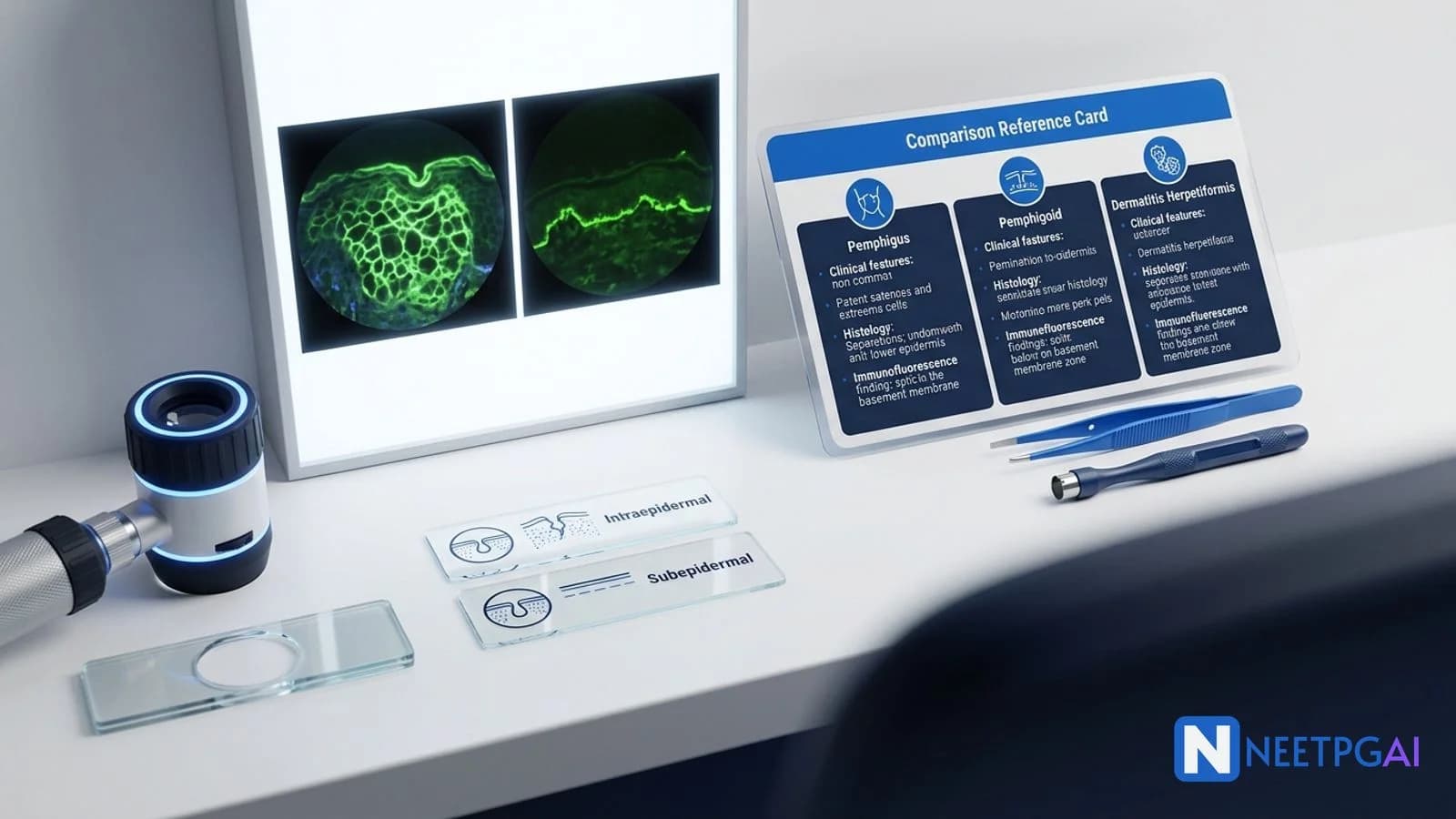
- DIF pattern — intercellular net-like IgG/C3 (pemphigus), linear IgG/C3 at BMZ (bullous pemphigoid and linear IgA — linear IgA only has IgA), granular IgA at dermal papillae (DH)
- Clinical distribution — mucosal-first flaccid blistering (PV), flexural tense bullae in elderly (BP), itchy grouped extensor vesicles (DH), annular "string-of-pearls" vesicles (linear IgA), widespread epidermal sloughing with mucosa (SJS/TEN)
Clinical image presentation
A 52-year-old man presents to the dermatology outpatient clinic with a 6-week history of painful oral erosions that have progressed to involve the lips, buccal mucosa, and hard palate. He has difficulty eating and has lost 4 kg. Over the past 2 weeks, flaccid blisters have appeared on the scalp, upper chest, and back — they rupture within hours of forming, leaving raw, weeping erosions that slowly re-epithelialize. No significant past medical history. No recent medication changes. No family history of skin disease.
On examination: vitals normal, temperature 37.4 C. Extensive oral mucosal erosions involving buccal mucosa, tongue, lips, and soft palate — the hard palate shows denuded epithelium. On the scalp, upper chest, and interscapular region: multiple flaccid, easily ruptured bullae on apparently normal skin, with widespread shallow erosions and crusting. Peri-lesional skin demonstrates a positive Nikolsky sign — lateral pressure causes epidermal slide. Asboe-Hansen sign is positive — lateral pressure on an existing intact bulla extends it into adjacent normal skin.
A student interpreting the dermatology photograph and clinical history should systematically identify:
Lesion morphology:
- Flaccid bullae (roof thin, easily ruptured, often only erosions visible)
- No tense, dome-shaped intact blisters
- No grouped vesicles
- Widespread erosions without new vesicle formation at the edges
Lesion distribution:
- Mucosal-dominant (oral, sometimes conjunctival, genital) — often the presenting and most severe site
- Cutaneous lesions on scalp, upper chest, back — seborrheic distribution
- Not flexural (rules out BP)
- Not extensor/grouped (rules out DH)
- Not annular with peripheral vesicle rim (rules out linear IgA)
Bedside signs:
- Nikolsky sign POSITIVE — indicates loss of intercellular cohesion (epidermal split)
- Asboe-Hansen sign POSITIVE — lateral bulla extension from pressure
Age and course:
- 52-year-old adult (middle age — typical PV; BP is elderly above 70; DH is young adult 20-40)
- 6-week chronic progressive course (rules out acute drug reaction)
Investigations ordered:
- Skin biopsy (H&E) from a fresh blister: suprabasal acantholysis with basal keratinocytes lined up in a tombstone row along the floor of the intraepidermal blister cavity; rounded acantholytic cells within the blister cavity
- Perilesional skin biopsy for DIF: intercellular IgG and C3 deposition in a net-like (fishnet) pattern throughout the epidermis
- Serum indirect immunofluorescence (IIF) on monkey esophagus: circulating anti-desmoglein 3 antibodies, titer 1:640
- ELISA: anti-desmoglein 3 (Dsg3) antibody positive at high titer; anti-desmoglein 1 (Dsg1) negative (mucosal-dominant PV)
MCQ question as it appears in NEET PG
A 52-year-old man presents with a 6-week history of painful oral erosions that are worsening, and 2 weeks of flaccid blisters on the scalp, chest, and back. The blisters rupture within hours. Nikolsky sign is positive on peri-lesional skin. Histology shows suprabasal acantholysis with a tombstone row of basal keratinocytes. DIF of peri-lesional skin shows intercellular IgG and C3 in a fishnet pattern. Which of the following is the most likely diagnosis and its target antigen?
- (a) Bullous pemphigoid — IgG against BP180 (hemidesmosome)
- (b) Pemphigus vulgaris — IgG against desmoglein 3
- (c) Dermatitis herpetiformis — IgA against epidermal transglutaminase (TG3)
- (d) Linear IgA bullous dermatosis — IgA against BP180
Take a moment to work through this before reading the analysis below.
Step-by-step visual analysis
A systematic reading protocol is critical — missing a single criterion (bulla tension, Nikolsky, DIF) can push you toward the wrong diagnosis. Use this protocol every time a vesiculobullous image or case appears in an NEET PG MCQ.
Step 1: Assess bulla morphology — flaccid vs tense
Bulla tension directly predicts the level of epidermal split.
| Feature | Flaccid bullae | Tense bullae |
|---|---|---|
| Appearance | Thin-roofed, wrinkled, often ruptured | Dome-shaped, firm, intact for days |
| Split level | Intraepidermal | Subepidermal (below basement membrane in some; at lamina lucida in others) |
| Diseases | Pemphigus vulgaris, pemphigus foliaceus | Bullous pemphigoid, dermatitis herpetiformis, linear IgA disease, epidermolysis bullosa acquisita, bullous lupus |
| Roof contents | Partial epidermis (few layers) | Full epidermis |
In this patient: flaccid bullae → intraepidermal disease (pemphigus family).
Step 2: Test Nikolsky sign
- Positive Nikolsky = loss of intercellular cohesion in epidermis; characteristic of:
- Intraepidermal blistering (pemphigus vulgaris, pemphigus foliaceus)
- Epidermal necrolysis (SJS/TEN, staphylococcal scalded skin syndrome, severe burns)
- Negative Nikolsky = intact epidermis; characteristic of:
- Subepidermal blistering (bullous pemphigoid, dermatitis herpetiformis, linear IgA)
Asboe-Hansen sign (lateral extension of existing bulla by pressure) is the positive-Nikolsky equivalent applied to an intact bulla — positive in pemphigus.
In this patient: Nikolsky positive + flaccid bullae + chronic course with mucosal involvement → pemphigus vulgaris (not SJS/TEN which would be acute with widespread necrolysis).
Step 3: Correlate clinical distribution
Distribution narrows the differential dramatically.
| Distribution | Likely diagnosis |
|---|---|
| Mucosal-dominant, flaccid bullae, scalp/chest/back erosions, middle-age | Pemphigus vulgaris |
| Seborrheic distribution, subcorneal flaccid bullae, no mucosal involvement | Pemphigus foliaceus |
| Flexural tense bullae, itchy, elderly (> 70 y), urticarial plaques preceding bullae | Bullous pemphigoid |
| Grouped itchy vesicles on extensors (elbows, knees, buttocks, scalp), young adult | Dermatitis herpetiformis |
| Annular "string-of-pearls" vesicle rim, children or adults, may be vancomycin-induced | Linear IgA bullous dermatosis |
| Widespread erythema + skin sloughing + mucosal lesions within 1-3 weeks of a drug | SJS/TEN |
| Subungual and trauma-site bullae with milia and scarring | Epidermolysis bullosa acquisita |
In this patient: mucosal-dominant + flaccid + seborrheic cutaneous distribution + middle-age → pemphigus vulgaris.
Step 4: Review histology level
| Split level | Disease | Histologic hallmark |
|---|---|---|
| Subcorneal (just below stratum corneum) | Pemphigus foliaceus, staphylococcal scalded skin syndrome, bullous impetigo | Split only in superficial epidermis |
| Suprabasal (just above basal cell layer) | Pemphigus vulgaris | Tombstone row of basal cells along blister floor; acantholytic cells in cavity |
| Full-thickness epidermal necrosis | SJS/TEN | Dead keratinocytes full thickness; subepidermal detachment secondary |
| Subepidermal, lamina lucida | Bullous pemphigoid (eosinophil-rich), linear IgA, dermatitis herpetiformis (neutrophils at dermal papillae tips) | Split at BMZ; intact epidermis forms roof |
| Subepidermal, sublamina densa | Epidermolysis bullosa acquisita, bullous lupus | Split below basement membrane; scarring tendency |
In this patient: suprabasal split with tombstone row → pemphigus vulgaris.
Step 5: Interpret DIF pattern
DIF on peri-lesional skin is the single most discriminatory test in vesiculobullous disease.
| DIF pattern | Disease | Target antigen |
|---|---|---|
| Intercellular IgG + C3, net-like throughout epidermis | Pemphigus vulgaris | Desmoglein 3 (± Dsg 1 in mucocutaneous PV) |
| Intercellular IgG + C3 in superficial epidermis only | Pemphigus foliaceus | Desmoglein 1 |
| Linear IgG + C3 at basement membrane zone | Bullous pemphigoid | BP180 (collagen XVII), BP230 hemidesmosome |
| Linear IgA at basement membrane zone | Linear IgA bullous dermatosis | BP180 (LAD-1 fragment) |
| Granular IgA at dermal papillae tips | Dermatitis herpetiformis | Epidermal transglutaminase (TG3) |
| Linear IgG at BMZ with dermal-side localization on salt-split skin | Epidermolysis bullosa acquisita | Type VII collagen (anchoring fibrils) |
In this patient: intercellular IgG + C3 fishnet → pemphigus vulgaris, confirmed.
Step 6: Match to serology
- Anti-desmoglein 3 ELISA: positive in PV (mucosal + cutaneous or mucosal-only PV)
- Anti-desmoglein 1 ELISA: positive in pemphigus foliaceus and mucocutaneous PV
- Anti-BP180 and anti-BP230 ELISA: positive in bullous pemphigoid
- Anti-tissue transglutaminase (TG2) and anti-epidermal transglutaminase (TG3) IgA: positive in DH (and 90 percent have celiac disease with anti-TG2 positivity)
In this patient: anti-Dsg3 positive at 1:640 → confirms mucocutaneous pemphigus vulgaris.
Answer and detailed explanation
Correct answer: (b) Pemphigus vulgaris — IgG against desmoglein 3
This patient has classic mucocutaneous pemphigus vulgaris. Mucosal-dominant presentation, flaccid bullae, positive Nikolsky, suprabasal acantholysis with tombstone row on histology, and intercellular IgG/C3 fishnet DIF with high-titer anti-Dsg3 ELISA are pathognomonic. Pemphigus vulgaris is driven by IgG autoantibodies against desmoglein 3 (mucosal form) or desmoglein 1 and 3 (mucocutaneous form). Desmoglein 3 is the dominant desmosomal cadherin in mucosa and the deep epidermis — its loss disrupts keratinocyte-keratinocyte adhesion suprabasally.
Why each distractor is wrong:
| Option | Why incorrect |
|---|---|
| (a) Bullous pemphigoid — IgG against BP180 | BP is a subepidermal disease with tense intact bullae in elderly patients, predominantly flexural, with negative Nikolsky. DIF shows linear IgG and C3 at BMZ, not intercellular net. Histology shows subepidermal split with eosinophils, not suprabasal acantholysis. |
| (c) Dermatitis herpetiformis — IgA against TG3 | DH presents as grouped, intensely itchy vesicles on extensor surfaces in young adults with celiac-spectrum disease. DIF shows granular IgA at dermal papillae, not intercellular net. Mucosal involvement is rare. Nikolsky is negative. |
| (d) Linear IgA — IgA against BP180 (LAD-1) | Linear IgA disease shows tense bullae in an annular "string-of-pearls" configuration with peripheral vesicle rim, often drug-induced (vancomycin). DIF shows linear IgA at BMZ, not intercellular net. Nikolsky is negative. |
NEET PG trap alert: The commonest wrong answer in a mucocutaneous bullous disease vignette is "bullous pemphigoid" because both diseases involve IgG. Remember: bullous pemphigoid is a subepidermal, Nikolsky-negative, tense-bulla, elderly, flexural, pruritic disease with linear DIF. Pemphigus vulgaris is intraepidermal, Nikolsky-positive, flaccid-bulla, middle-aged, mucocutaneous, with intercellular fishnet DIF. The three C's for pemphigus: Cohesion loss (Nikolsky+), Caudal-first (mucosa first), Crusting shallow erosions.
Practice dermatology MCQs with AI-powered explanations to build visual and DIF pattern recognition. For a full review, see the dermatology high-yield topics guide and the related psoriasis vs eczema image MCQ walkthrough.
Similar patterns comparison table
The five vesiculobullous diseases most commonly tested in NEET PG — memorize this comparison table, it covers approximately 90 percent of vesiculobullous image MCQs:
| Feature | Pemphigus vulgaris | Bullous pemphigoid | Dermatitis herpetiformis | Linear IgA | SJS/TEN |
|---|---|---|---|---|---|
| Typical age | 40-60 y | Above 70 y | 20-40 y | Children or adults | Any; often drug-related |
| Cause | IgG vs desmoglein 3 (± Dsg 1) | IgG vs BP180, BP230 | IgA vs TG3 (celiac-associated) | IgA vs BP180 (LAD-1) | Drug reaction; keratinocyte apoptosis |
| Bulla type | Flaccid, ruptures fast | Tense, intact days | Grouped tiny vesicles, often excoriated | Tense, "string-of-pearls" annular rim | Flaccid on erythema, full-thickness necrosis |
| Nikolsky sign | Positive | Negative | Negative | Negative | Positive (on diseased skin) |
| Asboe-Hansen sign | Positive | Negative | Negative | Negative | Positive |
| Mucosal involvement | >= 90 percent (first and severe) | 10-20 percent (mild) | Rare | 50 percent | > 90 percent (lips, mouth, eyes, genitals) |
| Itch | Mild | Severe (pre-bullous phase) | Severe (herpetiform) | Severe | Painful more than itchy |
| Distribution | Oral + scalp/chest/back (seborrheic) | Flexural (axillae, groin, inner thighs) | Extensor (elbows, knees, buttocks, scalp) | Trunk, flexural, acral | Face, trunk, extremities with mucosal |
| Histology level | Suprabasal (tombstone row) | Subepidermal (eosinophils) | Subepidermal (neutrophils at dermal papillae tips) | Subepidermal (neutrophils) | Full-thickness epidermal necrosis |
| DIF | Intercellular IgG + C3 fishnet | Linear IgG + C3 at BMZ | Granular IgA at dermal papillae | Linear IgA at BMZ | Usually negative; may show linear C3 non-specifically |
| Serology | Anti-Dsg3 (± Dsg1) ELISA | Anti-BP180, anti-BP230 ELISA | Anti-TG2, anti-TG3, anti-endomysial IgA | Anti-BP180 (LAD-1) | None specific |
| Associated conditions | Autoimmune (thyroid, myasthenia gravis rare) |
Clinical application: how to approach a vesiculobullous image in the exam
The systematic approach below solves 90 percent of NEET PG vesiculobullous image questions in under 90 seconds.
| Step | Question to ask | Answer narrows to |
|---|---|---|
| 1 | Tense or flaccid bullae? | Flaccid → pemphigus family; Tense → subepidermal family |
| 2 | Nikolsky sign positive or negative? | Positive → PV, PF, SJS/TEN, SSSS; Negative → BP, DH, linear IgA, EBA |
| 3 | Mucosal involvement prominent? | Yes + flaccid → PV; Yes + erythema sloughing → SJS/TEN; Rare → DH |
| 4 | Where are the lesions? | Flexural elderly → BP; Extensor young + itchy → DH; Annular "string-of-pearls" → linear IgA; Seborrheic mucocutaneous → PV |
| 5 | What is the histology level? | Suprabasal tombstone → PV; Subcorneal → PF; Subepidermal eosinophilic → BP; Subepidermal neutrophilic at papillae → DH; Full-thickness necrosis → TEN |
| 6 | What is the DIF pattern? | Intercellular fishnet → pemphigus; Linear IgG BMZ → BP; Linear IgA BMZ → linear IgA; Granular IgA papillae → DH |
| 7 | Match serology and treatment | Dsg3 → PV; BP180/BP230 → BP; TG2/TG3 → DH; No serology → linear IgA or TEN |
Frequently asked questions
What is the difference between tense and flaccid bullae and why does it matter?
Bulla tension is a direct clinical clue to the histologic level of blister formation. Flaccid bullae (easily ruptured, roof thin, often only erosions visible) indicate an intraepidermal split where the blister roof is just a few cell layers — classic of pemphigus vulgaris (suprabasal split) and pemphigus foliaceus (subcorneal split). Tense bullae (firm, intact, dome-shaped, persist for days) indicate a subepidermal split where the entire epidermis forms the roof — classic of bullous pemphigoid, dermatitis herpetiformis, linear IgA disease, epidermolysis bullosa acquisita, and bullous lupus. The single clinical sign of bulla tension reliably predicts the split level and narrows the differential by 50 percent before DIF.
How is Nikolsky sign elicited and what does it mean?
Nikolsky sign is the induction of epidermal detachment by lateral pressure on apparently normal or peri-lesional skin. Positive Nikolsky indicates loss of intercellular cohesion in the epidermis — a feature of intraepidermal blistering diseases (pemphigus vulgaris, pemphigus foliaceus) and acute epidermal necrolysis (SJS/TEN, staphylococcal scalded skin syndrome). Asboe-Hansen sign is related — lateral extension of an existing bulla with pressure, also positive in pemphigus. Negative Nikolsky is typical of subepidermal diseases (bullous pemphigoid, dermatitis herpetiformis, linear IgA). Key NEET PG trap: Nikolsky positive does NOT mean pemphigus by default — TEN, SSSS, and severe burns also show positive Nikolsky, and context distinguishes them.
What are the three direct immunofluorescence (DIF) patterns in vesiculobullous diseases?
DIF on peri-lesional skin shows three diagnostic patterns. First, intercellular IgG and C3 deposition in a net-like pattern throughout the epidermis — diagnostic of pemphigus vulgaris (IgG against desmoglein 3) and pemphigus foliaceus (IgG against desmoglein 1). Second, linear IgG and C3 at the basement membrane zone (BMZ) — diagnostic of bullous pemphigoid (IgG against BP180 and BP230 hemidesmosomes). A similar linear pattern with IgA alone is diagnostic of linear IgA disease. Third, granular IgA deposition in dermal papillae — pathognomonic of dermatitis herpetiformis (IgA against epidermal transglutaminase TG3). EBA (epidermolysis bullosa acquisita) shows linear IgG at BMZ like BP but on salt-split skin the deposits localize to the dermal side (vs epidermal side in BP).
What is the pathological level of blister formation in each major vesiculobullous disease?
Intraepidermal split diseases (flaccid bullae, Nikolsky positive): pemphigus vulgaris splits suprabasally (above basal cells, leaving tombstone row), pemphigus foliaceus splits subcorneally (just below stratum corneum), staphylococcal scalded skin syndrome splits in stratum granulosum (exfoliative toxin cleaves desmoglein 1), Hailey-Hailey shows full-thickness acantholysis (dilapidated brick wall). Subepidermal split diseases (tense bullae, Nikolsky negative): bullous pemphigoid splits at the lamina lucida (above PAS-positive basement membrane), dermatitis herpetiformis and linear IgA split at the lamina lucida, epidermolysis bullosa acquisita splits below the lamina densa (sublamina densa). SJS/TEN shows full-thickness epidermal necrosis — the split is at the dermo-epidermal junction because the entire epidermis is dead.
How is pemphigus vulgaris clinically distinguished from bullous pemphigoid?
Six clinical features separate PV from BP. Age: PV affects 40-60 years; BP affects elderly (above 70 years). Mucosal involvement: PV has almost 100 percent mucosal (oral, conjunctival, genital) — often the presenting feature; BP has only 10-20 percent mucosal. Bulla type: PV has flaccid bullae with widespread erosions because bullae rupture fast; BP has tense intact bullae that last days. Nikolsky sign: positive in PV, negative in BP. Itching: mild in PV, severe in BP (often precedes bullae by weeks — 'pre-bullous pemphigoid' phase). Mortality: untreated PV mortality is 60-90 percent (lethal disease before steroids); untreated BP is self-limiting over 1-5 years with 10-20 percent mortality mostly from comorbidities in the elderly.
What is the classic histology of pemphigus vulgaris?
Pemphigus vulgaris histology shows three pathognomonic features. First, suprabasal acantholysis — loss of desmosomes between keratinocytes creates an intraepidermal split just above the basal cell layer. Second, tombstone appearance — the basal keratinocytes remain attached to the basement membrane but lose lateral attachments to their neighbors, lining up like tombstones along the floor of the blister cavity. Third, acantholytic cells (Tzanck cells) within the blister cavity — rounded keratinocytes that have lost their intercellular connections. Tzanck smear from a fresh blister shows these rounded acantholytic cells (also seen in viral blisters — HSV, VZV — but without tombstone histology). DIF is diagnostic: intercellular IgG and C3 net-like pattern.
How is dermatitis herpetiformis linked to celiac disease and how is it treated?
Dermatitis herpetiformis (DH) is the cutaneous manifestation of gluten sensitivity — 90 percent of DH patients have small bowel villous atrophy (often subclinical). Both conditions are driven by IgA antibodies against tissue transglutaminase (TG2 in gut, TG3 in skin). DH presents as intensely itchy, grouped vesicles on extensor surfaces (elbows, knees, buttocks, scalp) — the grouped herpetiform distribution is the name origin. DIF shows pathognomonic granular IgA in dermal papillae. Treatment: strict lifelong gluten-free diet (addresses both skin and gut disease); dapsone 50-100 mg/day provides rapid symptomatic relief within 24-48 hours but does NOT address the underlying gluten enteropathy. G6PD screen is mandatory before dapsone (risk of hemolytic anemia in deficient patients).
How is vesiculobullous dermatology tested in NEET PG?
NBE tests vesiculobullous diseases through five patterns: clinical photograph recognition with bulla type (flaccid vs tense) and distribution (flexural in BP, extensor in DH, mucosal in PV), Nikolsky sign interpretation (positive in PV, SJS/TEN, SSSS; negative in BP, DH, linear IgA), histology level recognition (suprabasal in PV, subcorneal in PF, subepidermal in BP/DH/linear IgA), DIF pattern matching (intercellular net in pemphigus, linear BMZ in BP/linear IgA, granular BMZ in DH), and treatment choice (steroids for PV and BP, gluten-free diet plus dapsone for DH, withdraw offending drug plus supportive care in SCORTEN ICU for SJS/TEN). Expect 2-3 vesiculobullous questions per NEET PG paper in the dermatology section.
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Sources and references
- Bolognia JL, Schaffer JV, Cerroni L, Dermatology, 4th Edition (Elsevier, 2018) — comprehensive reference for autoimmune bullous diseases including histology, DIF patterns, and treatment algorithms.
- Schmidt E, Kasperkiewicz M, Joly P, "Pemphigus," Lancet, 2019 — definitive review on pemphigus vulgaris pathogenesis, diagnosis, and first-line rituximab therapy.
- IADVL Textbook of Dermatology, 5th Edition (Bhalani Publishing, 2022) — Indian standard dermatology reference with clinical photographs and DIF pattern recognition chapters for NEET PG preparation.
Strengthen your dermatology image pattern recognition by working through vesiculobullous and papulosquamous cases. Review the dermatology subject page, deepen psoriasis-vs-eczema reasoning with the dermatology psoriasis vs eczema image MCQ walkthrough, and drill targeted dermatology MCQs on NEETPGAI. Ready for unlimited AI-powered MCQs with detailed explanations? Explore NEETPGAI Pro.
For personalized study guidance on dermatology image pattern recognition, try the AI Tutor — it adapts to your weak areas and explains concepts the way a senior resident would.
Written by: NEETPGAI Editorial Team Reviewed by: Pending SME Review Last reviewed: March 2026
This article is reviewed by qualified medical professionals for clinical accuracy and exam relevance. For corrections or updates, contact the editorial team.
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Ready to put this into practice?
Start practicing NEET PG MCQs with AI-powered explanations.
Start Free PracticeYour Next Step
Related Study Guides
Image MCQ: Pediatric Imaging Findings for NEET PG (Intussusception, Pyloric Stenosis, Hirschsprung, VUR, DDH)
5 pediatric imaging MCQs for NEET PG: intussusception target sign, hypertrophic pyloric stenosis string sign, Hirschsprung contrast enema, VUR grading on MCUG, DDH Graf alpha angle.
Leprosy (Hansen Disease) Classification and MDT for NEET PG 2026
Master Ridley-Jopling spectrum, WHO PB/MB classification, lepromin test, slit-skin smear, WHO MDT, reactions and NLEP for NEET PG 2026.
14 Common Mistakes in Dermatology for NEET PG — And How to Avoid Them
Avoid the costliest dermatology mistakes in NEET PG 2026: psoriasis vs eczema, pemphigus vs pemphigoid, SJS vs TEN, leprosy, vitiligo, scabies, acne, hair loss, nail signs — all decoded.
Join our NEET PG community
Daily MCQs, study tips, and topper strategies on Telegram.
Join on Telegram →