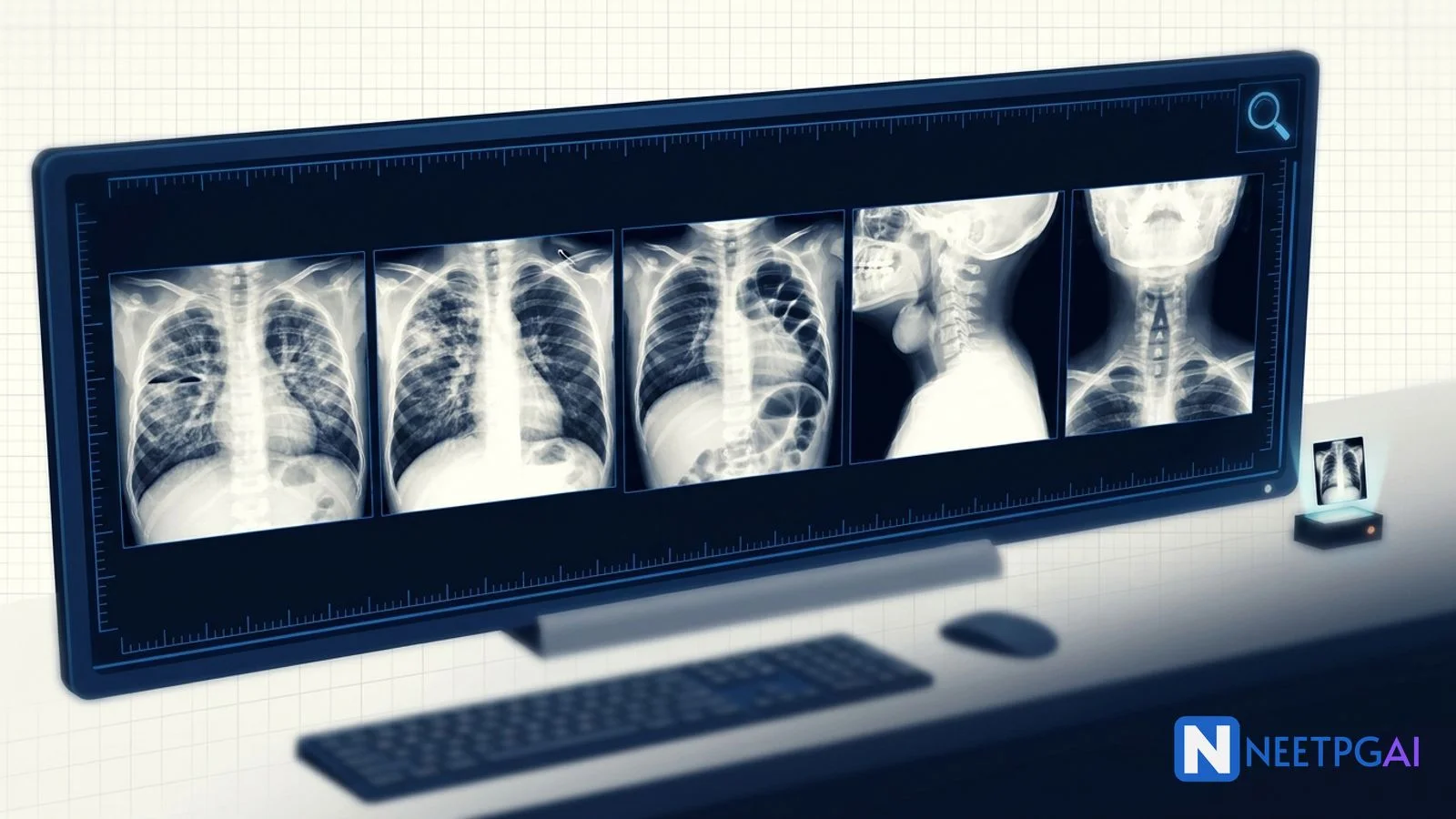
Image MCQ: Pediatric X-Ray Findings for NEET PG (Hyaline Membrane Disease, Meconium Aspiration, Congenital Diaphragmatic Hernia, Epiglottitis, Croup)
5 high-yield pediatric X-ray image MCQs for NEET PG: HMD ground-glass, MAS patchy infiltrates, CDH bowel-in-thorax, epiglottitis thumbprint, croup steeple sign — with teaching pearls.
Version 1.0 — Published May 2026
Quick Answer
Pediatric X-ray pattern recognition contributes 3-5 questions per NEET PG paper across pediatrics, neonatology, and radiology. Five patterns recur reliably:
- Hyaline membrane disease (HMD / neonatal RDS) — preterm under 34 weeks, surfactant deficiency, diffuse ground-glass + air bronchograms, low lung volumes
- Meconium aspiration syndrome (MAS) — term/post-term, meconium-stained liquor, patchy coarse infiltrates with hyperinflation, often with pneumothorax
- Congenital diaphragmatic hernia (CDH) — bowel loops in thorax, mediastinal shift, scaphoid abdomen, left-sided in 80-90 percent
- Epiglottitis — lateral neck X-ray thumbprint sign, tripod posture, drooling, high fever, Hib in unvaccinated
- Croup (laryngotracheobronchitis) — AP neck X-ray steeple sign, barking cough, inspiratory stridor, parainfluenza
Pair age plus presentation plus a single radiographic sign and almost every NEET PG pediatric X-ray collapses to a 30-second answer.
Why pediatric X-ray image MCQs are high-yield for NEET PG
Pediatric and neonatal radiographs are highly stereotyped — one sign per condition is enough to lock the diagnosis. NEET PG and FMGE feature pediatric X-rays in 3-5 questions per paper, often paired with a brief clinical vignette to test the entire reasoning chain (recognise the pattern, name the condition, choose first management).
Mastering these 5 patterns and the 5 NEET PG-favourite signs (ground-glass air bronchograms, patchy infiltrates with hyperinflation, bowel in thorax, thumbprint, steeple) covers approximately 70 percent of the pediatric radiograph questions seen across recent papers.
Foundational concepts before the MCQs
Neonatal respiratory distress — the five questions to ask
For any neonate with respiratory distress, ask:
- Gestational age — preterm (less than 37 weeks) or term/post-term (more than 37 weeks)?
- Onset — at birth, within hours, after 24 hours, or later?
- Maternal factors — meconium-stained liquor, chorioamnionitis, diabetes, PROM, GBS status, antenatal steroids?
- Birth events — type of delivery, APGAR, resuscitation needed, cord gases?
- Examination clues — scaphoid abdomen, absent breath sounds, asymmetric chest, central cyanosis, pre/post-ductal SpO2 differential?
| Condition | Typical gestational age | Onset | Hallmark |
|---|---|---|---|
| Hyaline membrane disease | Preterm <34 wk | Hours after birth | Ground-glass + air bronchograms |
| Transient tachypnea of newborn (TTN) | Term, especially C-section | Within 2 hours | Wet lungs, fluid in fissures |
| Meconium aspiration syndrome | Term/post-term | At birth | Patchy infiltrates, hyperinflation |
| Congenital diaphragmatic hernia | Term | Birth/first hours | Bowel in thorax, mediastinal shift |
| Pneumothorax | Any | Sudden | Lucent hemithorax, lung edge visible |
| Pneumonia / sepsis | Any | Variable | Patchy or lobar infiltrates, may be subtle |
| Congenital heart disease | Any | Variable | Cardiomegaly, pulmonary plethora or oligemia |
Pediatric stridor — upper airway X-ray patterns
| Sign | View | Condition |
|---|---|---|
| Thumbprint | Lateral neck (soft tissue) | Epiglottitis (supraglottic) |
| Steeple | AP neck | Croup (subglottic) |
| Widened prevertebral space | Lateral neck | Retropharyngeal abscess |
| Radio-opaque foreign body | AP and lateral | Foreign body aspiration |
| Air-trapping / unilateral hyperinflation | Inspiratory/expiratory | Foreign body in bronchus (ball-valve effect) |
MCQ 1: 28-week preterm neonate with respiratory distress at 4 hours of life
Image description: [Portable AP chest X-ray of a 1-day-old preterm neonate. There are diffuse, symmetric, fine reticulo-granular opacities (ground-glass appearance) affecting both lungs, with relative sparing of the apices. Multiple air bronchograms are visible extending peripherally — branching tubular lucencies of air-filled bronchi against the opacified lung. Lung volumes appear low (8 posterior ribs visible bilaterally, normally 9-10). The cardiac silhouette is normal. An endotracheal tube is in good position above the carina. An umbilical venous catheter is in place. No pneumothorax. No focal consolidation.]
Clinical vignette: A 28-week female neonate weighing 1,050 g is delivered by emergency LSCS for severe preeclampsia. APGAR 4 at 1 minute and 6 at 5 minutes. Mother received one dose of dexamethasone 12 hours before delivery (incomplete antenatal steroid course). The neonate develops increasing respiratory distress over the first 4 hours of life with grunting, intercostal retractions, nasal flaring, and tachypnea (RR 78). SpO2 is 80 percent on hood oxygen at FiO2 0.4. The neonate is intubated and surfactant is administered. Pre-treatment chest X-ray shows the findings above.
Options:
- (a) Hyaline membrane disease (neonatal respiratory distress syndrome)
- (b) Transient tachypnea of the newborn
- (c) Meconium aspiration syndrome
- (d) Congenital pneumonia
Correct answer: (a) Hyaline membrane disease (neonatal respiratory distress syndrome)
Reasoning: Preterm neonate at 28 weeks, female, incomplete antenatal corticosteroid course, respiratory distress within the first hours of life with grunting, retractions, and the classic CXR pattern of diffuse reticulo-granular ground-glass opacities with air bronchograms and low lung volumes is textbook hyaline membrane disease (neonatal respiratory distress syndrome, RDS) due to surfactant deficiency.
TTN occurs in term or near-term neonates (often after elective C-section), with onset within 2 hours, hyperinflation rather than low volumes, prominent perihilar streaking and fluid in fissures, and rapid resolution over 24-72 hours. MAS occurs in term or post-term neonates with meconium-stained liquor, with patchy coarse infiltrates and hyperinflation. Congenital pneumonia can mimic any pattern but typically has maternal risk factors (chorioamnionitis, PROM, GBS positive), often patchy or lobar consolidation, and laboratory evidence of sepsis.
Teaching pearl: HMD CXR triad = diffuse reticulo-granular (ground-glass) + air bronchograms + low lung volumes. In severe cases: complete "white-out" with obliteration of cardiac and diaphragmatic silhouettes. Surfactant deficiency is the cause; antenatal corticosteroids (at least 24 h of complete course of dexamethasone or betamethasone) reduce incidence and severity.
Risk factors:
- Prematurity (incidence 60-80 percent at less than 28 weeks; falls to 5 percent at 35 weeks)
- Maternal diabetes (delays surfactant maturation)
- Male sex (risk approximately 2x female)
- Second twin
- Asphyxia, cesarean section without labour
- Family history of HMD
Investigations:
- ABG showing respiratory acidosis and hypoxemia
- Lecithin-sphingomyelin (L/S) ratio <2 in amniotic fluid (rarely done now)
- Echocardiogram to exclude congenital heart disease and assess PDA
Management:
- Antenatal corticosteroids if delivery anticipated 24 h to 7 days before 34 weeks gestation (single course; reduces RDS, IVH, NEC)
- Delivery room management: delayed cord clamping 30-60 seconds, gentle ventilation, avoid hyperoxia, target SpO2 88-95 percent
- CPAP from birth for spontaneously breathing preterms (CURPAP, SUPPORT trials) — avoids intubation in many
- Surfactant replacement — natural surfactants (beractant, poractant alfa, calfactant) endotracheally; INSURE technique (Intubate, SURfactant, Extubate to CPAP) reduces ventilator days
- Mechanical ventilation with low tidal volume, optimal PEEP, permissive hypercapnia; volume-targeted modes preferred
- Caffeine for apnea of prematurity (caffeine citrate 20 mg/kg load, 5-10 mg/kg/day maintenance — CAP trial showed neurodevelopmental benefit)
- Antibiotics if sepsis cannot be excluded
- Supportive: thermoregulation, fluids, nutrition, monitoring for complications
Complications:
- Pneumothorax, pulmonary interstitial emphysema (barotrauma)
- Bronchopulmonary dysplasia (BPD) — chronic lung disease at 36 weeks corrected age
- Patent ductus arteriosus (PDA)
- Intraventricular hemorrhage (IVH)
- Retinopathy of prematurity (ROP)
- Necrotising enterocolitis (NEC)
MCQ 2: Term neonate with respiratory distress at birth and meconium-stained liquor
Image description: [Portable AP chest X-ray of a 1-day-old term neonate. There are patchy, coarse, asymmetric bilateral infiltrates with mixed areas of opacification and lucency — classical 'rope-like' or 'snowstorm' pattern. Hyperinflated lung volumes with flattened diaphragms and increased AP diameter. A small right apical pneumothorax is visible with a thin pleural line and absent lung markings beyond it. The cardiac silhouette is normal. An endotracheal tube is in place. No pleural effusion. Some areas of atelectasis adjacent to areas of hyperinflation.]
Clinical vignette: A 40-week male term neonate is delivered vaginally after a difficult labour with non-reassuring fetal heart rate tracing and thick, particulate meconium-stained amniotic fluid. The neonate is depressed at birth (not vigorous — apnea, poor tone, heart rate 90). Tracheal intubation and suctioning is performed before any positive pressure ventilation, recovering thick meconium. APGAR 3 at 1 minute, 6 at 5 minutes, 7 at 10 minutes. Birth weight 3.4 kg. Within 30 minutes the neonate develops worsening respiratory distress with central cyanosis, tachypnea (RR 90), severe retractions, and SpO2 of 78 percent on FiO2 1.0. Pre-ductal (right hand) SpO2 is 84 percent; post-ductal (left foot) SpO2 is 72 percent — pre-post-ductal differential of 12 percent suggesting persistent pulmonary hypertension of the newborn.
Options:
- (a) Hyaline membrane disease
- (b) Meconium aspiration syndrome with persistent pulmonary hypertension of the newborn (PPHN)
- (c) Transient tachypnea of the newborn
- (d) Group B streptococcal pneumonia and sepsis
Correct answer: (b) Meconium aspiration syndrome with persistent pulmonary hypertension of the newborn (PPHN)
Reasoning: Term neonate with thick meconium-stained liquor, depressed/non-vigorous at birth requiring tracheal suctioning, respiratory distress with patchy bilateral infiltrates, hyperinflation, pneumothorax, and a pre-post-ductal SpO2 differential of more than 10 percent is textbook meconium aspiration syndrome (MAS) complicated by persistent pulmonary hypertension of the newborn (PPHN).
HMD occurs in preterm neonates with low lung volumes and ground-glass appearance — opposite to MAS. TTN has perihilar streaking with fluid in fissures, mild distress, rapid resolution. GBS pneumonia in a term neonate is a strong mimic but typically presents with maternal risk factors (GBS positive screen, prolonged ROM, chorioamnionitis), laboratory sepsis markers, and more uniform consolidation rather than the patchy hyperinflated pattern.
Teaching pearl: MAS CXR signature = bilateral patchy coarse asymmetric infiltrates + hyperinflation + frequent pneumothorax/pneumomediastinum. PPHN clue = pre/post-ductal SpO2 differential more than 10 percent, severe hypoxemia disproportionate to lung disease, echocardiogram showing right-to-left shunting through PDA or foramen ovale.
Pathophysiology:
- Meconium passage in utero in response to fetal distress or post-maturity
- Aspiration of meconium-stained amniotic fluid into the airways
- Three mechanisms: (1) mechanical airway obstruction (ball-valve effect → hyperinflation, atelectasis, pneumothorax); (2) chemical pneumonitis with surfactant inactivation; (3) infection / pulmonary hypertension
Delivery room management (2015 NRP onwards):
- Vigorous neonates with meconium-stained liquor: routine intrapartum oropharyngeal suctioning NOT recommended; do NOT perform tracheal suctioning routinely
- Non-vigorous (depressed) neonates: tracheal intubation and suctioning IS recommended ONLY if airway obstruction is suspected; otherwise begin standard NRP with positive pressure ventilation
Management of established MAS:
- Surfactant replacement — useful for severe MAS to overcome surfactant inactivation
- Inhaled nitric oxide (iNO) for PPHN
- High-frequency ventilation for refractory hypoxemia
- ECMO for severe refractory cases
- Supportive: antibiotics empirically (cannot easily distinguish from sepsis), fluid management, thermoregulation, sedation as needed
Complications:
- Pneumothorax (15-20 percent of MAS)
- Pneumomediastinum
- PPHN (30-40 percent of MAS)
- Pulmonary hemorrhage (rare)
- Long-term: reactive airway disease, BPD (in some)
MCQ 3: Term neonate with respiratory distress, scaphoid abdomen, and absent left breath sounds
Image description: [Portable AP chest X-ray of a 1-day-old term neonate. The left hemithorax is occupied by multiple gas-filled bowel loops with a 'honeycomb' appearance, displacing the heart and mediastinum to the right. The left hemidiaphragm is indistinct or absent. The gastric air bubble is NOT seen in the abdomen — it appears to be within the chest. The right lung is compressed and small, pushed to the right by the mediastinal shift. An endotracheal tube is in place. A nasogastric tube descends into the abdomen but appears to deviate into the left thorax. The abdomen below the diaphragm appears gasless and scaphoid.]
Clinical vignette: A 38-week male term neonate is born via vaginal delivery to a 26-year-old primigravida who had no antenatal ultrasounds. Birth weight 3.1 kg. APGAR 5 at 1 minute, 7 at 5 minutes. The neonate develops severe respiratory distress within minutes of birth with marked cyanosis, tachypnea (RR 80), severe retractions, and SpO2 of 65 percent on FiO2 1.0 with bag-mask ventilation. Examination: scaphoid abdomen, absent breath sounds on the left side, bowel sounds heard in the left thorax, heart sounds best heard on the right side of the sternum. The neonate is intubated for severe respiratory failure. CXR shown above.
Options:
- (a) Congenital diaphragmatic hernia (left-sided Bochdalek)
- (b) Tension pneumothorax (left)
- (c) Congenital cystic adenomatoid malformation (CCAM)
- (d) Severe meconium aspiration syndrome
Correct answer: (a) Congenital diaphragmatic hernia (left-sided Bochdalek)
Reasoning: Term neonate with severe respiratory distress at birth, scaphoid abdomen, absent left breath sounds, bowel sounds in the chest, dextrocardia of position, and CXR showing bowel loops in the left hemithorax with mediastinal shift to the right and absent stomach bubble in the abdomen is textbook congenital diaphragmatic hernia (CDH), left-sided Bochdalek type (commonest, 80-90 percent of CDH).
Tension pneumothorax produces a homogeneous lucent hemithorax without bowel loops, often a thin pleural line, and emergency needle decompression is curative — the bowel loops in the chest are diagnostic of CDH. CCAM produces cystic lung lesions but the diaphragm is intact and the stomach bubble is in the abdomen; CCAM is often diagnosed antenatally. Severe MAS produces patchy infiltrates, hyperinflation, and pneumothorax but NOT bowel loops in the chest.
Teaching pearl: CDH triad = scaphoid abdomen + bowel loops in thorax + mediastinal shift to contralateral side. 80-90 percent are left-sided (Bochdalek = posterolateral, more common left); 10-20 percent right-sided; rarely bilateral. Morgagni hernia (anterior) is rare and typically presents later in life.
Pathophysiology:
- Failure of the pleuroperitoneal canal to close at 8-10 weeks gestation
- Abdominal contents (stomach, small bowel, large bowel, spleen, sometimes liver) herniate into the thoracic cavity
- Ipsilateral pulmonary hypoplasia (compressed lung development) — the main determinant of outcome
- Contralateral pulmonary hypoplasia also occurs (mediastinal shift compresses the opposite lung)
- Persistent pulmonary hypertension of the newborn (PPHN) common
Associated anomalies (40 percent of CDH):
- Congenital heart disease (most common)
- Neural tube defects
- Trisomy 18, 21, 13
- Pulmonary sequestration
Antenatal diagnosis:
- Routine antenatal ultrasound (USG abdominal contents in thorax) — most cases diagnosed antenatally in well-screened pregnancies
- Lung-to-head ratio (LHR) on USG and observed/expected LHR predict severity
- Liver position in thorax (intrathoracic liver = worse prognosis)
- Fetal MRI for lung volume assessment
Delivery and immediate management:
- Plan delivery at tertiary centre with ECMO if known antenatally
- NO bag-mask ventilation (avoids further bowel distension in the chest)
- Immediate endotracheal intubation with gentle low-pressure ventilation
- Nasogastric tube to decompress the stomach
- Sedation to prevent crying and air swallowing
- Avoid hyperventilation — hypocapnia constricts cerebral vessels
- Target SpO2 85-95 percent pre-ductal; permissive hypercapnia
Definitive management:
- Stabilise first, operate later — surgery is NOT emergent
- Treatment of PPHN (iNO, sildenafil, milrinone)
- ECMO for refractory cases (severe pulmonary hypoplasia or refractory PPHN)
- Elective surgical repair when haemodynamically stable (typically days 3-7 of life)
- Patch closure (synthetic) if defect is large
Outcome: Overall survival 60-80 percent at experienced centres; depends on degree of pulmonary hypoplasia and PPHN severity.
MCQ 4: 4-year-old with sudden high fever, drooling, tripod posture, and stridor
Image description: [Lateral soft-tissue X-ray of the neck in a 4-year-old child. There is a swollen, rounded soft-tissue density at the level of the larynx — a 'thumbprint' shape occupying the laryngeal vestibule, displacing the airway forward. The aryepiglottic folds appear thickened. The pre-vertebral soft tissue is of normal thickness (not widened). The subglottic airway and trachea appear normal in calibre. No radio-opaque foreign body. The vallecula is partially obliterated.]
Clinical vignette: A 4-year-old boy is brought to the emergency department with rapid-onset high fever (39.8 C) over 6 hours, severe sore throat, muffled 'hot potato' voice, drooling of saliva, refusal to drink, and inspiratory stridor. He is sitting on the bed, leaning forward with his neck extended and chin thrust forward (tripod posture), looking anxious and toxic. He is unvaccinated (parents declined immunisation). No barking cough. No upper respiratory prodrome. He is irritable but alert. Refusing to lie down.
Options:
- (a) Acute epiglottitis (Haemophilus influenzae type B)
- (b) Viral croup (parainfluenza)
- (c) Retropharyngeal abscess
- (d) Foreign body in upper airway
Correct answer: (a) Acute epiglottitis (Haemophilus influenzae type B)
Reasoning: Unvaccinated child with sudden onset high fever, severe sore throat, drooling, muffled voice, inspiratory stridor, tripod posture, refusal to lie down, NO barking cough, and lateral neck X-ray showing a thumb-shaped soft-tissue opacity at the laryngeal vestibule is textbook acute epiglottitis caused by Haemophilus influenzae type B (Hib) — now rare in vaccinated populations but still seen in unvaccinated children and in adults.
Viral croup has barking 'seal-like' cough, gradual onset over 1-2 days with URI prodrome, no drooling, no tripod posture, lower fever, and shows a steeple sign on AP neck X-ray (subglottic narrowing) — not a thumbprint. Retropharyngeal abscess shows widened pre-vertebral soft tissue on lateral neck X-ray (greater than half the AP diameter of the C2 vertebral body). Foreign body usually has a sudden choking history and may show a radio-opaque object or unilateral air-trapping.
Teaching pearl — Epiglottitis vs Croup (NEET PG favourite):
| Feature | Epiglottitis | Croup |
|---|---|---|
| Age | 2-7 years (any age now incl. adults) | 6 months - 3 years |
| Organism | Hib (commonest), strep, staph | Parainfluenza 1, 3 (commonest) |
| Onset | Sudden (hours) | Gradual (1-2 days) with URI prodrome |
| Fever | High (38.5-40 C) | Low to moderate (37.5-38.5 C) |
| Cough | Absent or minimal | Barking 'seal-like' |
| Voice | Muffled ('hot potato') | Hoarse |
| Drooling | Yes (cannot swallow saliva) | No |
| Posture | Tripod, leaning forward | Normal or any |
| Stridor | Severe inspiratory | Inspiratory, often biphasic in severe |
| Toxic appearance | Yes | No (usually well-looking apart from cough) |
| X-ray | Thumbprint sign (lateral) | Steeple sign (AP) |
| Anatomical level | Supraglottic (epiglottis) | Subglottic (cricoid) |
CRITICAL DO NOTs in suspected epiglottitis:
- Do NOT examine the throat with a tongue depressor — laryngospasm and complete airway obstruction may occur
- Do NOT obtain blood tests, IV access, or anything painful before securing the airway — agitation may precipitate obstruction
- Do NOT force the child to lie down — keep upright; the position they assume protects their airway
- Do NOT delay airway control waiting for laboratory or imaging results
Management:
- Urgent airway control in a controlled setting (operating room with anaesthesia and ENT) — fibre-optic intubation; surgical airway (tracheostomy or needle cricothyroidotomy) as backup
- IV ceftriaxone 100 mg/kg/day (or cefotaxime); add vancomycin if MRSA suspected
- IV dexamethasone 0.6 mg/kg
- Oxygen by mask without forcing
- ICU admission after airway secured
- Rifampicin prophylaxis for unvaccinated close household contacts and the index case before discharge (4 days oral)
Prevention: Hib conjugate vaccine — part of UIP pentavalent vaccine (DTwP-HepB-Hib) at 6, 10, 14 weeks.
MCQ 5: 18-month-old with barking cough, hoarse voice, and inspiratory stridor
Image description: [AP soft-tissue X-ray of the neck in an 18-month-old child. There is a tapered narrowing of the subglottic airway with a 'church steeple' or 'pencil-point' appearance — the normal shoulders of the subglottic airway are lost and the airway tapers to a point inferior to the vocal cords. The epiglottis and supraglottic structures appear normal. The pre-vertebral soft tissue is of normal thickness. No radio-opaque foreign body.]
Clinical vignette: An 18-month-old girl is brought to the emergency department in the early hours of the morning with a 2-day history of upper respiratory tract symptoms (rhinorrhea, mild fever 37.8 C, mild cough) which has now progressed overnight to a harsh barking 'seal-like' cough, hoarse voice (cry sounds hoarse), and inspiratory stridor that worsens with crying. She is alert, mildly distressed but interactive, drinking small sips of water, NOT drooling, and is willing to lie down. There is no tripod posture. Her vaccinations are up-to-date. Examination: RR 38, SpO2 96 percent in room air, suprasternal and intercostal retractions, audible inspiratory stridor at rest. Chest auscultation reveals upper airway transmitted sounds; clear lung bases.
Options:
- (a) Viral croup (laryngotracheobronchitis)
- (b) Acute epiglottitis
- (c) Bacterial tracheitis
- (d) Spasmodic croup
Correct answer: (a) Viral croup (laryngotracheobronchitis)
Reasoning: Child aged 6 months to 3 years with URI prodrome, gradual-onset barking 'seal-like' cough, hoarse voice, inspiratory stridor, mild fever, no drooling, no tripod posture, willing to lie down, and AP neck X-ray showing a steeple sign of subglottic narrowing is textbook viral croup (laryngotracheobronchitis) — typically caused by parainfluenza virus types 1 and 3 (also influenza, RSV, adenovirus).
Acute epiglottitis has sudden onset, high fever, drooling, tripod posture, muffled voice, NO barking cough, and shows a thumbprint sign on lateral neck X-ray. Bacterial tracheitis presents with high fever, toxic appearance, copious purulent secretions, and may have an irregular tracheal contour on imaging; treatment is intubation and antibiotics. Spasmodic croup is a recurrent allergic-type laryngeal spasm in older children without significant viral prodrome or fever — clinically resembles croup but is brief and recurs.
Teaching pearl — Croup grading and Westley score:
| Westley Score | Severity | Management |
|---|---|---|
| ≤2 | Mild | Single dose oral dexamethasone, discharge home, supportive |
| 3-5 | Moderate | Nebulised adrenaline + dexamethasone, observe 3-4 hours |
| 6-11 | Severe | Adrenaline + dexamethasone + oxygen; admit; consider PICU |
| ≥12 | Impending respiratory failure | Intubation in controlled setting |
Westley score components: level of consciousness, cyanosis, stridor, air entry, retractions. Each scored 0-5 depending on severity.
Management:
-
Mild croup (no stridor at rest):
- Single dose oral dexamethasone 0.15-0.6 mg/kg (or budesonide nebulisation if vomiting)
- Humidified air (minimal evidence; cool night air anecdotal)
- Supportive care, hydration, antipyretic
- Discharge home with safety-netting advice
-
Moderate-severe croup (stridor at rest, retractions):
- Nebulised adrenaline (1 mg/mL adrenaline, 0.5 mL/kg, max 5 mL) — vasoconstriction reduces mucosal edema; onset within minutes; lasts 1-2 hours; observe 3-4 hours for rebound
- Dexamethasone 0.6 mg/kg PO/IM
- Oxygen if SpO2 less than 92 percent
- Admission for monitoring
-
Impending respiratory failure:
- Intubation with a smaller-than-usual endotracheal tube (subglottic narrowing)
- PICU admission
What does NOT help:
- Antibiotics (viral aetiology; reserve only if bacterial tracheitis suspected)
- Beta-2 agonists (no role unless concomitant wheeze)
- Cool mist tents (minimal evidence)
- Tongue-depressor examination (avoid; minimises risk of laryngospasm)
Differential of inspiratory stridor in a child:
- Viral croup (commonest)
- Spasmodic croup (recurrent, allergic-type)
- Acute epiglottitis (now rare; toxic, tripod, drooling)
- Bacterial tracheitis (severe; toxic; purulent secretions)
- Foreign body aspiration (sudden onset; choking history)
- Retropharyngeal abscess (neck stiffness, fever, drooling)
- Peritonsillar abscess (older child; trismus, uvular deviation)
- Anaphylaxis (urticaria, hypotension, exposure history)
- Laryngomalacia (infants, positional, benign)
- Vocal cord paralysis (post-cardiac surgery; persistent)
- Subglottic stenosis (post-intubation; persistent)
Common pitfalls and how to avoid them
Pitfall 1: Confusing HMD and TTN. Both occur in neonates with respiratory distress, but HMD is in preterm with low lung volumes and ground-glass + air bronchograms, while TTN is in term/near-term (especially after C-section) with hyperinflation, prominent perihilar streaking, and fluid in fissures. TTN resolves within 24-72 hours; HMD evolves over days.
Pitfall 2: Missing PPHN in severe MAS or CDH. Any term neonate with severe hypoxemia disproportionate to lung disease — check pre-post-ductal SpO2 differential. Greater than 10 percent difference (pre-ductal higher) suggests right-to-left shunting and PPHN. Echocardiogram confirms.
Pitfall 3: Bag-mask ventilation in suspected CDH. Worsens distension of intrathoracic bowel and compresses the lung further. Always intubate immediately and place an NG tube; never give bag-mask ventilation if CDH is suspected antenatally or by examination (scaphoid abdomen, dextrocardia, bowel sounds in chest).
Pitfall 4: Examining the throat with a tongue depressor in epiglottitis. May precipitate laryngospasm and complete airway obstruction. If epiglottitis is suspected (tripod, drooling, toxic), DO NOT examine. Get the child to a controlled airway setting first.
Pitfall 5: Treating epiglottitis with steam or nebulised adrenaline. Croup responds to adrenaline; epiglottitis does NOT — epiglottitis needs definitive airway control and IV antibiotics.
Pitfall 6: Lateral vs AP neck X-ray confusion. Thumbprint sign is on LATERAL view (epiglottitis). Steeple sign is on AP view (croup). Read the projection carefully on the imaging legend.
Pitfall 7: Calling every subglottic narrowing 'croup'. Anaphylaxis, bacterial tracheitis, and foreign body can mimic. Look for the right clinical context — barking cough + URI prodrome + 6 months to 3 years is croup; choking history is foreign body; high fever and toxic appearance is bacterial tracheitis.
How NEET PG tests pediatric X-ray patterns
Six recurring patterns. Recognise the pattern and the question collapses.
Pattern 1 — The HMD question: Preterm neonate, surfactant deficiency, ground-glass + air bronchograms, low lung volumes, after incomplete antenatal steroids. Diagnosis? Hyaline membrane disease. Best management? CPAP / surfactant replacement; antenatal corticosteroids in subsequent pregnancies.
Pattern 2 — The MAS question: Term/post-term, meconium-stained liquor, patchy infiltrates, hyperinflation, pneumothorax, pre-post-ductal SpO2 differential. Diagnosis? MAS with PPHN. Best management? Surfactant + iNO + supportive ventilation; ECMO for refractory.
Pattern 3 — The CDH question: Severe distress at birth, scaphoid abdomen, dextrocardia of position, bowel in thorax. Diagnosis? Congenital diaphragmatic hernia (left Bochdalek 80-90 percent). Best management? Immediate intubation (NO bag-mask), NG tube, stabilise first, surgery delayed (NOT emergent), iNO/ECMO for PPHN.
Pattern 4 — The epiglottitis question: Sudden onset, high fever, drooling, tripod, muffled voice, no cough, thumbprint sign. Diagnosis? Acute epiglottitis (Hib). Best management? Urgent airway in OR + ceftriaxone + dexamethasone; do NOT examine the throat.
Pattern 5 — The croup question: Gradual onset, barking cough, hoarse voice, inspiratory stridor, mild fever, steeple sign. Diagnosis? Viral croup (parainfluenza). Best management? Dexamethasone for all; nebulised adrenaline for moderate-severe.
Pattern 6 — The 'pre-post-ductal SpO2 differential' question: Tests recognition of right-to-left shunting through the patent ductus arteriosus. Pre-ductal (right hand) higher than post-ductal (lower limbs) by more than 10 percent suggests PPHN or right-to-left shunt at the ductal level (e.g., coarctation, interrupted aortic arch).
High-yield one-liners:
- HMD CXR: diffuse ground-glass + air bronchograms + low lung volumes; preterm; surfactant deficiency
- MAS CXR: patchy coarse infiltrates + hyperinflation + frequent pneumothorax; term/post-term
- CDH CXR: bowel loops in thorax + mediastinal shift + absent stomach bubble in abdomen + scaphoid abdomen
- Epiglottitis: thumbprint sign on LATERAL neck X-ray + tripod + drooling + muffled voice
- Croup: steeple sign on AP neck X-ray + barking cough + hoarse voice + inspiratory stridor
- HMD age: preterm under 34 weeks; MAS: term/post-term; CDH: term; epiglottitis: 2-7 years; croup: 6 months to 3 years
- PPHN clue: pre-post-ductal SpO2 differential more than 10 percent
- Antenatal corticosteroids reduce HMD; Hib vaccine reduces epiglottitis
- Croup management: dexamethasone for all + nebulised adrenaline for moderate-severe
- Epiglottitis: NO throat exam, urgent airway control, IV ceftriaxone
Frequently Asked Questions
How do you differentiate hyaline membrane disease from meconium aspiration syndrome on chest X-ray?
Hyaline membrane disease (HMD, neonatal RDS) classically affects preterm neonates under 34 weeks who have surfactant deficiency. CXR shows a diffuse reticulo-granular ground-glass pattern, air bronchograms, low lung volumes, and a 'white-out' in severe cases. Meconium aspiration syndrome (MAS) affects term or post-term neonates with peripartum meconium-stained liquor and respiratory distress at birth. CXR shows patchy bilateral coarse asymmetric infiltrates with hyperinflation (flattened diaphragm, increased AP diameter), areas of atelectasis adjacent to areas of hyperinflation, and a high incidence of pneumothorax and pneumomediastinum. The clue pair is gestational age (preterm for HMD, term/post-term for MAS) and lung volume (low in HMD, high in MAS). HMD responds to surfactant replacement and CPAP; MAS responds to tracheal suctioning of non-vigorous infants, surfactant, inhaled nitric oxide for persistent pulmonary hypertension, and ECMO in severe cases.
What are the radiographic features of congenital diaphragmatic hernia in a newborn?
Congenital diaphragmatic hernia (CDH) classically presents within hours of birth with respiratory distress, scaphoid abdomen, and absent breath sounds on the affected side (typically left in 80-90 percent). CXR shows multiple gas-filled bowel loops within the thoracic cavity, mediastinal shift to the contralateral side (rightward in left-sided CDH), absence of a normal stomach bubble in the abdomen, contralateral compressed lung, and an indistinct or absent hemidiaphragm on the affected side. The differential is congenital cystic adenomatoid malformation (CCAM) — cystic-appearing lung lesions but with an intact diaphragm and stomach bubble in the abdomen. CDH is associated with pulmonary hypoplasia (both ipsilateral and contralateral) and persistent pulmonary hypertension of the newborn (PPHN). Management is gentle ventilation, sedation, avoidance of hyperventilation, treatment of PPHN with inhaled nitric oxide, ECMO in severe cases, and elective surgical repair when haemodynamically stable — surgery does NOT need to be emergent.
What is the thumbprint sign on a lateral neck X-ray and what is its differential?
The thumbprint sign is a soft-tissue swelling of the epiglottis on a lateral neck X-ray that resembles a thumb-shaped opacity above the larynx. It is the radiographic hallmark of acute epiglottitis (supraglottitis) typically caused by Haemophilus influenzae type B (Hib) in unvaccinated children aged 2-7 years (now rare after Hib vaccination) and increasingly seen in adults and in immunocompromised hosts. Clinical features: high fever, tripod posture (sitting forward with chin extended), drooling, dysphagia, muffled voice ('hot potato voice'), inspiratory stridor, severe sore throat without prominent cough. CRITICAL: do NOT examine the throat with a tongue depressor — laryngospasm and airway obstruction can occur. Management is urgent airway control by anaesthetics and ENT in a controlled setting (operating room ideally), IV ceftriaxone, IV dexamethasone, and oxygen. Differential of thumbprint sign: epiglottitis (commonest), severe pharyngitis with epiglottic swelling, retropharyngeal abscess (which usually shows widened pre-vertebral space, not specifically the thumb sign).
What is the steeple sign and how does croup differ from epiglottitis on imaging and clinical features?
The steeple sign (or pencil-point sign) is a tapered subglottic narrowing seen on an AP soft-tissue neck X-ray, resembling a church steeple. It is the radiographic hallmark of viral croup (laryngotracheobronchitis), typically caused by parainfluenza virus types 1 and 3 in children aged 6 months to 3 years. Croup presents with barking 'seal-like' cough, inspiratory stridor, hoarse voice, low-to-moderate fever, and prodromal upper respiratory symptoms. Croup is gradual onset over 1-2 days. Epiglottitis is sudden onset over hours with high fever, drooling, dysphagia, tripod posture, and muffled voice WITHOUT a barking cough. Imaging differentiation: steeple sign (croup, AP view, subglottic) vs thumbprint sign (epiglottitis, lateral view, supraglottic). Management of croup: nebulised adrenaline for moderate-severe, single-dose oral or IM dexamethasone 0.15-0.6 mg/kg, humidified oxygen, supportive care. Most croup is self-limiting; admission is needed for stridor at rest, severe retractions, or failure to respond to treatment.
What is persistent pulmonary hypertension of the newborn (PPHN) and how is it managed?
Persistent pulmonary hypertension of the newborn (PPHN) is the failure of the normal postnatal drop in pulmonary vascular resistance, leading to right-to-left shunting through the foramen ovale and ductus arteriosus with severe hypoxemia. PPHN complicates meconium aspiration syndrome, congenital diaphragmatic hernia, sepsis, pneumonia, congenital heart disease, and idiopathic cases. Clinical features: cyanosis disproportionate to respiratory distress, pre-ductal vs post-ductal SpO2 difference of more than 10 percent (pre-ductal right arm higher than post-ductal lower limbs), echocardiogram showing right-to-left or bidirectional shunting through the ductus arteriosus or foramen ovale and elevated pulmonary artery pressure. Management: optimise ventilation (avoid hyperventilation which worsens cerebral blood flow), maintain oxygenation, inhaled nitric oxide as first-line pulmonary vasodilator, sildenafil and milrinone as adjuncts, surfactant if surfactant-related cause, treat underlying cause (antibiotics, suction), and ECMO for refractory cases. Avoid alkalosis-induced hyperventilation; use targeted SpO2 (90-95 percent pre-ductal).
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Written by: NEETPGAI Editorial Team Reviewed by: Pending SME Review Last reviewed: May 2026
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Ready to put this into practice?
Start practicing NEET PG MCQs with AI-powered explanations.
Start Free PracticeYour Next Step
Related Study Guides
Anxiety Disorders, OCD & PTSD for NEET PG 2026: Diagnosis, SSRI, CBT
Master anxiety, OCD, and PTSD for NEET PG 2026 — DSM-5 criteria, Y-BOCS, SSRI first-line, exposure-response prevention, ECT indications, India NMHS data.
Cardiovascular Physiology and Cardiac Cycle for NEET PG 2026
Master cardiac cycle, Wiggers diagram, ECG basis, heart sounds, preload-afterload, Starling's law, JVP waves, and CO measurement for NEET PG 2026 — high-yield MCQ traps.
Acute Appendicitis Management for NEET PG 2026: Diagnosis & Surgery
Master acute appendicitis for NEET PG 2026 — pathophysiology, Alvarado score, imaging, laparoscopic appendicectomy, antibiotic-only therapy, complications, MCQ traps.
Join our NEET PG community
Daily MCQs, study tips, and topper strategies on Telegram.
Join on Telegram →