14 Common Mistakes in Orthopedics for NEET PG — And How to Avoid Them
Avoid the costliest orthopedic mistakes in NEET PG 2026: Colles vs Smith, Salter-Harris, fracture healing, dislocations, RA vs OA, septic arthritis, compartment syndrome, AVN, DDH, Gustilo.
Version 1.0 — Published May 2026
Quick Answer
Orthopedics contributes 8-12 questions in NEET PG, often coupled with radiology and rheumatology. The 14 most expensive mistakes cluster around fracture eponyms, paediatric growth plate injuries, joint pathology, and orthopedic emergencies. To protect your marks:
- Do not confuse Colles vs Smith fracture — dorsal vs volar displacement matters
- Master Salter-Harris classification I-V — the SALTR mnemonic and the Thurston-Holland fragment
- Sequence fracture healing stages correctly — hematoma → inflammation → soft callus → hard callus → remodeling
- Distinguish dislocation from subluxation — complete vs partial loss of joint congruity
- Differentiate RA from OA on joint distribution, morning stiffness, and X-ray — PIP/MCP vs DIP/CMC
- Recognise septic arthritis early — fever, joint tenderness, raised WBC/CRP, immediate joint aspiration
- Diagnose compartment syndrome on PAIN, not pulses — fasciotomy within 6 hours
- Apply the fat embolism syndrome triad — hypoxia, neurological signs, petechial rash
- Identify paediatric fracture patterns — greenstick, torus/buckle, plastic deformation
- Differentiate spondylolisthesis, spondylolysis, spondylosis — slip vs pars defect vs OA spine
- Perform Ortolani and Barlow correctly — relocation vs provocation
- Recognise AVN sites — scaphoid (proximal pole), femoral head, talus body
- Classify open fractures by Gustilo-Anderson I-IIIC — guides antibiotic and surgical plan
- Apply the rule of 3 to fracture management — reduction, retention, rehabilitation
Why orthopedic mistakes are costly
Orthopedics sits at the intersection of surgery, radiology, paediatrics, and rheumatology. A single misclassified Salter-Harris or missed compartment syndrome on an MCQ can cost 1-2 marks; in practice, missing the diagnosis means lifelong disability or limb loss. NEET PG and INI-CET examiners use orthopedic vignettes to test pattern recognition (eponyms, classifications), emergencies (compartment syndrome, fat embolism, open fractures), and high-yield trivia (AVN sites, Gustilo classification).
The 14 mistakes below come from analysis of NEET PG 2019-2024 orthopedics questions and represent the most frequent error patterns. Pair this guide with the bone X-ray pathology image MCQ for deeper imaging coverage.
Mistake 1: Confusing Colles and Smith fractures
What students do: Memorise both as "distal radius fracture" without locking in the displacement direction.
Why it is wrong: NEET PG specifically asks about displacement direction and deformity name. Calling a volar-displaced fracture "Colles" is a one-mark loss.
Correct approach:
| Feature | Colles | Smith (reverse Colles) |
|---|---|---|
| Displacement | DORSAL (posterior) | VOLAR (anterior) |
| Angulation | Dorsal | Volar |
| Deformity | Dinner-fork on lateral view | Garden-spade on lateral view |
| Mechanism | FOOSH with wrist extended | Fall on flexed wrist; backward fall with hand behind |
| Frequency | Common — elderly osteoporotic women | Less common |
| Associated | Ulnar styloid fracture (60 percent), median nerve injury | Median nerve injury |
| Management | Closed reduction + below-elbow cast in slight palmar flexion and ulnar deviation; ORIF if unstable/intra-articular | Closed reduction + cast in dorsiflexion; ORIF often required (Smith is more unstable) |
Other distal radius eponyms:
- Barton fracture — intra-articular distal radius fracture (volar Barton or dorsal Barton)
- Chauffeur fracture — radial styloid fracture
- Galeazzi fracture — distal third radius fracture + distal radio-ulnar joint (DRUJ) dislocation
- Monteggia fracture — proximal ulna fracture + radial head dislocation (mnemonic GRUM — Galeazzi Radius Ulna Monteggia, or MUGR — Monteggia Ulna Galeazzi Radius)
How to remember: Colles = Dorsal (both end in -s); Smith = Volar (Smith has a "V" sound). Or visually: Colles produces a dinner-fork (dorsal hump), Smith produces a garden-spade (volar bulge).
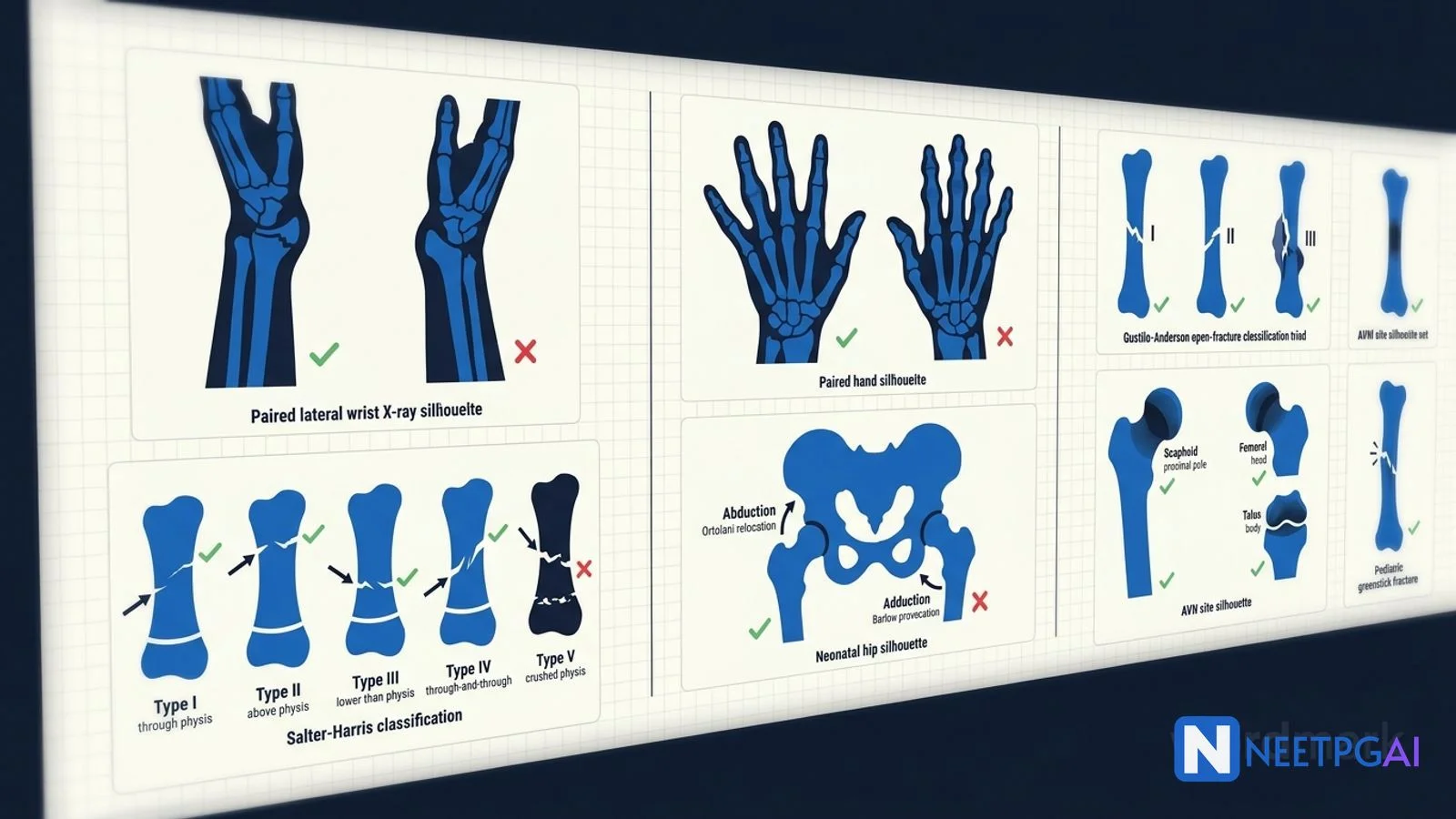
Mistake 2: Mislabeling Salter-Harris types I-V
What students do: Remember only Type II (the commonest) and confuse the others.
Why it is wrong: Each Salter-Harris type has different prognosis and management. Calling a Type III "Type II" misses the intra-articular nature and the need for anatomical reduction.
Correct approach — SALTR mnemonic:
| Type | Mnemonic | Description | Prognosis | NEET PG pearl |
|---|---|---|---|---|
| I | S — Slipped/Straight | Pure transverse fracture through physis | Good | Young children; may need wide physeal X-ray view |
| II | A — Above | Through physis extending UP into metaphysis | Good | MOST COMMON (75 percent); Thurston-Holland fragment in metaphysis |
| III | L — Lower | Through physis extending DOWN into epiphysis | Moderate (intra-articular) | Requires anatomical reduction; risk of growth arrest |
| IV | T — Through/Together | Through metaphysis AND epiphysis, crossing physis | Worse | Requires anatomical reduction (often ORIF); high growth arrest risk |
| V | R — Rammed/Ruined | Crush injury to physis | Worst | Often missed initially; growth arrest, limb shortening, angular deformity |
How to remember: SALTR, with the action progressing from PURE physis (I) → up into metaphysis (II) → down into epiphysis (III) → through both (IV) → ruined/crushed (V).
Key principle: Anatomical reduction is essential for Types III and IV (intra-articular); growth-arrest follow-up is essential for Types III, IV, and V. Always document neurovascular status and document the type clearly on imaging reports.
Mistake 3: Forgetting the stages of fracture healing
What students do: Mix up the order or compress 5 stages into "callus formation".
Why it is wrong: NEET PG asks "at what stage is callus visible on X-ray" — soft callus at 2-3 weeks, hard callus at 6-12 weeks. Getting the sequence wrong costs the question.
Correct sequence — 5 stages:
| Stage | Timing | Key event |
|---|---|---|
| 1. Hematoma formation | 0-72 hours | Bleeding from disrupted vessels forms a fibrin-rich clot at fracture site |
| 2. Inflammation | 1-7 days | Macrophages and inflammatory cells clear debris; release of cytokines (TNF, IL-1, IL-6, BMP) recruits stem cells |
| 3. Soft callus (fibrocartilaginous) | 2-3 weeks | Mesenchymal stem cells differentiate into chondroblasts and fibroblasts; cartilage and fibrous tissue bridge the gap; visible on X-ray |
| 4. Hard callus (bony) | 6-12 weeks | Endochondral ossification converts cartilage to woven bone; visible callus on X-ray with bridging |
| 5. Remodeling | Months to years | Woven bone is replaced by lamellar bone; restoration of medullary cavity; Wolff's law — bone remodels along lines of stress |
Two types of bone healing:
- Secondary (indirect) healing — through callus formation; the standard sequence above; in fractures treated with conservative casting or intramedullary nailing
- Primary (direct) healing — Haversian remodelling without visible callus; requires rigid anatomical reduction and absolute stability (compression plating); seen with ORIF
How to remember: "Hematoma → Inflammation → Soft callus → Hard callus → Remodeling" — mnemonic "HISHR" or simply visualise the timeline (days → weeks → months → years).
Mistake 4: Confusing dislocation, subluxation, and diastasis
What students do: Use these terms interchangeably.
Why it is wrong: Each has a specific meaning and different management. NEET PG tests vocabulary directly.
Correct definitions:
- Dislocation (luxation) — COMPLETE loss of joint congruity; articular surfaces of the two bones no longer in contact at all
- Subluxation — PARTIAL loss of joint congruity; articular surfaces still partially in contact but malaligned
- Diastasis — separation of two normally adjacent bones at a joint where there is usually no significant motion (e.g., tibiofibular diastasis at the syndesmosis, pubic symphysis diastasis after trauma or childbirth)
- Fracture-dislocation — joint dislocation associated with a fracture of one of the articulating bones
Common dislocations:
- Shoulder (glenohumeral) — most commonly dislocated large joint; 95 percent are anterior dislocations (FOOSH with arm abducted and externally rotated); look for Hill-Sachs lesion (humeral head) and Bankart lesion (anteroinferior labrum) on MRI
- Hip — posterior dislocation is commonest (dashboard injury — knee flexed, hip flexed, force along femur); risk of sciatic nerve injury and AVN; emergency reduction within 6 hours
- Elbow — posterior dislocation; FOOSH with elbow extended; check for radial head and coronoid fractures (terrible triad)
- Patella — usually lateral; medial patellofemoral ligament (MPFL) tear; classic in young female with valgus knee
- Knee (tibiofemoral) — high-energy trauma; check for popliteal artery injury (urgent angiography) and common peroneal nerve injury — limb-threatening
Mistake 5: Failing to differentiate RA from OA on a vignette
What students do: Memorise RA vs OA in isolation without integrating distribution, morning stiffness, and X-ray findings.
Why it is wrong: NEET PG vignettes often give partial features; only the integrated pattern recognition gets the answer.
Correct approach:
| Feature | Rheumatoid arthritis (RA) | Osteoarthritis (OA) |
|---|---|---|
| Joints involved | MCP, PIP, wrist (symmetric small joints first) | DIP, CMC of thumb, knee, hip, spine (large weight-bearing joints) |
| Distribution | Symmetric, polyarticular | Asymmetric, oligoarticular |
| Morning stiffness | Over 1 hour, worsens with rest, improves with use | Under 30 min, worsens with use, improves with rest |
| Systemic features | Fatigue, weight loss, fever, extra-articular (nodules, vasculitis, pleuritis, episcleritis) | None |
| Lab findings | Raised ESR/CRP, RF positive (70-80 percent), anti-CCP positive (more specific) | Normal labs |
| X-ray findings | Periarticular osteopenia, joint space narrowing (uniform), marginal erosions, ulnar deviation, swan-neck/boutonnière deformities | Joint space narrowing (asymmetric/non-uniform), osteophytes, subchondral sclerosis, subchondral cysts, Heberden (DIP) and Bouchard (PIP) nodes |
| Synovial fluid | Inflammatory (WBC 5,000-50,000, mostly neutrophils early then mixed) | Non-inflammatory (WBC under 2,000, mostly mononuclear) |
| Treatment | DMARDs (methotrexate first-line), biologics (anti-TNF, anti-IL-6, JAK inhibitors), steroids for flares | Analgesics, NSAIDs, physiotherapy, intra-articular steroids, joint replacement |
How to remember:
- RA: morning stiffness over 1 hour, MCP/PIP, symmetric, systemic, raised inflammatory markers, RF/anti-CCP positive, erosions on X-ray
- OA: morning stiffness under 30 min, DIP/weight-bearing joints, asymmetric, no systemic features, normal labs, osteophytes on X-ray
The classic exam trap: a vignette with DIP involvement and Heberden's nodes is OA, NOT RA. RA typically SPARES the DIP joints.
Mistake 6: Missing septic arthritis vs reactive arthritis
What students do: Both have fever and joint pain — call both "septic".
Why it is wrong: Septic arthritis is a surgical emergency requiring joint aspiration and antibiotics within 24 hours. Missing it destroys the joint.
Correct approach:
| Feature | Septic arthritis | Reactive arthritis |
|---|---|---|
| Pathophysiology | Direct infection of joint (haematogenous, contiguous, or iatrogenic) | Sterile inflammation triggered by extra-articular infection (post-Chlamydia, post-Salmonella/Shigella/Yersinia gastroenteritis) |
| Onset | Acute (hours to days), hot/red/swollen single joint | Days to weeks after triggering infection |
| Joint distribution | Monoarticular usually; knee most common in adults, hip in children | Asymmetric oligoarthritis (knees, ankles, sacroiliac); enthesitis |
| Fever | Often high | Mild or absent |
| Synovial fluid WBC | Over 50,000 (often over 100,000), mostly neutrophils, low glucose, positive Gram stain/culture in 50-70 percent | 2,000-50,000, sterile culture |
| Causative organism | Adults: S. aureus (commonest), Streptococcus, Gonococcus (young sexually active); Children: S. aureus, Kingella kingae (under 4 yr); IVDU/elderly: Gram-negatives | None in joint; trigger organisms identified by stool culture, urine PCR, urethral swab |
| Associated features | None typically | Conjunctivitis, urethritis (Reiter triad), keratoderma blennorrhagicum, circinate balanitis, HLA-B27 positive |
| Treatment | Emergency joint aspiration + IV antibiotics (empirical: ceftriaxone + vancomycin, adjust to culture; duration 2-4 weeks IV then oral) + arthroscopic/open washout | NSAIDs, intra-articular steroids; treat triggering infection with antibiotics; biologics for chronic disease |
Key principle: ANY child or adult with monoarticular hot joint + fever must have urgent joint aspiration to rule out septic arthritis. Kocher criteria for paediatric septic hip: fever over 38.5 C, non-weight-bearing, ESR over 40, WBC over 12,000 — 3-4 criteria predict over 90 percent risk of septic arthritis.
Mistake 7: Diagnosing compartment syndrome on pulselessness instead of pain
What students do: Wait for the classic 5 P's including pulselessness to make the diagnosis.
Why it is wrong: Pulses are typically PRESENT in early compartment syndrome (compartment pressure rarely exceeds systolic BP). Waiting for pulselessness means muscle and nerve are already irreversibly damaged. Pain out of proportion is the earliest sign.
Correct approach — 5 P's, in order of appearance:
- Pain — out of proportion to injury, worsened by passive stretch of involved muscles (the most sensitive early sign)
- Paraesthesia — early sign of nerve compression
- Pallor — later
- Paralysis — late
- Pulselessness — VERY late (means severe ischaemia already)
A 6th P (Poikilothermia/cold) is sometimes added.
Diagnostic threshold:
- Absolute compartment pressure over 30 mmHg measured with a Stryker needle
- OR delta pressure (diastolic BP minus compartment pressure) under 30 mmHg — more reliable in hypotensive patients
Treatment: emergency fasciotomy within 6 hours. Delayed fasciotomy causes irreversible muscle necrosis, contracture (Volkmann ischaemic contracture in forearm; clawing of fingers/toes), and rhabdomyolysis with AKI. After fasciotomy, leave wound open and close after 5-7 days when swelling subsides.
Commonest sites:
- Leg — anterior compartment (commonest in tibial fractures; deep peroneal nerve affected, foot drop)
- Forearm — Volkmann ischaemic contracture after supracondylar humerus fracture
- Hand, foot, thigh, buttock — less common
Risk factors: tibial shaft fracture (most common), supracondylar humerus fracture, crush injury, prolonged compression, tight cast/dressing, severe burns, snakebite, IV extravasation, reperfusion after vascular surgery.
Mistake 8: Missing the fat embolism syndrome triad
What students do: Attribute hypoxia and confusion in a polytrauma patient to PE or sepsis.
Why it is wrong: Fat embolism syndrome (FES) has a specific triad and a specific window (24-72 hours after long-bone fracture). Treatment is supportive and prevention is fracture stabilisation.
Correct approach — Gurd's criteria for FES:
Major criteria:
- Respiratory insufficiency (hypoxia, tachypnoea, ARDS pattern, bilateral pulmonary infiltrates)
- Cerebral involvement (altered mental status, confusion, drowsiness, seizures — not explained by head injury)
- Petechial rash (axilla, conjunctiva, oral mucosa — classically appears 24-72 hours after fracture)
Minor criteria: tachycardia, fever, retinal changes (Purtscher retinopathy — cotton-wool spots), jaundice, renal changes, thrombocytopenia, anaemia, raised ESR, fat globules in sputum/urine.
Diagnosis: ≥1 major + ≥4 minor criteria, or 2 major criteria.
Timing: 24-72 hours after long-bone fracture (commonly femur), polytrauma, or pelvic surgery.
Pathophysiology:
- Mechanical theory: fat globules from marrow enter venous circulation, embolise to lung and brain
- Biochemical theory: free fatty acids release from stored triglycerides cause inflammatory injury
Treatment:
- Supportive — oxygen, mechanical ventilation if ARDS develops, fluid resuscitation, ICU care
- Early fracture stabilisation (within 24 hours) reduces FES risk
- NO role for steroids or heparin routinely (though steroids studied as prophylaxis in high-risk fractures)
Mortality: 5-15 percent if recognised; higher if missed.
Mistake 9: Missing the spectrum of paediatric fractures
What students do: Apply adult fracture morphology to paediatric vignettes.
Why it is wrong: Paediatric bones are more elastic, periosteum is thicker, and growth plate adds vulnerability. Distinct fracture patterns occur.
Correct paediatric fracture types:
- Greenstick fracture — incomplete fracture; cortex broken on convex (tension) side, intact on concave (compression) side; common in forearm; needs angulation correction and casting
- Torus (buckle) fracture — compression fracture; cortex buckled or wrinkled, no clear cortex break; commonest paediatric forearm fracture (FOOSH); typically heals in 3-4 weeks with simple immobilisation
- Plastic deformation (bowing) — bone bows without a discrete fracture line; common in ulna and fibula; may need closed reduction if angulation severe
- Complete fracture — both cortices fractured; transverse, oblique, spiral patterns
- Salter-Harris fractures — through the growth plate (covered in Mistake 2)
- Supracondylar humerus fracture — common 5-7 yr; Gartland classification I-IV; risk of brachial artery and median nerve injury (anterior interosseous branch); high risk of cubitus varus deformity ("gunstock") if not anatomically reduced
- Toddler fracture — undisplaced spiral fracture of distal tibia in 1-3 yr olds; often very subtle X-ray; weight-bearing pain; long-leg cast 4 weeks
Key principle: Paediatric remodelling is excellent — even moderate angulation in young children remodels over time (especially in the plane of joint motion). But rotational deformity does NOT remodel — must be corrected.
Mistake 10: Confusing spondylolisthesis, spondylolysis, and spondylosis
What students do: Treat these as variants of the same word.
Why it is wrong: They are completely different entities. NEET PG examiners use the names interchangeably to trap.
Correct definitions:
- Spondylolysis — defect in the pars interarticularis (between superior and inferior articular processes); a stress fracture in adolescent athletes (gymnasts, fast bowlers, weightlifters); seen as "Scotty dog with collar" sign on oblique lumbar X-ray; commonest at L5; treatment usually non-operative (rest, brace)
- Spondylolisthesis — forward (anterior) slip of one vertebra on another; often secondary to bilateral spondylolysis (isthmic spondylolisthesis) or to degenerative changes (degenerative spondylolisthesis); commonest at L5-S1; Meyerding grading I-V based on degree of slip (under 25 percent, 25-50, 50-75, 75-100, complete); treatment depends on grade and symptoms — non-operative for low grade, fusion for high grade or refractory symptoms
- Spondylosis — degenerative arthritis of the spine; osteophytes, disc space narrowing, facet joint OA; affects cervical and lumbar spine commonly; presents with axial pain and may have radiculopathy or myelopathy
Mnemonic: Lysis = lesion (pars defect); Listhesis = lateral/forward slip; Sis (osis) = arthritis.
Mistake 11: Botching Ortolani and Barlow in neonatal hip examination
What students do: Confuse which test is for relocation vs provocation.
Why it is wrong: NEET PG examiners directly test the direction of force and the meaning of a positive sign.
Correct approach:
| Test | Action | Positive sign meaning |
|---|---|---|
| Ortolani (relocation) | Hip ABDUCTED, greater trochanter LIFTED ANTERIORLY | Palpable CLUNK as dislocated hip relocates → dislocated but reducible |
| Barlow (provocation) | Hip ADDUCTED, knee pushed POSTERIORLY | Palpable clunk as hip dislocates posteriorly → dislocatable (unstable) |
Important: A "click" (high-pitched, soft tissue) is NOT pathological — a "clunk" (low-pitched, mechanical, palpable) is. Distinguishing click from clunk takes practice.
Limitations: Both tests become less reliable after 3 months as soft-tissue contractures develop. After 3 months, look for:
- Limited hip abduction (under 60 degrees, especially asymmetric)
- Galeazzi sign — apparent femoral shortening on one side when knees flexed in supine
- Asymmetric thigh creases
- Trendelenburg sign / waddling gait in older children once walking
Imaging:
- Ultrasound is the investigation of choice from birth to 6 months (Graf alpha angle measures bony coverage; Harcke dynamic technique assesses stability)
- X-ray pelvis AP is used after 6 months when the femoral head ossifies; measure Acetabular index, Shenton's line, Hilgenreiner's line, Perkin's quadrant
Risk factors for DDH: Female sex (4-6x), breech presentation, family history, firstborn, oligohydramnios, swaddling with hips extended, postural deformity.
Treatment:
- Birth to 6 months: Pavlik harness (keeps hip flexed and abducted) — success rate over 90 percent
- 6 to 18 months: closed reduction under anaesthesia + hip spica cast
- Over 18 months: open reduction + femoral or pelvic osteotomy (Salter, Pemberton)
- Late-presenting (over 2-3 years): more extensive reconstructive surgery
Mistake 12: Missing classic AVN sites
What students do: Forget which bones are at high risk of avascular necrosis after fracture.
Why it is wrong: AVN is a delayed complication with specific anatomical predispositions. NEET PG asks "which fracture has highest risk of AVN" — the answer depends on knowing the blood supply.
Correct list — AVN-prone sites and why:
- Scaphoid (proximal pole) — blood supply enters distally and runs proximally; fracture interrupts blood supply to proximal pole; 30 percent AVN in proximal-third fractures; X-ray initially normal — repeat at 10-14 days or MRI for early diagnosis
- Femoral head — blood supply via medial circumflex femoral artery, retinacular vessels; subcapital and intracapsular femoral neck fractures in elderly have high AVN risk (15-30 percent); hemiarthroplasty/total hip replacement preferred over fixation in displaced intracapsular fractures in elderly
- Talus body — blood supply enters distally; talar neck fractures (Hawkins classification I-IV) have rising AVN risk with displacement and dislocation (Hawkins I — 0-10 percent, II — 20-50, III — over 80, IV — almost 100 percent)
- Lunate (Kienböck disease) — idiopathic AVN of the lunate; associated with ulnar minus variant
- Capitellum (Panner disease in children, osteochondritis dissecans in adolescents)
- Hip (Perthes disease in children) — idiopathic AVN of femoral head age 4-8 years
- Tarsal navicular (Köhler disease in children, Müller-Weiss in adults)
- Metatarsal head (Freiberg disease) — second metatarsal head, adolescent girls
Risk factors for non-traumatic AVN: Steroid use (long-term), alcohol, sickle cell disease, lupus, antiphospholipid syndrome, Gaucher disease, decompression sickness (dysbaric osteonecrosis), pregnancy, idiopathic.
Imaging: MRI is the gold standard — shows marrow edema and the characteristic "double-line sign" or "crescent sign" early, before X-ray changes appear.
Ficat-Arlet staging of femoral head AVN:
- I: Normal X-ray, abnormal MRI
- II: Sclerosis or cyst on X-ray
- III: Subchondral collapse (crescent sign)
- IV: Femoral head flattening, OA
Treatment: Core decompression for early stages; bone grafting; osteotomy; hip replacement for advanced disease.
Mistake 13: Misclassifying open fractures by Gustilo-Anderson
What students do: Use "open fracture" as a single category and miss the gradation.
Why it is wrong: Gustilo-Anderson classification guides antibiotic regimen, soft-tissue management, and prognosis. Examiners ask which grade requires which antibiotic.
Correct classification:
| Grade | Wound size | Soft-tissue injury | Contamination | Antibiotic |
|---|---|---|---|---|
| I | Under 1 cm | Minimal | Clean | Cefazolin (1st-gen cephalosporin) |
| II | 1-10 cm | Moderate | Moderate | Cefazolin |
| IIIA | Over 10 cm | Extensive but adequate soft-tissue coverage available | Heavy | Cefazolin + aminoglycoside (gentamicin) |
| IIIB | Over 10 cm | Extensive with periosteal stripping, requires flap | Heavy | Cefazolin + aminoglycoside; consider piperacillin-tazobactam |
| IIIC | Any | Associated arterial injury requiring repair | Variable | Cefazolin + aminoglycoside; consider piperacillin-tazobactam; emergency vascular surgery |
Additional considerations:
- Add penicillin (or metronidazole) for farm/soil contamination (Clostridium prophylaxis)
- Tetanus prophylaxis for all open fractures — booster Td if last dose over 5 years; tetanus immunoglobulin (TIG) if non-immunised or unknown status
- Wound debridement within 6-24 hours; serial debridements as needed
- External fixation for IIIB-IIIC initially; definitive fixation after soft tissue stable
- Soft-tissue coverage with flap within 7 days reduces infection risk in IIIB
Outcomes: IIIB-IIIC have substantially higher rates of infection (15-25 percent), non-union, and amputation (especially IIIC with limb-salvage failure).
MESS (Mangled Extremity Severity Score) ≥7 traditionally predicted amputation in lower limbs with vascular injury; modern data show many limbs with MESS 7-9 can be salvaged with modern microsurgery — score is no longer a strict amputation threshold but informs counselling.
Mistake 14: Skipping the "3 Rs" of fracture management
What students do: Jump to "ORIF" without thinking through the conservative principles.
Why it is wrong: Most fractures are managed by the 3 Rs in a stepwise manner. NEET PG examiners test the conceptual framework.
Correct approach — the 3 Rs of fracture management:
-
Reduction — restoring anatomical alignment
- Closed reduction — manipulation without surgery; under sedation/anaesthesia; for stable, minimally displaced fractures
- Open reduction — surgical exposure; for unstable, intra-articular, irreducible, or complex fractures
-
Retention (immobilisation) — maintaining reduction during healing
- Casts and splints — POP (plaster of Paris), fibreglass; below-elbow, above-elbow, long-leg, short-leg casts
- Traction — skin traction (Buck's, Russell's) or skeletal traction (Steinmann pin, K-wire); temporary stabilisation pre-operatively or definitive for some paediatric femur fractures
- External fixation — for open fractures, polytrauma, IIIB/IIIC open fractures
- Internal fixation (ORIF) — plates and screws, intramedullary nails, K-wires; for unstable, intra-articular, periarticular fractures
-
Rehabilitation — restoring function
- Early range-of-motion exercises (limited by fracture stability)
- Weight-bearing progression (non-weight-bearing → toe-touch → partial → full)
- Strengthening, proprioception, return to sport/work
- Physiotherapy and occupational therapy
Key principle: "Move what you can, don't move what you cannot" — early mobilisation of uninjured joints prevents stiffness; the fractured segment requires immobilisation appropriate to its stability.
Summary — protect your orthopedics marks
The 14 most cost-effective mistakes to fix:
- Colles = dorsal displacement (dinner fork); Smith = volar displacement (garden spade)
- Salter-Harris: SALTR mnemonic; Type II most common; Types III-V need careful follow-up for growth arrest
- Fracture healing: Hematoma → Inflammation → Soft callus → Hard callus → Remodeling
- Dislocation (complete) vs subluxation (partial) vs diastasis (joint separation)
- RA = symmetric small-joint MCP/PIP, raised inflammatory markers, RF+ ; OA = asymmetric large-joint DIP/CMC, normal labs, osteophytes
- Septic arthritis = monoarticular hot joint with fever; URGENT aspiration; Kocher criteria in children
- Compartment syndrome — diagnose on PAIN, not pulses; fasciotomy within 6 hours; pressure over 30 mmHg or delta under 30
- Fat embolism — hypoxia + cerebral signs + petechial rash 24-72 hr after long-bone fracture
- Paediatric fractures: greenstick, torus/buckle, plastic deformation; remodelling potential excellent
- Spondylolysis (pars defect), spondylolisthesis (slip), spondylosis (arthritis) — three different entities
- Ortolani (relocation, abduction) vs Barlow (provocation, adduction); USG before 6 months, X-ray after
- AVN sites: scaphoid proximal pole, femoral head, talus body, lunate; Hawkins classification for talar neck
- Gustilo-Anderson I-IIIC: guides antibiotic and soft-tissue management; tetanus for all
- 3 Rs of fracture management: Reduction → Retention → Rehabilitation
Master these 14 patterns and you protect ~10 marks across orthopedic, radiology, and rheumatology questions in NEET PG 2026.
Frequently Asked Questions
How many orthopedics questions appear in NEET PG?
Orthopedics contributes 8-12 questions per NEET PG paper (2021-2024 paper analysis), including overlap with surgery, radiology, and rheumatology. Question themes cluster around fracture eponyms (Colles, Smith, Monteggia, Galeazzi, Bennett, Boxer's, Jones), Salter-Harris classification, dislocations, paediatric orthopedics (DDH, Perthes, slipped capital femoral epiphysis), compartment syndrome, fat embolism, septic vs reactive vs RA vs OA arthritis, AVN sites, open fracture Gustilo-Anderson classification, spinal disorders (spondylolisthesis, spondylolysis, ankylosing spondylitis), and bone tumours. The 14 mistakes in this guide cover roughly 60-70 percent of typical orthopedic question failures.
What is the difference between Colles and Smith fractures?
Both are distal radius fractures within 2.5 cm of the wrist joint, but with opposite displacement directions. Colles fracture: extra-articular distal radius fracture with DORSAL (posterior) displacement and DORSAL angulation of the distal fragment, producing the classic 'dinner-fork' deformity on lateral view. Mechanism: fall on outstretched hand (FOOSH) with wrist in extension. Commonest in elderly women with osteoporosis. Often associated ulnar styloid fracture (60 percent). Smith fracture (reverse Colles): extra-articular distal radius fracture with VOLAR (anterior) displacement and VOLAR angulation of the distal fragment, producing a 'garden-spade' deformity on lateral view. Mechanism: fall on flexed wrist or backward fall with hand behind. Less common than Colles. Both are typically managed with closed reduction and below-elbow plaster cast; surgical fixation (volar plate or K-wires) for unstable, intra-articular, or significantly displaced fractures, particularly in younger active patients.
What is the Salter-Harris classification of physeal fractures?
The Salter-Harris classification (1963) describes fractures involving the physis (growth plate) in skeletally immature children. Five types — mnemonic SALTR. Type I (S — Slipped/Straight): fracture purely through the physis, no metaphyseal or epiphyseal involvement; typically in young children; good prognosis; can be difficult to see on X-ray (look for widened physis). Type II (A — Above): fracture through the physis extending up into the metaphysis (a triangular metaphyseal fragment called the Thurston-Holland fragment is the key X-ray sign); MOST COMMON type (75 percent of all Salter-Harris); good prognosis. Type III (L — Lower): fracture through the physis extending down into the epiphysis (joint surface); intra-articular, requires anatomical reduction; risk of growth arrest. Type IV (T — Through/Together): fracture through both the metaphysis AND the epiphysis crossing the physis; intra-articular, requires anatomical reduction; high risk of growth arrest. Type V (R — Rammed/Ruined): crush injury to the physis; often missed on initial X-ray; worst prognosis with growth arrest and limb-length discrepancy. Higher types (III-V) have higher risk of premature physeal closure and require careful follow-up.
What are the 5 P's of compartment syndrome and what is the diagnostic threshold?
Compartment syndrome is increased pressure within a closed fascial compartment that exceeds capillary perfusion pressure, leading to ischaemic muscle and nerve necrosis. The classic 5 P's are: Pain out of proportion to injury (the EARLIEST and most sensitive sign — pain on passive stretch of the involved muscles is highly characteristic), Pallor, Paraesthesia, Paralysis (LATE), Pulselessness (VERY LATE — if pulses are absent, severe ischaemia has already occurred). A 6th P (Poikilothermia) is sometimes added. Pulses are typically PRESENT in early compartment syndrome because compartment pressure rarely exceeds systolic blood pressure — DO NOT wait for pulselessness. Diagnosis: clinical with high suspicion. Compartment pressure measurement (Stryker needle) is confirmatory — absolute compartment pressure over 30 mmHg OR delta pressure (diastolic BP minus compartment pressure) under 30 mmHg is diagnostic. Treatment: EMERGENCY fasciotomy within 6 hours — this is a limb-saving emergency. Commonest sites: leg (anterior compartment with deep peroneal nerve, posterior compartment with tibial nerve), forearm (Volkmann ischaemic contracture if missed).
What is the difference between developmental dysplasia of the hip (DDH) Ortolani and Barlow tests?
Both are neonatal physical examination manoeuvres to detect developmental dysplasia of the hip (DDH, previously congenital dysplasia of hip) — performed in newborns before discharge and at 6-week well-baby check. ORTOLANI test (relocation): with the baby supine, hips and knees flexed to 90 degrees, the examiner's middle finger placed over the greater trochanter and thumb on the medial thigh, the hip is ABDUCTED while the greater trochanter is lifted ANTERIORLY — a palpable CLUNK (not click) as the dislocated femoral head relocates into the acetabulum is a positive Ortolani sign, indicating a DISLOCATED but reducible hip. BARLOW test (provocation, opposite direction): with the same starting position, the hip is gently ADDUCTED while applying POSTERIOR pressure on the knee — a palpable clunk as the femoral head dislocates posteriorly out of the acetabulum is a positive Barlow sign, indicating a DISLOCATABLE (unstable) but currently located hip. Both tests become less reliable after 3 months as soft-tissue contractures develop. After 3 months, the screening tests are limited abduction (under 60 degrees, asymmetric), Galeazzi sign (apparent femoral shortening on one side when knees are flexed), and asymmetric thigh creases. Imaging: ultrasound is the investigation of choice from birth to 6 months (Graf alpha angle, Harcke dynamic technique); X-ray pelvis AP is used after 6 months when the femoral head has ossified (Acetabular index, Shenton's line, Hilgenreiner's line, Perkin's line).
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Written by: NEETPGAI Editorial Team Reviewed by: Pending SME Review Last reviewed: May 2026
Ready to put this into practice?
Start practicing NEET PG MCQs with AI-powered explanations.
Start Free PracticeYour Next Step
Related Study Guides
Anxiety Disorders, OCD & PTSD for NEET PG 2026: Diagnosis, SSRI, CBT
Master anxiety, OCD, and PTSD for NEET PG 2026 — DSM-5 criteria, Y-BOCS, SSRI first-line, exposure-response prevention, ECT indications, India NMHS data.
Carbohydrate Metabolism — Glycolysis, TCA, ETC for NEET PG 2026
Master glycolysis, gluconeogenesis, glycogen metabolism, TCA cycle, ETC, oxidative phosphorylation, PPP, and G6PD deficiency for NEET PG 2026 biochemistry.
Cardiovascular Physiology and Cardiac Cycle for NEET PG 2026
Master cardiac cycle, Wiggers diagram, ECG basis, heart sounds, preload-afterload, Starling's law, JVP waves, and CO measurement for NEET PG 2026 — high-yield MCQ traps.
Join our NEET PG community
Daily MCQs, study tips, and topper strategies on Telegram.
Join on Telegram →