Image MCQ Walkthrough: MRI Brain Common Findings — Signal Patterns, Stroke, MS, Tumors, and HSV (NEET PG)
Step-by-step MRI brain interpretation for NEET PG: systematic reading approach across T1, T2, FLAIR, DWI, and contrast sequences; signal patterns (CSF, fat, acute infarct DWI bright/ADC dark, hemorrhage stages); classic patterns — MS (Dawson's fingers), glioblastoma (ring enhancement with necrosis), HSV encephalitis (temporal lobe T2 hyperintensity), brain abscess (ring-enhancing with central DWI restriction), and acute cytotoxic edema in stroke, with a pattern-to-differential comparison table and practice MCQs.
Version 1.0 — Published February 2026
Quick Answer
MRI brain interpretation is pattern recognition built on sequence behavior — signal anchored to CSF reference, diffusion anchored to DWI-ADC pairing, and enhancement anchored to blood-brain-barrier breakdown. To correctly interpret NEET PG MRI brain MCQs, master these 5 pattern groups:
- Sequence identification — CSF dark on T1, bright on T2, dark on FLAIR; fat bright on T1 and T2; DWI bright + ADC dark = true restricted diffusion; post-contrast T1 enhancement = blood-brain-barrier breakdown
- Acute stroke — DWI bright within 30 minutes; ADC dark; FLAIR bright by 6-12 hours; DWI-FLAIR mismatch identifies wake-up-stroke thrombolysis candidates
- Hemorrhage stages — hyperacute (T2 bright), acute (T2 dark), early subacute (T1 bright, T2 dark), late subacute (T1 and T2 bright), chronic (dark rim of hemosiderin)
- Classic patterns — MS with Dawson's fingers (periventricular, perpendicular to ventricles); GBM with thick irregular ring enhancement crossing the corpus callosum; HSV with bilateral asymmetric medial temporal lobe involvement; abscess with thin smooth ring enhancement + central DWI restriction
- Ring-enhancing differential — metastasis, GBM, abscess, toxoplasmosis, tuberculoma, radiation necrosis; DWI pattern (restricted in abscess vs not in tumor), number of lesions, and patient context (HIV, primary cancer) narrow the diagnosis
Clinical image presentation
A 48-year-old previously healthy man presents to the neurology emergency at 10 PM with a 36-hour history of progressively worsening headache, fever (peak 39.2 C), confusion, agitation, and two witnessed generalized tonic-clonic seizures in the last 12 hours. His wife reports that he was entirely normal 48 hours ago. No preceding respiratory or gastrointestinal illness, no recent travel, no immunosuppression, no HIV risk factors. On arrival the patient is GCS 12 (E3 V3 M6), febrile, oriented to person but not to time and place, with no focal motor or sensory deficit, no meningism, pupils equal and reactive.
Initial CT brain is unremarkable. Given the clinical suspicion of infective encephalitis, an urgent contrast-enhanced MRI brain with DWI, FLAIR, T2, post-contrast T1, and SWI sequences is obtained. The study shows:
MRI findings:
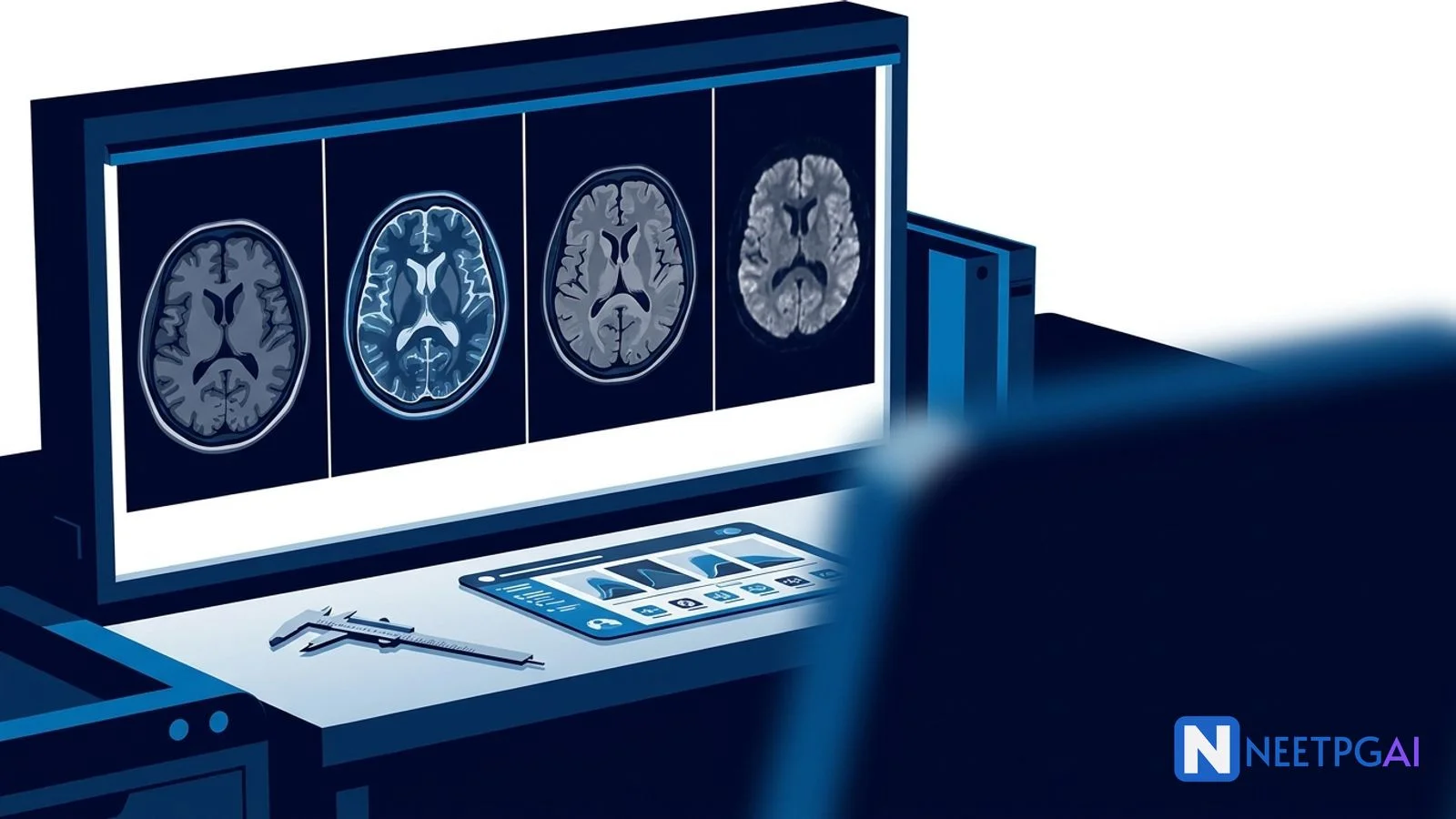
- T2 and FLAIR: bilateral but asymmetric hyperintensity of medial temporal lobes involving both hippocampi (left more than right), parahippocampal gyri, insular cortex, and inferior frontal cortex (cingulate gyrus); cortical ribboning edema pattern
- DWI: corresponding bright signal in the same distribution with dark ADC values — confirms true cytotoxic edema (restricted diffusion)
- SWI / GRE: scattered punctate microbleeds in the affected temporal cortex (petechial hemorrhagic transformation)
- Post-contrast T1: subtle gyriform (ribbon-like) cortical enhancement in left temporal cortex
- Sparing of basal ganglia and putamen — distinguishing feature
- No mass effect, no midline shift, ventricles normal in size
A student reading this image should systematically identify:
Sequence identification:
- CSF dark on T1 and FLAIR, bright on T2 (matches expected)
- DWI bright with ADC dark = cytotoxic edema (acute cellular injury)
- Post-contrast T1 enhancement = blood-brain-barrier disruption
Lesion distribution:
- Bilateral asymmetric medial temporal lobe involvement
- Hippocampi, parahippocampal gyri, insular cortex, inferior frontal cortex
- Cortical and subcortical white matter involvement
- Striking sparing of basal ganglia, putamen, thalami
- No cerebellar or brainstem involvement
Hemorrhagic component:
- Petechial microbleeds on SWI within affected temporal cortex = hemorrhagic encephalitis pattern
Clinical correlation:
- 48-year-old immunocompetent adult
- Acute onset over 36 hours
- Fever + altered mentation + seizures
- Temporal lobe focus clinically (behavioral change, hallucinations) matches imaging
Investigations ordered:
- Lumbar puncture (after MRI, no mass effect or risk of herniation): CSF shows 180 cells/mm3 (lymphocytic predominance), protein 85 mg/dL, glucose 65 mg/dL (normal — ratio above 60 percent of serum glucose), negative Gram stain and bacterial culture; xanthochromia absent
- CSF HSV-1 PCR: positive at 10^5 copies/mL (confirms HSV encephalitis)
- HIV serology: negative
- EEG: periodic lateralized epileptiform discharges (PLEDs) over the left temporal region — highly suggestive of HSV encephalitis
- Empirical IV acyclovir 10 mg/kg every 8 hours was already started before MRI results — correct standard of care
MCQ question as it appears in NEET PG
A 48-year-old previously healthy man presents with 36 hours of fever, confusion, agitation, and two generalized tonic-clonic seizures. MRI brain shows bilateral asymmetric T2 and FLAIR hyperintensity involving both medial temporal lobes and insular cortex with sparing of the basal ganglia; DWI shows restricted diffusion in the same distribution; SWI shows scattered petechial microbleeds in the affected cortex; post-contrast T1 shows subtle gyriform enhancement. Which of the following is the most likely diagnosis and the most appropriate initial management?
- (a) Acute ischemic stroke — IV thrombolysis with alteplase within the 4.5-hour window
- (b) Herpes simplex encephalitis — IV acyclovir 10 mg/kg every 8 hours, started immediately, duration 14-21 days
- (c) Autoimmune limbic encephalitis — IV methylprednisolone and IVIG
- (d) Glioblastoma multiforme — urgent neurosurgical consultation for biopsy and debulking
Take a moment to work through this before reading the analysis below.
Step-by-step visual analysis
A systematic reading protocol is the difference between catching and missing a life-threatening diagnosis on MRI brain. Use this protocol every time an MRI brain image or vignette appears in an NEET PG MCQ.
Step 1: Identify the sequence
Match CSF signal to sequence type.
| Sequence | CSF signal | Fat signal | Best for detecting |
|---|---|---|---|
| T1-weighted | Dark (low signal) | Bright | Anatomy, fat, subacute blood, fat-containing lesions (dermoid, lipoma) |
| T2-weighted | Bright (high signal) | Bright | Edema, inflammation, most pathology, CSF collections |
| FLAIR (fluid-attenuated inversion recovery) | Dark (nulled) | Bright | White matter lesions adjacent to CSF (MS plaques, SAH, cortical edema) |
| DWI (diffusion-weighted imaging) | Usually dark or intermediate | Dark | Acute stroke, abscess, hypercellular tumor, status epilepticus |
| ADC map | Bright | Intermediate | Confirms DWI findings (restricted diffusion = dark ADC) |
| Post-contrast T1 | Dark; enhancing tissue bright | Bright | Blood-brain-barrier breakdown — tumor, infection, active demyelination |
| GRE / SWI | Variable | Intermediate | Hemosiderin, calcification, microbleeds (appear very dark with blooming) |
In this patient: T2/FLAIR bright temporal cortex + DWI bright + ADC dark + SWI dark microbleeds + post-contrast subtle enhancement — consistent with acute cortical inflammatory/infective process with restricted diffusion and hemorrhagic component.
Step 2: Check for mass effect and herniation
Before labeling pathology, ensure no:
- Midline shift (measured at the septum pellucidum level)
- Effacement of basal cisterns or sulci
- Uncal, subfalcine, or transtentorial herniation
- Hydrocephalus (dilated ventricles with transependymal edema)
In this patient: no mass effect, no herniation — lumbar puncture is safe.
Step 3: Identify the lesion distribution
Distribution is the single most powerful clue to diagnosis.
| Distribution | Most likely diagnosis |
|---|---|
| Periventricular ovoid lesions perpendicular to ventricles (Dawson's fingers) | Multiple sclerosis |
| Medial temporal lobes bilaterally, insular cortex, inferior frontal — sparing basal ganglia | HSV encephalitis |
| Butterfly-pattern mass crossing corpus callosum | Glioblastoma |
| Single or multiple round lesions at gray-white junction with extensive vasogenic edema | Metastasis |
| Basal ganglia (bilaterally) with restricted diffusion | Hypoxic-ischemic injury, Creutzfeldt-Jakob, Wilson disease, Leigh syndrome |
| Cortical-subcortical wedge in vascular territory, restricted diffusion | Acute ischemic stroke |
| Multiple ring-enhancing lesions in immunocompromised patient | Toxoplasmosis, primary CNS lymphoma, tuberculoma |
| Cerebellar hemispheres with hyperintense lesions | Cerebellitis, metastasis, hemangioblastoma |
| Sella + suprasellar mass | Pituitary adenoma, craniopharyngioma, Rathke cleft cyst |
In this patient: bilateral asymmetric medial temporal + insular + inferior frontal with basal ganglia sparing = HSV encephalitis.
Step 4: Evaluate DWI and ADC pair
Restricted diffusion (DWI bright + ADC dark) narrows the differential dramatically.
| Cause of restricted diffusion | Clinical context |
|---|---|
| Acute ischemic stroke (cytotoxic edema) | Vascular territory, sudden-onset focal deficit |
| Brain abscess (pus viscosity) | Ring enhancement with central restricted diffusion |
| Hypercellular tumor (lymphoma, high-grade glioma) | Focal mass with variable enhancement |
| HSV encephalitis (cytotoxic + inflammatory edema) | Medial temporal distribution, fever |
| Status epilepticus (cytotoxic edema in involved cortex and thalamus) | Ongoing or recent prolonged seizures |
| Creutzfeldt-Jakob disease (prion-mediated neuronal damage) | Rapidly progressive dementia, cortical ribboning, pulvinar sign in variant CJD |
T2 shine-through gives DWI bright signal without ADC dark — always confirm with ADC before calling restricted diffusion.
In this patient: restricted diffusion in medial temporal cortex supports acute cellular injury pattern, consistent with HSV encephalitis (not T2 shine-through because ADC is dark).
Step 5: Review post-contrast enhancement pattern
| Enhancement pattern | Most likely cause |
|---|---|
| Thick, irregular, heterogeneous ring enhancement | Glioblastoma, high-grade glioma, metastasis |
| Thin, smooth, regular ring enhancement with central DWI restriction | Pyogenic brain abscess |
| Open-ring enhancement (incomplete ring) | Tumefactive demyelinating lesion (atypical MS variant) |
| Punctate or patchy enhancement | Active MS plaques, small metastases, early infection |
| Gyriform (ribbon-like) cortical enhancement | HSV encephalitis (from day 3-7), cortical infarct in subacute phase |
| Leptomeningeal (pial) enhancement | Meningitis, carcinomatous meningitis, neurosarcoidosis |
| Dural (pachymeningeal) enhancement | Hypertrophic pachymeningitis, intracranial hypotension, dural metastasis |
| No enhancement | Acute stroke (enhances from day 3-5), low-grade glioma, cyst, chronic hemorrhage |
In this patient: subtle gyriform cortical enhancement in left temporal cortex, consistent with HSV encephalitis (3-7 day phase).
Step 6: Look for hemorrhage on GRE or SWI
GRE and SWI are exquisitely sensitive to paramagnetic substances (deoxyhemoglobin, methemoglobin, hemosiderin, calcium).
| GRE/SWI finding | Diagnosis |
|---|---|
| Petechial microbleeds in HSV-affected temporal cortex | Hemorrhagic encephalitis (HSV) |
| Lobar microbleeds in elderly with cognitive decline | Cerebral amyloid angiopathy |
| Deep brain microbleeds (basal ganglia, thalami, pons) | Hypertensive microangiopathy |
| Cavernous malformation (popcorn appearance with dark rim) | Cavernoma |
| Susceptibility artifact in vascular territory | Hemorrhagic stroke |
| Multiple small foci of blooming at gray-white junction | Diffuse axonal injury in trauma |
In this patient: petechial microbleeds in affected temporal cortex support HSV encephalitis (which is characteristically hemorrhagic, distinguishing it from limbic encephalitis of autoimmune/paraneoplastic cause).
Answer and detailed explanation
Correct answer: (b) Herpes simplex encephalitis — IV acyclovir 10 mg/kg every 8 hours, started immediately, duration 14-21 days
The MRI pattern in this patient is pathognomonic for HSV encephalitis: bilateral asymmetric medial temporal lobe T2/FLAIR hyperintensity involving hippocampi and insular cortex with sparing of the basal ganglia, accompanied by restricted diffusion on DWI, petechial microbleeds on SWI, and subtle gyriform enhancement on post-contrast T1. Combined with the clinical picture of acute febrile encephalopathy with seizures, CSF lymphocytic pleocytosis, and HSV PCR positivity, the diagnosis is confirmed. HSV-1 causes 95 percent of cases of HSV encephalitis in adults (HSV-2 more often causes neonatal encephalitis and adult meningitis). Untreated mortality is 70 percent; with prompt IV acyclovir started within 48 hours of symptom onset, mortality drops to 5-10 percent with significant improvement in long-term neurologic outcome.
Initial empirical IV acyclovir 10 mg/kg every 8 hours should be started before confirmatory PCR in any patient with suspected HSV encephalitis — delays of even 24 hours worsen outcomes. Duration is 14-21 days, guided by clinical response and repeat CSF PCR if necessary. Adjunctive anti-seizure medications, ICU monitoring, aggressive hydration, and monitoring of renal function (acyclovir crystal nephropathy) are essential.
Why each distractor is wrong:
| Option | Why incorrect |
|---|---|
| (a) Acute ischemic stroke — IV thrombolysis | Ischemic stroke causes restricted diffusion in a vascular territory (MCA, ACA, PCA) — not a bilateral medial temporal + insular + inferior frontal pattern with basal ganglia sparing. Fever, altered mentation, and seizures are uncommon as primary stroke presentation. Thrombolysis is contraindicated in infective encephalitis. |
| (c) Autoimmune limbic encephalitis — methylprednisolone and IVIG | Autoimmune limbic encephalitis (anti-NMDA, anti-LGI1, anti-CASPR2, paraneoplastic) can produce similar medial temporal T2/FLAIR hyperintensity but is typically less hemorrhagic (GRE/SWI normal or minimal microbleeds), less acute (subacute over days to weeks), and CSF HSV PCR is negative. Treatment requires excluding HSV first (untreated HSV is lethal); once excluded, immunotherapy is appropriate. |
| (d) Glioblastoma multiforme — surgery | GBM is a solitary (or less commonly multifocal) heterogeneous mass with thick irregular ring enhancement and extensive peritumoral vasogenic edema, often crossing the corpus callosum in a butterfly pattern. Bilateral medial temporal + insular cortical edema with restricted diffusion and no mass effect is not GBM. |
NEET PG trap alert: The commonest wrong answer in an acute encephalopathy MRI vignette is "autoimmune limbic encephalitis" because both conditions involve the medial temporal lobes. Key distinguishing features: HSV is hyperacute (hours to days) with hemorrhagic microbleeds on SWI and CSF HSV PCR positive; autoimmune limbic encephalitis is subacute (weeks), typically non-hemorrhagic, and associated with specific autoantibodies (anti-NMDA in young women, anti-LGI1 in older adults with faciobrachial dystonic seizures). Always start empirical acyclovir first — missing HSV is lethal; starting acyclovir in non-HSV limbic encephalitis is low-risk.
Practice neurology MCQs with AI-powered explanations to build MRI pattern recognition speed. For a full review of radiology high-yield patterns, see the NEET PG radiology high-yield topics guide and the related CT brain stroke image MCQ walkthrough.
Similar patterns comparison table
The 6 MRI brain patterns most commonly tested in NEET PG — memorize this comparison table, it covers approximately 80 percent of MRI brain image MCQs.
| Pattern | Signature findings | Classic clinical scenario | Management focus |
|---|---|---|---|
| Acute ischemic stroke | DWI bright + ADC dark in vascular territory; FLAIR bright from 6-12 h; GRE dark if hemorrhagic transformation | Sudden-onset focal deficit; time-critical for thrombolysis/thrombectomy | IV alteplase within 4.5 h; mechanical thrombectomy within 6-24 h with DWI-perfusion mismatch |
| Multiple sclerosis (Dawson's fingers) | Periventricular ovoid T2/FLAIR hyperintense lesions perpendicular to ventricles; juxtacortical, infratentorial, spinal cord lesions; gadolinium enhancement in active plaques | Young adult (20-40 years) with optic neuritis, myelitis, or brainstem syndrome; relapsing-remitting course | IV methylprednisolone for acute relapse; DMT (beta-interferons, glatiramer, natalizumab, ocrelizumab) long-term |
| Glioblastoma (GBM) | Thick irregular ring-enhancing mass with central necrosis; butterfly corpus callosum crossing; extensive vasogenic edema | Middle-aged to elderly with progressive focal deficit or seizures over weeks | Maximal safe resection + concurrent radiation + temozolomide (Stupp protocol); MGMT methylation status guides prognosis |
| HSV encephalitis | Bilateral asymmetric medial temporal + insular + inferior frontal T2/FLAIR; restricted diffusion; petechial microbleeds; gyriform enhancement; basal ganglia spared | Acute fever + altered mentation + temporal seizures | IV acyclovir 10 mg/kg every 8 h × 14-21 days; start empirically before PCR |
| Brain abscess | Thin smooth ring-enhancing lesion with central DWI restriction (pus); smooth inner wall and outer capsule | Fever + focal deficit; often with predisposing source (sinusitis, otitis, dental, endocarditis, immunosuppression) | IV antibiotics (ceftriaxone + metronidazole + vancomycin) + surgical drainage if > 2.5 cm |
| Intracranial hemorrhage (dated by signal) | Hyperacute T2 bright; acute T2 dark; early subacute T1 bright T2 dark; late subacute T1 and T2 bright; chronic dark rim on GRE/SWI | Sudden severe headache, focal deficit, hypertension (hypertensive bleed), lobar in amyloid, aneurysmal in SAH | BP control; reversal of anticoagulation; neurosurgical consult for large lobar or cerebellar bleeds; coiling/clipping for aneurysmal SAH |
Clinical application: how to approach an MRI brain image in the exam
The systematic approach below solves 80 percent of NEET PG MRI brain image questions in under 90 seconds.
| Step | Question to ask | Answer narrows to |
|---|---|---|
| 1 | Which sequence is this? (Use CSF as anchor) | T1 dark CSF; T2 bright CSF; FLAIR dark CSF with bright pathology; DWI bright for cytotoxic edema |
| 2 | Is there restricted diffusion? (DWI bright + ADC dark) | If yes → stroke, abscess, hypercellular tumor, HSV, status epilepticus, CJD |
| 3 | What is the lesion distribution? | Vascular territory → stroke; periventricular perpendicular → MS; medial temporal bilateral → HSV; butterfly callosal → GBM |
| 4 | Is there hemorrhage? (GRE/SWI dark blooming) | Petechial in temporal cortex → HSV; deep → hypertensive; lobar in elderly → amyloid |
| 5 | What is the enhancement pattern? (post-contrast T1) | Thick irregular ring → GBM/metastasis; thin smooth ring + DWI restriction → abscess; gyriform → HSV, subacute stroke; leptomeningeal → meningitis |
| 6 | What does the clinical vignette add? | Fever + altered mentation = encephalitis; sudden focal deficit = stroke; immunocompromised + ring lesions = toxo/lymphoma; young woman with optic neuritis = MS |
| 7 | What is the next step in management? | Acute stroke → thrombolysis within 4.5 h; HSV → IV acyclovir; GBM → neurosurgery; abscess → IV antibiotics + drainage; MS → IV steroids |
Frequently asked questions
What is the systematic reading approach for an MRI brain?
Always read an MRI brain with a fixed 6-step sequence to avoid missing findings. Step 1 — identify the sequence on each image (T1, T2, FLAIR, DWI, ADC, post-contrast T1, GRE/SWI) using CSF signal as the reference (CSF is dark on T1, bright on T2, dark on FLAIR). Step 2 — check midline structures for shift, compression, or herniation. Step 3 — review ventricular size (hydrocephalus, atrophy). Step 4 — scan the parenchyma systematically: cortex, white matter, basal ganglia, brainstem, cerebellum. Step 5 — look specifically at the DWI for restricted diffusion (bright DWI with dark ADC = acute stroke, abscess, hypercellular tumor). Step 6 — review post-contrast images for enhancement patterns (nodular, ring, leptomeningeal, dural). Finally, correlate with clinical history — a ring-enhancing lesion in an immunocompromised patient is toxoplasmosis until proven otherwise; the same lesion in a healthy adult is more likely a high-grade glioma or metastasis.
How do you distinguish T1, T2, and FLAIR sequences on MRI brain?
Use CSF signal as the anchor. On T1-weighted images: CSF is dark (low signal), fat is bright, white matter is brighter than gray matter. On T2-weighted images: CSF is bright (high signal), fat is also bright (less so on T2 fat-saturated sequences), gray matter is brighter than white matter. On FLAIR (fluid-attenuated inversion recovery): CSF is dark (nulled by inversion pulse) but other fluid collections and edema remain bright — this is why FLAIR is the best sequence for detecting white matter lesions near CSF spaces (MS plaques, subarachnoid hemorrhage in early acute phase, cortical edema). Mnemonic: on T2 and FLAIR, pathology usually appears bright because edema and gliosis have high water content. T1 post-contrast adds information about blood-brain-barrier breakdown — enhancement indicates active pathology (tumor, active demyelination, infection, metastasis).
What are the MRI signal changes of acute ischemic stroke?
Acute ischemic stroke produces a characteristic MRI signature within minutes to hours. DWI (diffusion-weighted imaging) is the most sensitive sequence — shows hyperintense (bright) signal due to cytotoxic edema restricting water diffusion, visible within 30 minutes of vessel occlusion. ADC (apparent diffusion coefficient) map shows corresponding hypointense (dark) signal — the 'DWI-bright with ADC-dark' pair confirms true restricted diffusion (vs T2 shine-through, which is DWI-bright but ADC-normal). FLAIR may be normal in hyperacute strokes (within 3-4 hours) but becomes hyperintense by 6-12 hours — the 'DWI-FLAIR mismatch' (positive DWI, negative FLAIR) is used to select patients for thrombolysis in wake-up strokes. T2 becomes bright by 12-24 hours. GRE or SWI detects hemorrhagic transformation. Post-contrast enhancement appears from 3-5 days as the blood-brain barrier breaks down.
How do the MRI signal patterns of intracranial hemorrhage evolve over time?
Hematoma signal on MRI evolves predictably as hemoglobin undergoes biochemical changes — a critical dating tool. Hyperacute (below 24 hours, oxyhemoglobin): T1 isointense to slightly hypointense, T2 hyperintense (bright). Acute (1-3 days, deoxyhemoglobin): T1 isointense, T2 hypointense (dark). Early subacute (3-7 days, intracellular methemoglobin): T1 hyperintense (bright), T2 hypointense (dark). Late subacute (1 week to 1 month, extracellular methemoglobin): T1 hyperintense (bright), T2 hyperintense (bright). Chronic (months to years, hemosiderin and ferritin): T1 isointense with dark rim, T2 dark, GRE/SWI strongly hypointense (blooming). Mnemonic — IB GGB ID (Isointense, Bright, Grows darker, Grows brighter on T1; Bright, Dark, Dark, Bright, Dark on T2) — captures the predictable hemoglobin breakdown sequence. GRE and SWI sequences are exquisitely sensitive to hemosiderin and detect old microbleeds that other sequences miss.
What are Dawson's fingers and how do they help diagnose multiple sclerosis on MRI?
Dawson's fingers are periventricular white matter demyelinating lesions that appear perpendicular to the lateral ventricles, extending outward along the medullary perforating veins. They are best seen on sagittal FLAIR sequences as ovoid hyperintense lesions radiating from the corpus callosum into the adjacent white matter. This pattern is highly characteristic of multiple sclerosis (MS) and is one of the McDonald 2017 criteria imaging features for dissemination in space (DIS). Other MS lesion locations that satisfy DIS criteria include juxtacortical or cortical, infratentorial (brainstem, cerebellum), and spinal cord. Dissemination in time (DIT) requires either simultaneous presence of both enhancing and non-enhancing lesions on a single MRI, or a new T2 or enhancing lesion on a follow-up scan. MS plaques typically are ovoid, 3 mm or larger, and involve white matter preferentially — cortical sparing helps distinguish MS from vasculitis or ischemic white matter disease in the elderly.
What is the typical MRI appearance of glioblastoma?
Glioblastoma (GBM, WHO grade IV astrocytoma) has a highly characteristic MRI appearance. T1 shows a heterogeneous mass, often hypointense with central necrosis (darker) and surrounding isointense to hypointense edema. T2 and FLAIR show extensive peritumoral edema (bright) extending far beyond the enhancing tumor margin — this vasogenic edema infiltrates along white matter tracts. Post-contrast T1 shows thick, irregular, heterogeneous ring enhancement surrounding a non-enhancing necrotic core. Restricted diffusion on DWI may be present in hypercellular tumor regions. GBM typically crosses the corpus callosum in a 'butterfly' pattern — this callosal crossing distinguishes it from metastases (which usually do not cross the midline). Spectroscopy shows elevated choline, reduced NAA, and a lactate peak from anaerobic metabolism. The differential for ring-enhancing lesions — GBM, metastasis, abscess, toxoplasmosis, tuberculoma, radiation necrosis — is narrowed by location (cortical, deep), number of lesions, DWI pattern, and patient context (HIV status, immunosuppression, primary cancer).
How does HSV encephalitis appear on MRI?
Herpes simplex virus encephalitis has a pathognomonic MRI pattern — bilateral asymmetric T2 and FLAIR hyperintensity involving the medial temporal lobes (especially hippocampi and parahippocampal gyri), insular cortex, and inferior frontal lobes (cingulate gyrus), with characteristic sparing of the basal ganglia and the putamen. DWI shows restricted diffusion in acutely affected cortex — this is earlier and more sensitive than T2/FLAIR in hyperacute HSV (within 24-48 hours of symptoms). Gyriform (ribbon-like) cortical enhancement may appear on post-contrast T1 from 3-7 days. Hemorrhagic transformation (petechial microbleeds on GRE/SWI) is common and distinguishes HSV from limbic encephalitis of autoimmune or paraneoplastic etiology. Clinical correlation: fever + altered mentation + temporal lobe seizures + the classic MRI pattern = presumptive HSV until CSF PCR confirms; start empirical IV acyclovir 10 mg/kg every 8 hours immediately — delays above 48 hours increase mortality from 5-10 percent to 30-50 percent.
How is MRI brain tested in NEET PG?
NBE tests MRI brain interpretation through five patterns: sequence identification (CSF as anchor — T1 dark, T2 bright, FLAIR dark), acute stroke recognition (DWI bright with ADC dark = cytotoxic edema), hemorrhage dating by signal evolution (hyperacute bright T2 → late subacute bright T1 and T2 → chronic dark rim), pattern-to-diagnosis matching (MS with Dawson's fingers, GBM with butterfly callosal crossing, HSV with medial temporal lobe involvement, abscess with ring enhancement and DWI restriction), and ring-enhancing lesion differential (metastasis, GBM, abscess, toxoplasmosis, tuberculoma, radiation necrosis — context narrows choice). Expect 2-3 MRI brain questions per NEET PG paper in radiology and neurology sections, often as image-based MCQs with a labeled sequence and a clinical vignette.
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Sources and references
- Osborn AG, Hedlund GL, Salzman KL, Osborn's Brain: Imaging, Pathology, and Anatomy, 3rd Edition (Elsevier, 2020) — comprehensive neuroradiology reference with MRI sequence interpretation, stroke imaging, tumor patterns, and demyelinating disease protocols.
- Grossman RI, Yousem DM, Neuroradiology: The Requisites, 4th Edition (Elsevier, 2019) — systematic MRI brain reading approach with classic patterns and differential diagnosis tables for NEET PG preparation.
- Thompson AJ, Banwell BL, Barkhof F, et al. "Diagnosis of multiple sclerosis: 2017 revisions of the McDonald criteria," Lancet Neurology, 2018 — current imaging criteria for MS diagnosis including Dawson's finger recognition and DIS/DIT rules.
Strengthen your MRI brain pattern recognition by working through stroke, MS, tumor, and encephalitis images. Review the radiology subject page, deepen stroke-focused reasoning with the CT brain stroke image MCQ walkthrough, and drill radiology MCQs on the NEETPGAI practice platform. Ready for unlimited AI-powered MCQs with detailed explanations? Explore NEETPGAI Pro.
For personalized study guidance on radiology pattern recognition, try the AI Tutor — it adapts to your weak areas and explains concepts the way a senior resident would.
Written by: NEETPGAI Editorial Team Reviewed by: Pending SME Review Last reviewed: February 2026
This article is reviewed by qualified medical professionals for clinical accuracy and exam relevance. For corrections or updates, contact the editorial team.
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Ready to put this into practice?
Start practicing NEET PG MCQs with AI-powered explanations.
Start Free PracticeYour Next Step
Related Study Guides
Image MCQ: Pediatric Imaging Findings for NEET PG (Intussusception, Pyloric Stenosis, Hirschsprung, VUR, DDH)
5 pediatric imaging MCQs for NEET PG: intussusception target sign, hypertrophic pyloric stenosis string sign, Hirschsprung contrast enema, VUR grading on MCUG, DDH Graf alpha angle.
Image MCQ: Obstetric Ultrasound Findings for NEET PG (Gestational Sac, IUFD, Previa, Abruption, Liquor)
5 obstetric USG image MCQs for NEET PG: gestational sac with yolk sac, IUFD criteria, placenta previa classification, placental abruption, polyhydramnios vs oligohydramnios — pearls and pitfalls.
Image MCQ: Peripheral Blood Smear for NEET PG (AML M3 Auer Rods, CML, ALL, ITP, HUS/TTP)
5 high-yield peripheral blood smear image MCQs for NEET PG: AML M3 (APL) Auer rods + faggot cells, CML granulocyte spectrum, ALL lymphoblasts, ITP megathrombocytes, HUS/TTP schistocytes.
Join our NEET PG community
Daily MCQs, study tips, and topper strategies on Telegram.
Join on Telegram →